108) Posterior Tibial Tendon Dysfunction: The Hidden Cause of Adult Flat Foot Pain
If you’ve developed aching along the inside of your ankle and your arch seems to be collapsing, you might be dealing with posterior tibial tendon dysfunction physiotherapy could help fix. This common but often missed condition is a leading cause of adult flat foot pain — and the earlier you treat it, the better the outcome.
Why Your Arch Is Suddenly Dropping
Adult flat foot doesn’t usually happen overnight. Most people don’t wake up one day with a completely collapsed arch. It’s gradual.
One of the biggest culprits? Posterior Tibial Tendon Dysfunction (PTTD) — now often referred to as Progressive Collapsing Foot Deformity.
The posterior tibial tendon runs from a key calf muscle (tibialis posterior), behind the inside ankle bone, and attaches into the arch of your foot. Its job is simple but critical:
- Support your arch
- Control foot position while walking
- Help you push off when you step
When this tendon becomes overloaded, irritated, or degenerative, it can’t hold the arch up anymore. The result? Pain, weakness, and flattening of the foot.
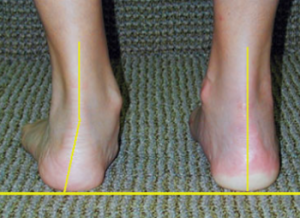
What Is Posterior Tibial Tendon Dysfunction?
Posterior Tibial Tendon Dysfunction is a condition where the tendon gradually becomes:
- Inflamed (early stage)
- Thickened and degenerative
- Weak and unable to support the arch
Over time, this leads to:
- Arch collapse
- Heel drifting outward
- Forefoot turning outward
- Difficulty standing on one leg
- Trouble doing a single heel raise
If untreated, it can become rigid and arthritic.
This is why early posterior tibial tendon dysfunction physiotherapy is crucial.
Who Is Most At Risk?
PTTD is more common in:
- Adults over 40
- Women
- Runners and walkers
- People who stand all day for work
- Those with previous ankle sprains
- People with higher body weight
- Diabetics
We commonly see it in busy tradies, nurses, teachers, and parents who are constantly on their feet.
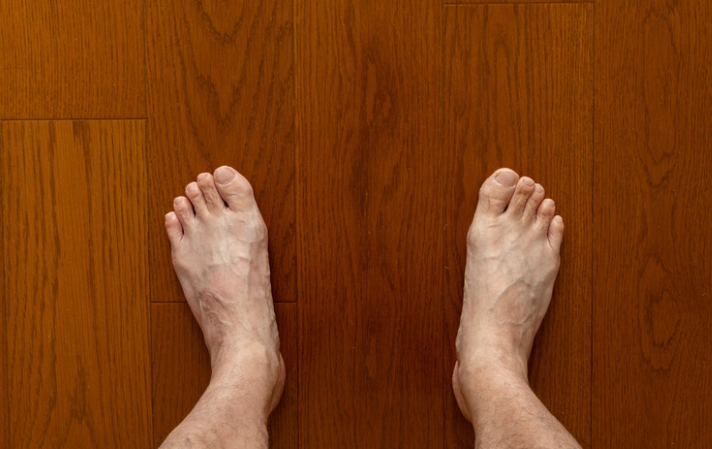
The Early Warning Signs
Most patients tell us:
- “It started as a dull ache along the inside of my ankle.”
- “My foot feels tired and heavy.”
- “My shoes are wearing unevenly.”
- “My arch looks flatter than the other side.”
A big red flag is pain behind the inside ankle bone (medial malleolus) that worsens with walking.
Another key test: try standing on one leg and doing a heel raise. If the heel doesn’t roll inward or you can’t lift at all — that’s often posterior tibial tendon dysfunction.
What Happens If You Ignore It?
Here’s the tough truth.
If untreated, posterior tibial tendon dysfunction can progress through stages:
Stage 1
Painful tendon but normal foot shape.
Stage 2
Arch collapse begins. Foot becomes flexible flat.
Stage 3
Flat foot becomes stiff and arthritic.
Stage 4
Ankle joint involvement develops.
By Stage 3 or 4, surgery is often considered.
This is why conservative management early is so important.
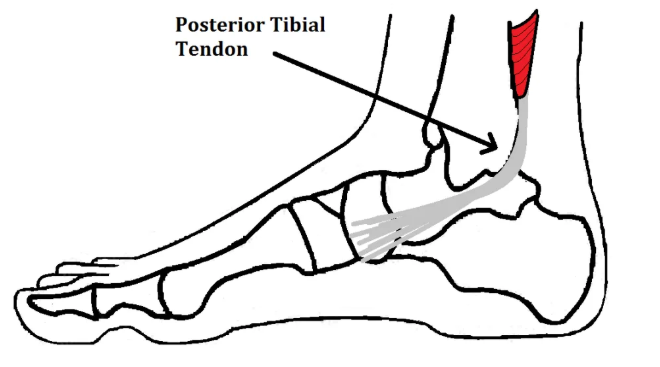
How Physiotherapy Fixes Posterior Tibial Tendon Dysfunction
The good news? Most cases respond very well to targeted physiotherapy.
At our Frenchs Forest clinic, our approach to posterior tibial tendon dysfunction physiotherapy focuses on:
1. Reducing Tendon Load
Early on, we may modify activity and temporarily reduce aggravating loads. That doesn’t mean complete rest — it means smart load management.
2. Strengthening the Tibialis Posterior
The tendon needs progressive loading. Research shows tendons respond positively to the right strengthening program.
Key exercises include:
- Resisted foot inversion
- Heel raises (progressing to single-leg)
- Slow controlled calf raises
- Arch control drills
3. Foot Intrinsic Muscle Training
Strengthening the small stabilisers in the foot helps support the arch naturally.
4. Ankle and Calf Mobility
Restricted ankle dorsiflexion increases strain on the tendon. Improving mobility reduces stress.
5. Taping or Temporary Orthotics
Short-term arch support can unload the tendon while it heals.
6. Gait Retraining
Subtle walking changes can significantly reduce medial foot overload.
A Recent Patient Story (Frenchs Forest NSW)
Recently, we saw a 52-year-old woman who travelled from a surrounding suburb near Frenchs Forest NSW. She works in retail and stands all day.
She came in with:
- 6 months of inner ankle pain
- Progressive flattening of her right arch
- Inability to do a single heel raise
- Increasing difficulty walking more than 20 minutes
She had been told she “just had flat feet.”
After assessment, we diagnosed Stage 2 posterior tibial tendon dysfunction.
Her treatment plan included:
- Load modification (reducing long walking initially)
- Structured strengthening program
- Calf and tibialis posterior progressive loading
- Temporary arch taping
- Education around footwear
Within 4 weeks, pain reduced significantly.
By 8 weeks, she could perform 15 single-leg heel raises.
At 12 weeks, she returned to full work shifts pain-free.
The key? Early, progressive physiotherapy rather than ignoring it or relying purely on passive supports.
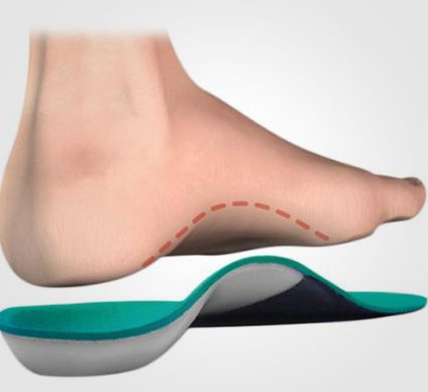
Do Orthotics Fix It?
Orthotics can help — but they are not the full solution.
They reduce strain on the tendon temporarily. However:
- They don’t strengthen the tendon
- They don’t improve muscle control
- They don’t address mobility deficits
The best outcomes occur when orthotics are combined with active rehabilitation.
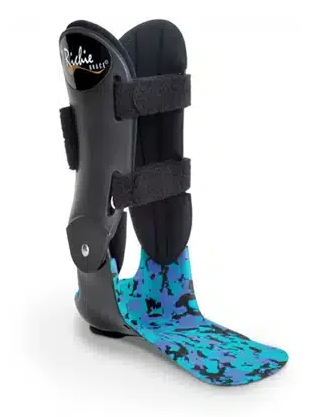
What is a Richie Brace?
In more advanced or stubborn cases, we sometimes discuss the use of a Richie Brace. A Richie Brace is a custom-made ankle-foot orthosis (AFO) that combines a supportive foot orthotic with semi-rigid uprights that stabilise the ankle. It’s typically used in moderate to more advanced posterior tibial tendon dysfunction where the arch is significantly collapsing and the tendon needs substantial offloading. The goal isn’t to rely on it forever — it’s to reduce strain enough to calm symptoms while we continue strengthening and rehabilitation. For some patients, particularly those wanting to avoid surgery, a Richie Brace can be an effective middle-ground option alongside physiotherapy.
Can It Heal Without Surgery?
Yes — especially in Stages 1 and 2.
Evidence supports exercise-based tendon rehab for tendon dysfunction conditions, similar to what we use in Achilles and patellar tendinopathy.
Surgery is usually considered only when:
- Conservative care fails
- Deformity becomes rigid
- Severe arthritis develops
Most people we see respond well to a 8–16 week progressive rehab program.
Footwear Matters More Than You Think
Shoes that are:
- Too flexible
- Worn out
- Completely flat
- Minimal support
can worsen tendon overload.
We often recommend:
- Firm heel counter
- Mild arch support
- Structured midsole
- Avoiding very flexible minimalist shoes during rehab
How Long Does Recovery Take?
It depends on:
- Stage of dysfunction
- Duration of symptoms
- Compliance with rehab
- Body load and activity demands
General guide:
- Mild cases: 6–8 weeks
- Moderate cases: 8–16 weeks
- Chronic cases: 3–6 months
Consistency is key.
Why Early Physiotherapy Matters
The longer you wait:
- The more the arch collapses
- The harder it becomes to reverse
- The greater the risk of joint damage
Early posterior tibial tendon dysfunction physiotherapy can stop progression and restore strength before permanent changes occur.
When Should You Book In?
You should get assessed if:
- You have pain along the inside of your ankle
- Your arch is dropping
- You struggle with heel raises
- Walking distance is reducing
- You’ve had repeated ankle sprains
Don’t wait until it becomes rigid and painful daily.
FAQs – Posterior Tibial Tendon Dysfunction
What is posterior tibial tendon dysfunction?
Posterior tibial tendon dysfunction is a condition where the tendon supporting your arch becomes inflamed or degenerative, leading to adult flat foot and inner ankle pain.
Can physiotherapy fix posterior tibial tendon dysfunction?
Yes. Early-stage PTTD responds very well to progressive strengthening, load management, and foot control retraining.
How long does posterior tibial tendon dysfunction take to heal?
Most cases improve within 8–16 weeks with consistent physiotherapy. More advanced cases may take longer.
Do I need orthotics for posterior tibial tendon dysfunction?
Orthotics can help reduce strain but work best when combined with strengthening and rehabilitation exercises.
Can posterior tibial tendon dysfunction cause permanent flat feet?
If left untreated, it can lead to progressive arch collapse and arthritis. Early treatment reduces this risk significantly.
References
- American Academy of Orthopaedic Surgeons – Posterior Tibial Tendon Dysfunction
https://orthoinfo.aaos.org - Cleveland Clinic – Posterior Tibial Tendonitis
https://my.clevelandclinic.org - Journal of Orthopaedic & Sports Physical Therapy – Tendon Rehabilitation Guidelines
https://www.jospt.org - X-Physio Blog – Snapping Hip Syndrome
https://xphysio.com.au/blog
If you’re noticing arch collapse or inside ankle pain, don’t wait for it to get worse.
Give us a call today on 9806 3077, or book online, just CLICK HERE: https://x-physio.au4.cliniko.com/bookings#service