Muscle knots can feel like tight, painful lumps that just won’t go away—no matter how much you stretch or massage them. If you’re dealing with persistent tension, this guide explains what’s going on and how physio can actually fix it properly.
Muscle Knots Treatment in Frenchs Forest
If you’re searching for muscle knots treatment Frenchs Forest, you’re definitely not alone. We regularly see this issue in clinic across a wide range of patients—from gym-goers and runners to desk workers and tradies.
In Frenchs Forest NSW, muscle knots are one of the most common complaints we treat. Whether it’s neck tension from long hours at a desk, tight calves from running, or shoulder knots from the gym, this is something we deal with every day—and it’s very treatable with the right approach.
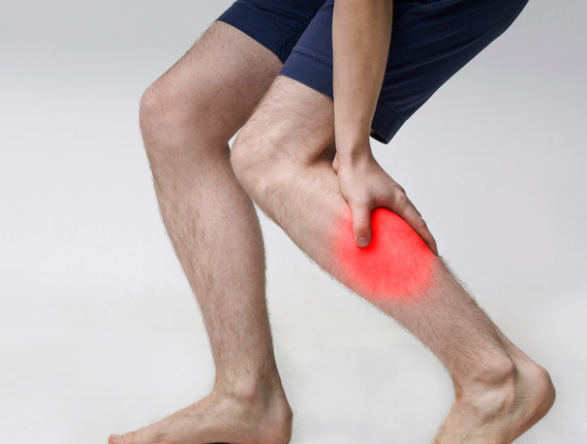
What Are Muscle Knots (Trigger Points)?
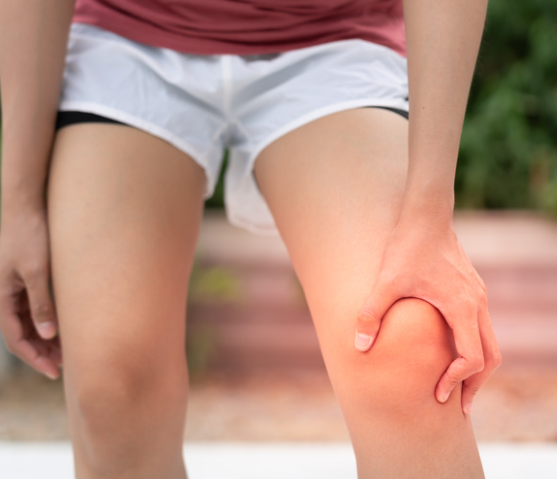
Muscle knots, often called trigger points, are small, tight areas within a muscle that become sensitive and painful. They can feel like a hard lump or band and often cause discomfort both locally and in surrounding areas.
In simple terms, a muscle knot is where part of the muscle fibres have become stuck in a contracted state. This reduces blood flow, increases sensitivity, and creates that familiar tight, aching feeling.
Most patients are surprised that these knots aren’t just “tight muscles”—they’re actually dysfunctional muscle tissue that needs targeted treatment, not just stretching.
Common Symptoms of Muscle Knots
- Localised tenderness or a “lump” in the muscle
- Aching or deep muscle pain
- Pain that spreads (referred pain)
- Stiffness or reduced range of motion
- Pain when pressing on the area
- Muscle fatigue or weakness

What Causes Muscle Knots?
A. General Causes
Muscle knots usually develop due to a combination of factors:
- Overuse or repetitive movements
- Sudden increases in training load
- Poor posture (especially desk work)
- Muscle weakness or imbalance
- Stress and tension
B. 🔥 What We See in Clinic
In our experience, the most common cause we see is a combination of overload and poor muscle control—not just “tightness” on its own.
A mistake we often see is people trying to fix knots purely with stretching or massage guns. While that might feel good short-term, it doesn’t address why the knot formed in the first place.
Most people think muscle knots are caused by dehydration or “toxins”—but actually, they’re usually due to mechanical overload and poor muscle function.
We often find that once we improve strength, movement patterns, and load management, the knots stop coming back.
Can You Keep Training?
The short answer: yes, but it depends.
In many cases, you can keep training—but you may need to modify:
- Intensity
- Volume
- Movement patterns
Pushing through severe pain usually makes things worse, especially if the underlying issue isn’t addressed.
This is where physio becomes the smarter option. Instead of guessing, we can guide you on exactly what to continue, what to modify, and what to temporarily avoid—so you don’t lose progress.
If this sounds like what you’re dealing with, getting on top of it early with physio can make a huge difference.
How Physio Treats Muscle Knots (Step-by-Step)
1. Assessment
We start by identifying:
- Where the trigger points are
- What’s causing them
- Movement or strength issues contributing to the problem
This is key—because treating the knot without fixing the cause usually leads to recurrence.
2. Pain Reduction
We use a combination of:
- Hands-on release techniques
- Dry needling (if appropriate)
- Targeted soft tissue work
This helps reduce pain and relax the muscle quickly.
3. Strength & Rehab
This is where long-term change happens.
We focus on:
- Strengthening weak muscles
- Improving control and coordination
- Fixing posture and movement patterns
In our experience, this is the step most people skip—and it’s why their knots keep coming back.

4. Return to Activity
We guide you back to:
- Gym training
- Running
- Work tasks
…in a way that prevents flare-ups and builds resilience.
Why Rest Alone Doesn’t Fix Muscle Knots
One of the biggest misconceptions is that rest will solve the problem.
While rest might reduce symptoms temporarily, it doesn’t address:
- Muscle weakness
- Movement dysfunction
- Load issues
We often see patients who’ve rested for weeks, only for the knot to return as soon as they resume activity.
The real fix comes from combining treatment with proper rehab.
Real Patient Example
We recently treated a patient from Belrose who came into our Frenchs Forest clinic with persistent upper back and shoulder knots.
He was a desk worker who also trained at the gym 4–5 times per week. He’d tried massage and stretching, but the knots kept coming back.
On assessment, we found:
- Poor upper back strength
- Overactive neck and shoulder muscles
- Limited thoracic mobility
We treated the trigger points with hands-on therapy and dry needling, then introduced a targeted strength program.
Within 3–4 weeks, his pain significantly reduced—and more importantly, the knots stopped recurring.
Most patients are surprised that fixing the cause makes such a big difference compared to just treating the symptoms.
Common Mistakes People Make
- Only using massage or foam rolling
These help temporarily but don’t fix the underlying issue - Ignoring strength training
Weak muscles are a major contributor to trigger points - Training through sharp pain
This can worsen the problem and delay recovery - Poor posture all day
Especially common with desk workers - Not addressing workload
Sudden spikes in activity often trigger knots
Recovery Time
Recovery depends on:
- How long the knot has been there
- Severity
- Underlying causes
Generally:
- Mild cases: 1–2 weeks
- Moderate cases: 3–6 weeks
- Chronic cases: 6+ weeks
In our experience, patients who combine treatment with rehab recover faster and are less likely to have the issue return.
If you’re dealing with muscle knots in Frenchs Forest or nearby areas, our physios can help you recover faster and prevent it from coming back.
Give us a call today on 9806 3077, or book online, just CLICK HERE:
https://x-physio.au4.cliniko.com/bookings#service
FAQs
What is the fastest way to get rid of muscle knots?
The fastest way is a combination of hands-on treatment (like physio or dry needling) and targeted exercises to fix the underlying cause.
Do muscle knots go away on their own?
Some mild knots may settle, but many persist if the root cause isn’t addressed.
Are muscle knots dangerous?
No, but they can become chronic and affect movement, performance, and comfort.
Is massage enough to fix muscle knots?
Massage helps temporarily, but without rehab, the knots often return.
Should I stretch a muscle knot?
Stretching can help, but it’s usually not enough on its own. Strength and control are key.
Internal Links
For more help, explore our physio in Frenchs Forest services:
https://www.xphysio.com.au
You can also read more about related injuries like:
https://xphysio.com.au/10-running-tips-from-a-physio-to-avoid-injury/
References
- Australian Physiotherapy Association – www.physio.asn.au
- Sports Medicine Australia – www.sma.org.au
- Better Health Channel (Victoria) – www.betterhealth.vic.gov.au
Outer ankle pain that just won’t settle can be frustrating—especially when it limits walking, running, or even standing comfortably. Peroneal tendonitis is a common cause we treat in clinic, and the good news is it responds well to the right care. Here’s how physiotherapy can help you recover properly.
Peroneal Tendonitis Treatment in Frenchs Forest
If you’re searching for peroneal tendonitis physiotherapy Frenchs Forest, you’re not alone. We regularly see this condition in runners, gym-goers, tradies, and even people who’ve simply increased their walking or activity levels.
Based in Frenchs Forest NSW, our clinic treats outer ankle pain every week. In our experience, this issue is often misdiagnosed or left too long, which is why early physio can make a big difference.

What is Peroneal Tendonitis?
Peroneal tendonitis refers to irritation or overload of the peroneal tendons, which run along the outside of your ankle and foot. These tendons help stabilise your ankle and control side-to-side movements.
When they become overloaded—often from repetitive stress or sudden changes in activity—they can become painful and inflamed. Most patients are surprised that this condition isn’t just a “sprain” but a load-related issue that needs proper rehab, not just rest.
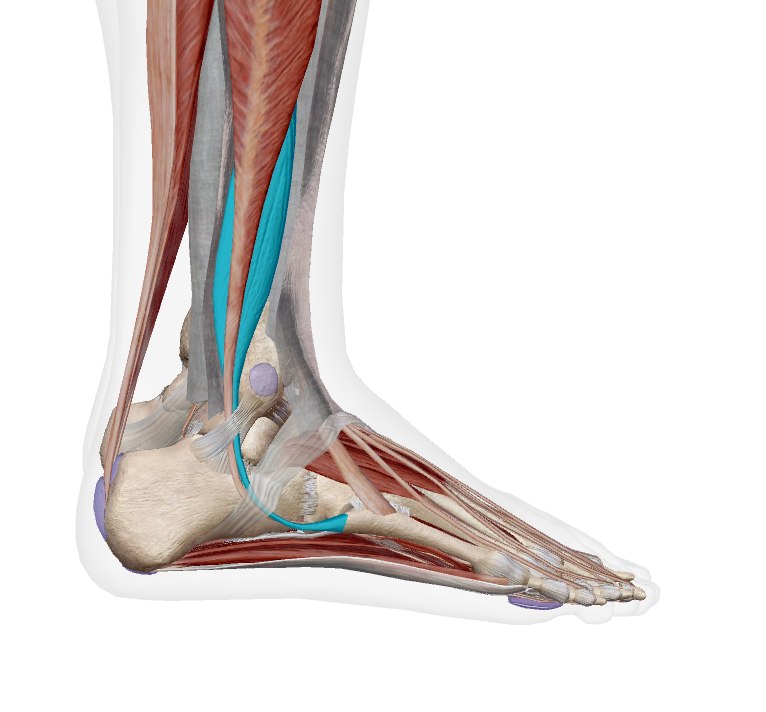
Symptoms of Peroneal Tendonitis
- Pain on the outside of the ankle (especially with walking or running)
- Tenderness behind the ankle bone
- Swelling or stiffness along the outer ankle
- Pain that worsens with activity and eases with rest
- Feeling of weakness or instability in the ankle
What Causes Peroneal Tendonitis?
A. General Causes
- Overuse or repetitive loading
- Sudden increase in training or activity
- Poor footwear or support
- Weakness in ankle or foot muscles
- Previous ankle injuries
B. Clinic Insights
In our experience, the most common cause we see is a sudden spike in activity—like returning to running too quickly or ramping up gym sessions.
A mistake we often see is people treating it like a simple ankle sprain and just resting. While rest can settle symptoms temporarily, it doesn’t address the underlying weakness or loading issue.
Most people think it’s just inflammation, but actually, it’s often a load management problem combined with poor ankle control.
To learn more about ankle sprains CLICK HERE
Can You Keep Training?
The honest answer: it depends.
You don’t always need to stop completely—but you do need to modify. Continuing to push through pain usually prolongs recovery.
In our clinic, we guide patients on how to reduce aggravating movements while keeping them active in safer ways. This is where peroneal tendonitis physiotherapy Frenchs Forest becomes valuable—you’re not guessing what to do.

How Physio Treats Peroneal Tendonitis
1. Assessment
We assess your ankle strength, movement patterns, footwear, and training load. Often, the issue isn’t just the tendon—it’s how your whole lower limb is working.
2. Pain Reduction
This may include:
- Load modification
- Taping or bracing
- Manual therapy
- Advice on footwear
3. Strength & Rehab
This is the most important phase. We focus on:
- Peroneal muscle strengthening
- Calf and foot control
- Balance and stability work
Most patients are surprised that improving strength—not just resting—is what actually fixes the problem.
If this sounds like what you’re dealing with, getting on top of it early with physio can make a huge difference.
4. Return to Activity
We gradually reintroduce running, gym work, or sport with a structured plan. In our experience, this step is often rushed—which is why many people get recurring pain.
Why Rest Alone Doesn’t Fix Peroneal Tendonitis
This is something most blogs miss.
Rest might reduce pain short-term, but it doesn’t improve tendon capacity. Without rebuilding strength and tolerance, the pain often comes straight back when activity resumes.
We often see patients who rested for weeks, felt better, then flared up again immediately when returning to exercise. Proper rehab is what breaks that cycle.

Real Patient Example
We recently treated a runner from Dee Why who came into our Frenchs Forest clinic with persistent outer ankle pain.
They had stopped running for three weeks, but the pain kept returning whenever they tried to get back into it.
On assessment, we found:
- Weak peroneal muscles
- Poor ankle control during running
- A recent increase in training load
We guided them through a structured strengthening program, adjusted their running load, and improved their movement mechanics.
Within 4–6 weeks, they were back to running pain-free—and more importantly, confident it wouldn’t return.
Common Mistakes
- Ignoring the pain early
Waiting too long often makes it harder to settle - Resting without rehab
Symptoms improve, but the problem remains - Returning to sport too quickly
Leads to flare-ups and frustration - Wearing unsupportive footwear
Adds unnecessary stress to the tendon - Trying random exercises online
Without guidance, this can make things worse
Recovery Time
Recovery varies depending on severity and how early treatment starts.
- Mild cases: 2–4 weeks
- Moderate cases: 4–8 weeks
- Longer-standing cases: 8–12+ weeks
In our experience, patients who start physio early tend to recover faster and avoid long-term issues.
Physio in Frenchs Forest – How We Can Help
If you’re dealing with peroneal tendonitis in Frenchs Forest or nearby areas, our physios can help you recover faster and prevent it from coming back.
We focus on not just settling pain, but fixing the underlying cause—so you can get back to running, training, or work without setbacks.
You can learn more about our approach to physio in Frenchs Forest or explore our advice on running injury treatment to stay injury-free.
Give us a call today on 9806 3077, or book online, just CLICK HERE:
https://x-physio.au4.cliniko.com/bookings#service
FAQs
1. What is the fastest way to recover from peroneal tendonitis?
The fastest way is a combination of load management and targeted strengthening through physiotherapy—not just rest.
2. Should I stop running with peroneal tendonitis?
Not always. In many cases, running can be modified rather than stopped completely, depending on pain levels.
3. Can peroneal tendonitis heal on its own?
It can improve, but without addressing the underlying cause, it often returns.
4. Is peroneal tendonitis the same as an ankle sprain?
No. While symptoms can feel similar, tendonitis is usually a load-related issue rather than a ligament injury.
5. Do I need scans for peroneal tendonitis?
Most cases don’t require imaging. A thorough physio assessment is usually enough to diagnose and treat it.
References
- Australian Physiotherapy Association – www.physiotherapy.asn.au
- Sports Medicine Australia – www.sma.org.au
- Better Health Channel (Victoria) – www.betterhealth.vic.gov.auAmerican Academy of Orthopaedic Surgeons – www.aaos.org
Give us a call today on 9806 3077, or book online, just CLICK HERE
https://x-physio.au4.cliniko.com/bookings#service
Bone spurs can be painful, frustrating, and often misunderstood. The good news? Most don’t need surgery. With the right bone spur treatment, you can reduce pain and stay active. If you’re dealing with ongoing joint or tendon pain, this guide will help you understand what’s going on—and what to do next.
Bone Spur Treatment in Frenchs Forest
If you’re searching for bone spur treatment Frenchs Forest, you’re not alone. We regularly treat runners, gym-goers, tradies, and office workers from across Frenchs Forest, NSW dealing with bone spurs in the heel, shoulder, knee, and spine.
In our clinic, this is a very common presentation—especially in people who stay active but have gradually increasing pain. The key thing most patients don’t realise is that the spur itself is rarely the real problem.
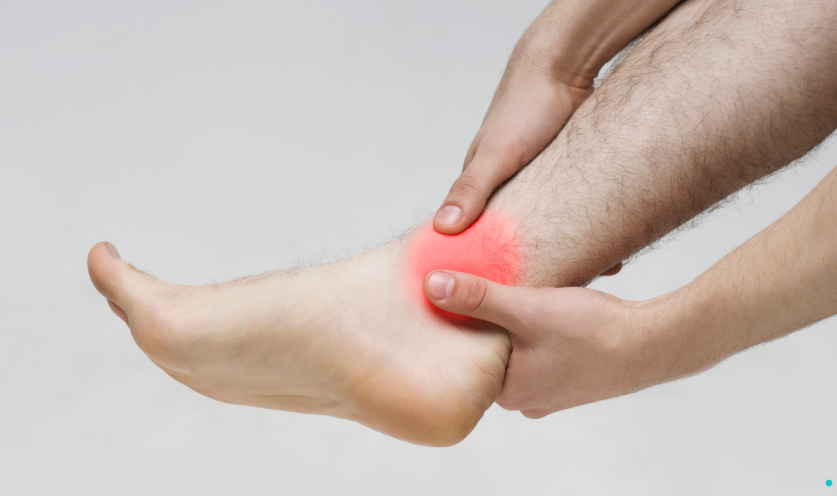
What Is a Bone Spur?
A bone spur (also called an osteophyte) is an extra bit of bone that forms along the edges of joints or where tendons attach. It’s your body’s way of responding to stress, friction, or long-term loading.
They often develop over time and are commonly found in the heel (plantar fascia), shoulder, knee, and spine.
Most patients are surprised that bone spurs themselves aren’t always painful. In fact, many people have them without knowing. Pain usually comes from the surrounding tissues becoming irritated—not the spur itself.
Symptoms
Bone spurs can present differently depending on the location, but common symptoms include:
- Localised pain with movement or load
- Stiffness around a joint (especially in the morning)
- Reduced range of motion
- Pain that builds gradually over time
- Tenderness when pressing on the area
- In some cases, nerve-related symptoms (tingling or weakness)

Causes
General Causes
Bone spurs typically develop due to:
- Repetitive loading or overuse
- Sudden increases in training or activity
- Joint wear and tear over time
- Muscle weakness or poor movement patterns
- Age-related changes
What We See in Clinic (Real Insights)
In our experience, the most common cause we see isn’t just “wear and tear”—it’s poor load management over time.
A mistake we often see is people blaming the spur on scans and thinking it needs to be removed. In reality, we frequently treat patients successfully without touching the spur at all.
Most people think it’s the bone causing the pain—but actually, it’s usually irritated soft tissue around it (like tendons or fascia).
We also often see people rest completely, which actually makes things worse long-term. The body needs the right load—not zero load.
Can You Keep Training?
Short answer: yes—but it depends.
You usually don’t need to stop completely. In fact, staying active (with the right modifications) is often better for recovery.
We guide patients to:
- Reduce aggravating activities temporarily
- Modify training intensity or volume
- Keep moving within a safe pain range
- Gradually reload the affected area
This is where physio becomes crucial—guessing often leads to flare-ups.

How Physio Treats Bone Spurs
1. Assessment
We look beyond the scan.
Your physio will assess:
- Movement patterns
- Strength and flexibility
- Load tolerance
- The actual source of pain
In our experience, this is where most of the answers come from.
2. Pain Reduction
Early treatment focuses on calming symptoms:
- Activity modification
- Manual therapy (if needed)
- Taping or temporary support
- Education around load
3. Strength & Rehab
This is the most important stage.
We build:
- Strength in surrounding muscles
- Tendon capacity
- Joint control and stability
Most patients are surprised how much stronger they need to get to truly fix the issue.
If this sounds like what you’re dealing with, getting on top of it early with physio can make a huge difference.
4. Return to Activity
We gradually reintroduce:
- Running, gym, or work demands
- Sport-specific movements
- Higher loads safely
The goal is not just pain relief—but preventing it from coming back.
Why Rest Alone Doesn’t Fix Bone Spurs
One of the biggest myths is that rest will solve the problem.
While short-term rest can reduce pain, it doesn’t address the underlying issue—load capacity.
In our experience, patients who only rest tend to flare up again as soon as they return to activity.
The real solution is progressive loading—done properly.
Real Patient Example
We recently treated a runner from Oxford Falls who came into our Frenchs Forest clinic with persistent heel pain diagnosed as a heel spur.
They had already tried rest, orthotics, and stretching—but nothing worked long-term.
On assessment, we found:
- Weak calf muscles
- Poor load tolerance in the plantar fascia
- Sudden increase in running volume
We focused on:
- Gradual calf strengthening
- Load management strategies
- Progressive return to running
Within 8 weeks, they were back running pain-free—and importantly, confident it wouldn’t return.
Common Mistakes
- Blaming the scan: The spur isn’t always the pain source
- Resting too much: Leads to weakness and recurrence
- Stretching only: Often not enough without strength work
- Returning too quickly: Causes flare-ups
- Ignoring early pain: Makes it harder to treat later
Recovery Time
Recovery varies depending on:
- Location of the spur
- How long symptoms have been present
- Your activity level
- How well rehab is followed
General guide:
- Mild cases: 4–6 weeks
- Moderate cases: 6–12 weeks
- Long-standing cases: 3+ months
We always aim for steady, sustainable progress—not quick fixes that don’t last.

How We Can Help
If you’re dealing with bone spurs in Frenchs Forest or nearby areas, our physios can help you recover faster and prevent it from coming back. We focus on treating the real cause—not just the symptoms.
Give us a call today on 9806 3077, or book online here:
https://x-physio.au4.cliniko.com/bookings#service
Recommended Reading
If you’re looking for expert physio in Frenchs Forest, visit:
https://www.xphysio.com.au
You may also find this blog helpful:
https://xphysio.com.au/tendonitis-vs-tendinopathy-whats-the-difference/
References
- Australian Physiotherapy Association – https://australian.physio
- Better Health Channel – https://www.betterhealth.vic.gov.au
- Sports Medicine Australia – https://sma.org.au
- Mayo Clinic – https://www.mayoclinic.org
- NHS – https://www.nhs.uk
Give us a call today on 9806 3077, or book online, just CLICK HERE: https://x-physio.au4.cliniko.com/bookings#service
Reactive vs Degenerative Tendinopathy pain that keeps coming back is usually more than just “overuse.” Understanding the difference between reactive and degenerative tendinopathy is the key to fixing it properly. In this guide, we break it down simply—and show how the right physio approach can stop the cycle for good.
At our physiotherapy clinic in Frenchs Forest, NSW, we regularly treat tendon injuries in runners, gym-goers, tradies, and office workers alike. Whether it’s an Achilles flare-up, patellar tendon pain, or shoulder tendinopathy, this pattern of recurring pain is something we see every single week.
Most patients come in frustrated—they’ve rested, stretched, and even tried strengthening, but the pain keeps returning. In our experience, that’s usually because they haven’t been told whether their tendon is in a reactive or degenerative stage.
If you’re looking for expert guidance, you can learn more about our approach to physio in Frenchs Forest here:
https://www.xphysio.com.au
What is Reactive vs Degenerative Tendinopathy?
Tendinopathy is a broad term used to describe tendon pain and dysfunction—but not all tendon injuries are the same.
Reactive tendinopathy is the early stage. It happens when a tendon becomes irritated from a sudden increase in load (like ramping up running or gym training too quickly). The tendon thickens slightly and becomes painful but is still structurally healthy.
Degenerative tendinopathy is more chronic. Over time, repeated overload leads to breakdown in the tendon structure. The tissue becomes weaker, less organised, and more prone to flare-ups.
Most patients are surprised that long-term tendon pain often involves a mix of both—this is why it keeps coming back.
Symptoms
- Pain during or after activity
- Morning stiffness or a “tight” feeling in the tendon
- Pain that warms up, then worsens later
- Localised tenderness when pressing the tendon
- Reduced strength or performance

What Causes Tendinopathy?
General Causes
- Sudden increase in training load
- Repetitive overuse
- Muscle weakness or imbalance
- Poor recovery or sleep
- Biomechanical factors
What We See in the Clinic
In our experience, the most common cause we see is poor load management—not just overuse.
A mistake we often see is patients doing too much rest or jumping into strengthening too quickly—both can make things worse.
Most people think tendon pain is purely inflammatory and needs rest. But actually, tendons respond best to gradual, progressive loading—not complete rest.
We also often find that the pain isn’t just at the tendon. There are usually contributing factors like weak calves, poor hip control, or stiffness elsewhere that keep driving the issue.

Can You Keep Training?
Short answer: it depends—but usually yes, with modification.
Completely stopping activity isn’t always the best solution. In fact, too much rest can make tendons weaker and more sensitive.
Instead, we guide patients to:
- Reduce load (not eliminate it)
- Modify exercises
- Stay within a tolerable pain range
This is where physio becomes crucial—because guessing this yourself often leads to setbacks.
How Physio Treats Tendinopathy
Assessment
We identify whether your tendon is reactive, degenerative, or a mix of both. We also assess strength, movement patterns, and load tolerance.
Pain Reduction
For reactive tendons, we calm things down by adjusting load and using targeted isometric exercises.
Strength & Rehab
This is where most blogs oversimplify things.
We progressively load the tendon using:
- Isometric exercises (early stage)
- Slow heavy resistance training
- Plyometrics (later stage)
In our experience, this phase is where long-term success is built.

Return to Activity
We gradually reintroduce sport or gym work with a structured plan—so you don’t fall back into the same cycle.
If this sounds like what you’re dealing with, getting on top of it early with physio can make a huge difference.
You can also read more about running injury treatment here:
https://xphysio.com.au/10-running-tips-from-a-physio-to-avoid-injury/
Why Rest Alone Doesn’t Fix Tendon Pain
Many people are told to just rest until pain settles. The problem? Tendons don’t heal well with rest alone.
Without proper loading:
- Tendons become weaker
- Pain returns quickly when you restart activity
- The cycle repeats
We often see patients who’ve had months of rest—but still can’t run, squat, or train without pain.
The key is the right load at the right time—not no load.
Real Patient Example
We recently treated a runner from Dee Why who came into our Frenchs Forest clinic with ongoing Achilles pain.
He’d been dealing with it for over 8 months—resting, stretching, and trying random exercises he found online. Every time he returned to running, the pain flared up again.
On assessment, we found a mix of degenerative tendon changes with a reactive flare-up. His calf strength was also significantly reduced.
We:
- Modified his running load
- Introduced isometric calf work initially
- Progressed into heavy strength training
- Built him back into running gradually
Within 8 weeks, he was back running consistently—and more importantly, without flare-ups.
Common Mistakes
- Resting too much – weakens the tendon further
- Jumping into heavy exercises too early – aggravates reactive tendons
- Ignoring pain signals – pushing through often worsens things
- Copying generic rehab programs – not tailored to your stage
- Not addressing contributing factors – like strength or movement issues
Recovery Time
Recovery varies depending on the stage:
- Reactive tendinopathy: 2–6 weeks with proper management
- Degenerative tendinopathy: 3–6+ months
Most patients are surprised that tendon rehab takes time—but when done properly, results are long-lasting.
If you’re dealing with reactive vs degenerative tendinopathy in Frenchs Forest or nearby areas, our physios can help you recover faster and prevent it from coming back.
Give us a call today on 9806 3077, or book online here:
https://x-physio.au4.cliniko.com/bookings#service
FAQs
What is the difference between reactive and degenerative tendinopathy?
Reactive tendinopathy is an early-stage overload response, while degenerative tendinopathy involves longer-term structural breakdown.
Can tendinopathy heal on its own?
It can improve, but without proper rehab, it often returns.
Should I stop exercising with tendon pain?
Not completely. Most cases benefit from modified activity rather than full rest.
How do I know what stage my tendon injury is?
A proper physio assessment is the best way to determine this.
What is the best treatment for tendon pain?
Progressive loading exercises tailored to your specific condition and stage.
References
Australian Institute of Sport – Tendinopathy Guidelines
https://www.ais.gov.au
Cook JL, Purdam CR. Is tendon pathology a continuum? A pathology model to explain the clinical presentation of load-induced tendinopathy
https://bjsm.bmj.com
Sports Medicine Australia – Tendon Injuries
https://sma.org.au
Physiopedia – Tendinopathy
https://www.physio-pedia.com
Recurrent hamstring cramps can be frustrating, unpredictable, and often misunderstood. If your hamstrings keep tightening up during runs, workouts, or even at night, there’s usually more going on than just “tight muscles.” In this guide, we break down the real causes—and how physiotherapy can fix it properly.
At our physiotherapy clinic in Frenchs Forest NSW, recurrent hamstring cramps are something we treat every week. Whether you’re a runner hitting the trails, a gym-goer lifting heavy, or someone just trying to stay active, this issue is incredibly common.
We see it across all age groups—from weekend warriors to office workers who sit all day and then train hard. The good news? Once you understand the cause, it’s very treatable.
What Are Recurrent Hamstring Cramps?
Recurrent hamstring cramps are repeated episodes of sudden, involuntary tightening in the muscles at the back of your thigh. These cramps can happen during activity, after exercise, or even at rest (like during sleep).
Unlike a one-off cramp, recurrent cramps usually point to an underlying issue—whether that’s muscle imbalance, fatigue, or irritation of the nervous system. Most patients are surprised that it’s not just about hydration or stretching.

Symptoms of Recurrent Hamstring Cramps
- Sudden tightness or “grabbing” in the back of the thigh
- Cramping during or after exercise
- Night cramps that wake you up
- Ongoing feeling of tight hamstrings despite stretching
- Reduced performance or fear of pushing hard
Causes of Recurrent Hamstring Cramps
General Causes
- Overuse – too much load without enough recovery
- Sudden increases in training or activity
- Muscle weakness (especially glutes and hamstrings)
- Fatigue from repeated or intense exercise
What We See in the Clinic
In our experience, the most common cause we see isn’t just “tight hamstrings”—it’s a combination of muscle imbalance and nerve irritation.
Most people come in thinking they just need to stretch more, but the cramping keeps coming back. That’s because the hamstring is often overworking due to weak glutes or poor movement patterns.
We also often see subtle irritation of the sciatic nerve. This can make the hamstring more sensitive and prone to cramping—even if the muscle itself is strong.
A mistake we see all the time is people relying only on magnesium, hydration, or stretching. While these can help, they rarely fix the root cause.
Most patients are surprised that it’s not just a muscle problem—it’s often a coordination issue between your nervous system and muscles, especially under fatigue.
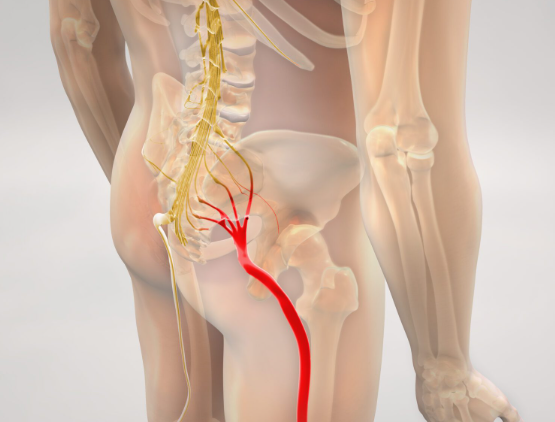
Can You Keep Training?
Short answer: it depends.
In most cases, you can keep training—but you need to modify things:
- Reduce intensity or volume temporarily
- Avoid pushing into cramp territory
- Focus on movement quality
In our experience, completely stopping activity isn’t usually necessary—and can actually slow recovery. The key is getting the right guidance so you don’t keep aggravating the issue.
If this sounds like what you’re dealing with, getting on top of it early with physio can make a huge difference.
How Physio Treats Recurrent Hamstring Cramps
1. Assessment
We look beyond just the hamstring:
- Strength testing (glutes, hamstrings, calves)
- Movement patterns (running, squatting, bending)
- Neural tension (checking for nerve involvement)
This is where we often uncover the real cause.
2. Pain Reduction
- Hands-on treatment to reduce muscle tension
- Gentle mobility work
- Techniques to calm nerve sensitivity
This helps settle symptoms quickly so you can move better.
3. Strength & Rehab
This is the most important stage.
- Targeted hamstring strengthening (not just stretching)
- Glute activation and control
- Core and pelvic stability work
- Gradual exposure to load
In our experience, this is where long-term results happen.
4. Return to Activity
- Gradual return to running, sport, or gym
- Load progression planning
- Technique correction
We make sure you don’t just feel better—you stay better.
Why Rest Alone Doesn’t Fix Hamstring Cramps
Rest might reduce symptoms short-term, but it doesn’t fix:
- Muscle weakness
- Poor movement patterns
- Nerve sensitivity
That’s why cramps often come straight back when you return to activity. Real recovery comes from fixing the underlying cause—not just waiting it out.
Real Patient Example
We recently treated a runner from Dee Why who came into our Frenchs Forest clinic with ongoing hamstring cramps during long runs.
He’d tried stretching daily and taking magnesium, but nothing changed.
After assessing him, we found:
- Weak glutes causing overloading of the hamstrings
- Increased neural tension through the sciatic nerve
We worked on:
- Glute strength and control
- Hamstring loading exercises
- Nerve mobility work
Within 4–6 weeks, his cramping had completely resolved, and he was back to running without fear.
Common Mistakes
- Stretching too much – feels good short-term but doesn’t fix the cause
- Ignoring strength work – weak muscles cramp more easily
- Training through severe cramps – often worsens the issue
- Relying only on supplements – doesn’t address biomechanics
- Missing nerve involvement – a key factor we often see overlooked

Recovery Time for Recurrent Hamstring Cramps
Recovery depends on the cause and how long it’s been going on.
- Mild cases: 2–4 weeks
- Moderate: 4–8 weeks
- Long-standing issues: 8–12+ weeks
In our experience, patients who address the root cause early recover much faster.
Physio in Frenchs Forest for Recurrent Hamstring Cramps
If you’re dealing with recurrent hamstring cramps in Frenchs Forest or nearby areas, our physios can help you recover faster and prevent it from coming back.
Learn more about our services HERE
Explore more injury advice HERE
Give us a call today on 9806 3077, or book online, just CLICK HERE:
FAQs
Why do my hamstrings cramp even when I stretch regularly?
Stretching doesn’t address strength deficits or nerve irritation, which are two of the most common causes.
Are hamstring cramps a sign of injury?
Not always, but recurrent cramps often indicate an underlying issue that should be assessed.
Does magnesium help with hamstring cramps?
It can help in some cases, but in our experience, it rarely fixes the issue on its own.
Can nerve irritation really cause cramps?
Yes—irritation of the sciatic nerve can increase muscle sensitivity and trigger cramping.
Should I stop running if I get hamstring cramps?
Not necessarily. Modifying your training while addressing the cause is usually the best approach.
References
- Australian Physiotherapy Association
https://australian.physio - Sports Medicine Australia
https://sma.org.au - NSW Health
https://www.health.nsw.gov.au - Journal of Orthopaedic & Sports Physical Therapy
https://www.jospt.org - Brukner & Khan’s Clinical Sports Medicine
https://www.mhmedical.com/book.aspx?bookid=2926
Tight muscles aren’t always the problem—sometimes it’s your nerves. Nerve flossing exercises physio targets irritation and tension within the nervous system to reduce pain, pins and needles, and stiffness. In this blog, we’ll show you how it works, when to use it, and how physio can fast-track your recovery.
Why Your Pain Might Not Be a Muscle Problem
Most people assume pain comes from tight muscles or weak joints. And while that’s often true, there’s another major player that gets overlooked: your nervous system.
Your nerves run from your spine all the way to your fingers and toes. They need to glide and move freely through surrounding tissues. When they don’t—due to irritation, inflammation, or compression—you can experience:
- Sharp or burning pain
- Pins and needles
- Numbness
- Tightness that stretching doesn’t fix
- Pain that travels (like down the arm or leg)
This is where nerve flossing exercises physio comes in.

What Are Nerve Flossing Exercises?
Nerve flossing (also called neural gliding or neural mobilisation) involves gentle, controlled movements that help your nerves slide smoothly through surrounding tissues.
Think of it like this:
Your nerve is like a piece of floss running through tight spaces in your body. If it gets stuck, irritated, or compressed, movement becomes painful. Nerve flossing helps “unstick” it.
Unlike traditional stretching:
- You’re not trying to stretch the muscle aggressively
- You’re encouraging movement of the nerve itself
- The movements are gentle and controlled, not forced

Common Conditions That Benefit from Nerve Flossing
Nerve flossing exercises physio can be incredibly effective for:
1. Sciatica
Pain radiating down the leg from the lower back due to irritation of the sciatic nerve.
2. Cervical Radiculopathy
Neck-related nerve pain travelling into the arm.
3. Carpal Tunnel Syndrome
Median nerve compression at the wrist causing tingling in the hand.
4. Thoracic Outlet Syndrome
Compression of nerves around the shoulder and collarbone.
5. Post-Injury or Post-Surgery Stiffness
Scar tissue can restrict nerve movement.
If you’ve ever said, “Stretching doesn’t help my pain”, there’s a good chance the issue might be neural rather than muscular.
How Physiotherapy Uses Nerve Flossing Exercises
At physio, nerve flossing isn’t just handed out as a random exercise—it’s part of a targeted treatment plan.
A physiotherapist will:
- Assess whether your symptoms are nerve-related
- Identify which nerve is involved
- Determine the level of irritation (important!)
- Prescribe the right type and intensity of movement
There’s a big difference between:
- Nerve sliders (gentle, early-stage exercises)
- Nerve tensioners (more advanced loading)
Getting this wrong can flare symptoms—so this is where expert guidance matters.

Real Patient Example (From Our Clinic)
We recently treated a patient who travelled from Oxford Falls to Frenchs Forest NSW with persistent leg pain.
He’d been dealing with what he thought was “tight hamstrings” for months. He’d tried:
- Stretching daily
- Massage
- Foam rolling
Nothing worked.
On assessment, it became clear his symptoms were actually coming from sciatic nerve irritation, not muscle tightness.
We introduced:
- Gentle nerve flossing exercises
- Lumbar mobility work
- Gradual loading through strength exercises
Within 2 weeks:
- Pain reduced significantly
- Mobility improved
- He stopped feeling that constant “pulling” sensation
By 6 weeks, he was back to full activity—pain free.
The key? Treating the nervous system, not just the muscles.
Example Nerve Flossing Exercises
Important: These should be pain-free or only mildly uncomfortable. Sharp pain = stop.
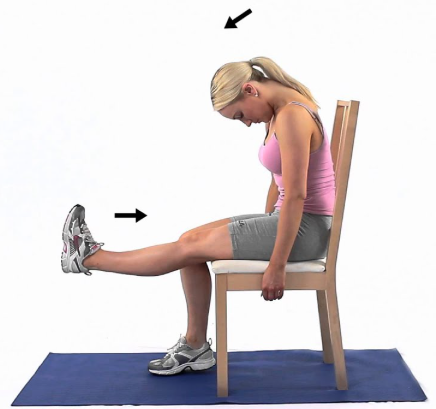
1. Sciatic Nerve Glide (Seated)
- Sit upright
- Straighten one knee while lifting your head up
- Then bend your knee while tucking your chin down
- Repeat 10–15 reps
👉 This creates a sliding motion through the nerve without overloading it.
2. Median Nerve Glide (Arm)
- Arm out to the side, palm facing up
- Slowly extend your wrist and fingers
- Tilt your head away from that arm
- Return to neutral
👉 Great for desk workers with wrist or forearm symptoms.
3. Slump Nerve Glide
- Sit slouched
- Straighten one leg
- Look up as you extend the leg
- Look down as you bend it again
👉 Targets neural tension from the spine down the leg.
When Should You Avoid Nerve Flossing?
Nerve flossing is powerful—but not always appropriate.
Avoid or modify if:
- Pain is severe and highly irritable
- Symptoms worsen after each attempt
- You have progressive neurological symptoms (e.g., worsening weakness)
This is why assessment matters—doing the wrong exercise can aggravate things.
If you have severe nerve pain – READ HERE to learn more
Why Nerve Flossing Works (The Science Bit, Made Simple)
Your nerves need to:
- Slide through surrounding tissues
- Tolerate tension and compression
- Receive good blood flow
When a nerve gets irritated:
- Movement becomes restricted
- Sensitivity increases
- Pain signals amplify
Nerve flossing helps by:
- Restoring mobility
- Reducing sensitivity
- Improving circulation around the nerve
Over time, this calms the system down and restores normal function.
Common Mistakes People Make
If you’ve tried nerve flossing before and it didn’t work, it’s often due to:
❌ Going too hard, too soon
Nerves hate aggressive stretching.
❌ Holding stretches too long
These are dynamic movements, not static holds.
❌ Poor technique
Small changes in head or limb position can completely alter the effect.
❌ Not addressing the root cause
Nerve irritation often stems from the spine or surrounding joints.
How Long Until You See Results?
This depends on:
- Severity of the condition
- How long symptoms have been present
- Consistency with exercises
Typically:
- Mild cases → improvement within 1–2 weeks
- Moderate cases → 3–6 weeks
- Chronic issues → longer, but still very manageable
The key is progressive loading, not just doing the same exercise forever.
Nerve Flossing vs Stretching: What’s the Difference?
| Feature | Stretching | Nerve Flossing |
|---|---|---|
| Target | Muscles | Nerves |
| Sensation | Pulling/stretch | Gentle glide |
| Purpose | Lengthen tissue | Restore movement |
| Approach | Static or dynamic | Controlled, repetitive |
Both have their place—but using the wrong one can slow your recovery.
Why You Should See a Physio First
Google can show you exercises—but it won’t tell you:
- Which nerve is involved
- Whether it’s safe to start
- How far to push it
- What else needs to be treated
That’s where physio comes in.
At X Physio, we combine:
- Hands-on treatment
- Targeted exercise prescription
- Movement retraining
- Education so you understand your injury
So you’re not just guessing—you’re progressing.
Final Thoughts
If your pain:
- Travels
- Feels like burning, tingling, or sharp
- Doesn’t improve with stretching
…it might not be a muscle problem.
Nerve flossing exercises physio could be the missing piece in your recovery.
FAQs
What does nerve flossing feel like?
It should feel like a gentle movement or glide—not a strong stretch. You might feel mild tension, but it shouldn’t be painful.
Can nerve flossing make things worse?
Yes, if done incorrectly or too aggressively. That’s why proper assessment and guidance from a physio is important.
How often should I do nerve flossing exercises?
Usually 1–2 times per day, depending on your condition. Your physio will tailor this to you.
Is nerve flossing the same as stretching?
No. Stretching targets muscles, while nerve flossing targets the movement of nerves through surrounding tissues.
How long does it take for nerve pain to settle?
It varies, but many people see improvement within a few weeks with the right treatment.
References
- https://www.physio-pedia.com/Neural_Mobilisation
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2565076/
- https://www.healthline.com/health/nerve-flossing
- https://www.physio-network.com/blog/neural-mobilisation-explained/
- https://www.spine-health.com/conditions/sciatica/what-you-need-know-about-sciatica
Ready to fix the real cause of your pain—not just the symptoms?
Give us a call today on 9806 3077, or book online, just CLICK HERE: https://x-physio.au4.cliniko.com/bookings#service
Chest pain is scary—no doubt about it. But not all chest pain is heart-related. Costochondritis is a common, treatable condition involving inflammation of the rib joints. The good news? With the right costochondritis physiotherapy, you can reduce pain, restore movement, and get back to normal life faster.
What Is Costochondritis?
Costochondritis is inflammation of the cartilage where your ribs attach to your breastbone (sternum). These joints—called costochondral joints—play a key role in allowing your chest to expand when you breathe.
When they become irritated or inflamed, you can feel sharp, aching, or pressure-like pain in the chest. It often mimics more serious conditions, which is why it can cause a lot of anxiety.

What Does Costochondritis Feel Like?
Costochondritis pain can vary from person to person, but common symptoms include:
- Sharp or aching pain in the front of the chest
- Pain that worsens with deep breathing, coughing, or sneezing
- Tenderness when pressing on the ribs near the sternum
- Pain that increases with movement (especially twisting or lifting)
- Discomfort that may radiate to the shoulder or upper back
A key feature? The pain is usually reproducible with touch or movement, which helps differentiate it from heart-related chest pain.
If the pain is referring down your arm, please read THIS BLOG instead.
What Causes Costochondritis?
There’s often no single clear cause, but several contributing factors can lead to costochondritis:
1. Repetitive Strain
Activities like heavy lifting, gym training, or repetitive upper body movements can overload the rib joints.
2. Poor Posture
Slouched posture—especially from desk work—can place constant stress on the chest wall.
3. Sudden Increase in Activity
Starting a new workout program or increasing intensity too quickly can trigger symptoms.
4. Trauma or Impact
A fall, sporting collision, or even minor trauma can irritate the costochondral joints.
5. Coughing or Respiratory Illness
Persistent coughing (e.g. after a cold) can strain the rib joints and lead to inflammation.

Why It’s Important to Rule Out Serious Causes
Before assuming it’s costochondritis, it’s critical to rule out more serious conditions like heart or lung issues—especially if you experience:
- Chest tightness or pressure with exertion
- Shortness of breath
- Pain spreading to the arm, jaw, or neck
- Dizziness or nausea
If in doubt, always seek medical attention first. Once serious causes are excluded, costochondritis physiotherapy becomes a highly effective treatment pathway.
How Physiotherapy Helps Costochondritis
Physiotherapy is one of the most effective ways to treat costochondritis because it targets the underlying mechanical and movement-related causes.
Here’s how we approach it:
1. Pain Relief Techniques
We start by settling the pain and inflammation through:
- Manual therapy (gentle joint mobilisation)
- Soft tissue release around the chest, shoulders, and upper back
- Advice on activity modification
2. Improving Thoracic Mobility
Stiffness in the upper back (thoracic spine) is a major contributor. If your upper back doesn’t move well, your ribs take on extra load.
We use:
- Mobility exercises
- Stretching techniques
- Hands-on mobilisation
3. Posture Correction
Poor posture is one of the biggest drivers of ongoing symptoms.
We help you:
- Improve sitting and standing posture
- Set up your workstation properly
- Build awareness of daily habits
4. Strengthening Exercises
Weakness in the upper back and shoulder muscles can overload the chest.
Your program may include:
- Scapular stability exercises
- Postural strengthening
- Gradual return-to-loading programs
5. Breathing Retraining
Many people with costochondritis develop shallow or protective breathing patterns.
We guide you through:
- Diaphragmatic breathing
- Rib expansion exercises
- Relaxation strategies

Real Patient Example from Our Clinic
We recently treated a 34-year-old patient who travelled from Dee Why to our clinic in Frenchs Forest, NSW with persistent chest pain.
They had been to the GP and emergency department—thankfully, all cardiac causes were ruled out. However, the pain lingered for over 6 weeks and was affecting sleep, work, and gym training.
On assessment, we found:
- Significant stiffness through the thoracic spine
- Poor posture from long hours at a desk
- Pain reproduced with rib palpation and rotation
We started a structured costochondritis physiotherapy program including:
- Manual therapy to the rib joints and upper back
- Thoracic mobility exercises
- Postural correction strategies
- Gradual return to gym-based loading
Within 2 weeks, their pain had reduced significantly. By week 5, they were back to full training with no symptoms.
How Long Does Costochondritis Take to Heal?
Recovery time varies depending on the severity and how long it’s been present.
- Mild cases: 2–4 weeks
- Moderate cases: 4–8 weeks
- Persistent cases: 2–3+ months
With guided costochondritis physiotherapy, most people recover faster and reduce the risk of recurrence.
What Makes Costochondritis Worse?
If you’re dealing with this condition, try to avoid:
- Heavy lifting (especially pressing movements like bench press)
- Slouched sitting for long periods
- Sudden increases in training load
- Ignoring pain and pushing through
Small adjustments early can make a big difference.

Can You Still Exercise with Costochondritis?
Yes—but it needs to be modified.
We usually recommend:
- Lower body training
- Light cardio (walking, cycling)
- Avoiding aggravating upper body movements
A physio-guided plan ensures you stay active without delaying recovery.
When Should You See a Physio?
You should consider costochondritis physiotherapy if:
- Pain has lasted more than 1–2 weeks
- It’s affecting your daily activities or sleep
- You’re unsure what movements are safe
- Symptoms keep coming back
Early treatment often means faster recovery and less frustration.
Why Choose Physiotherapy Over Rest Alone?
While rest can help settle symptoms temporarily, it doesn’t address the root cause.
Physiotherapy focuses on:
- Fixing movement dysfunction
- Improving strength and posture
- Preventing recurrence
That’s why it’s the most effective long-term solution.
FAQs About Costochondritis Physiotherapy
What is the fastest way to recover from costochondritis?
The fastest way is a combination of relative rest, avoiding aggravating movements, and starting targeted physiotherapy early to improve mobility, posture, and strength.
Can physio fix costochondritis?
Yes. Physiotherapy is one of the most effective treatments, as it addresses the underlying mechanical causes rather than just masking symptoms.
Is costochondritis serious?
It’s not dangerous, but it can be painful and distressing. Always rule out heart-related causes first before confirming the diagnosis.
Should I stretch or rest with costochondritis?
Both are important. Rest initially, but guided stretching and mobility exercises are essential for recovery.
Can poor posture cause costochondritis?
Yes—poor posture places increased stress on the rib joints and is a common contributing factor.
How do I know if my chest pain is costochondritis?
If the pain is reproducible with touch or movement and worsens with certain activities, it may be costochondritis—but always get it checked by a medical professional first.
References
- https://www.healthdirect.gov.au/costochondritis
- https://www.physio-pedia.com/Costochondritis
- https://www.mayoclinic.org/diseases-conditions/costochondritis
- https://www.arthritis.org/diseases/costochondritis
- https://www.ncbi.nlm.nih.gov/books/NBK532931/
Chest pain doesn’t have to mean the worst—but it does deserve the right attention. If you’re dealing with ongoing rib or chest discomfort, a targeted costochondritis physiotherapy plan can make all the difference.
Give us a call today on 9806 3077, or book online, just CLICK HERE:
https://x-physio.au4.cliniko.com/bookings#service
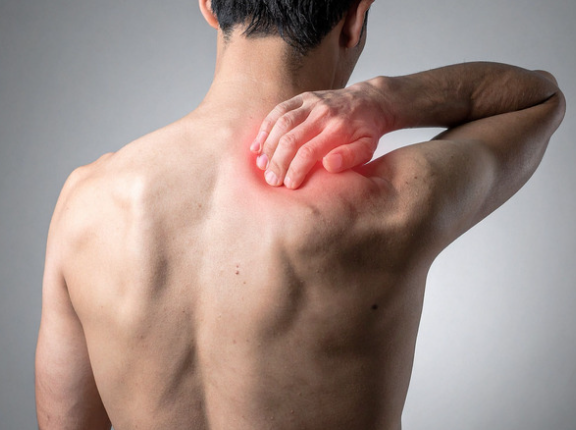
Scapular winging is when your shoulder blade sticks out instead of sitting flat, often causing pain, weakness, and poor movement. The good news? With the right scapular winging physiotherapy, you can restore strength and control. In this blog, we’ll break down causes, symptoms, and exactly how physio can fix it.
Why Your Shoulder Blade Might Be the Real Problem
If you’ve been dealing with shoulder pain that just won’t go away, here’s something most people don’t realise…
👉 It might not actually be your shoulder joint causing the issue.
The scapula (shoulder blade) plays a massive role in how your shoulder moves. When it’s not stable or controlled properly, everything else starts to compensate—and that’s when pain, weakness, and dysfunction creep in.
Scapular winging is one of the clearest signs something isn’t working properly.

What Is Scapular Winging?
Scapular winging happens when the shoulder blade lifts away from the ribcage instead of sitting flat against it.
This creates a noticeable “winging” appearance, especially when you:
- Push against a wall
- Lift your arm overhead
- Carry heavy objects
But beyond how it looks, the real issue is what it does to your movement.
When the scapula isn’t stable, your shoulder loses its foundation—leading to:
- Reduced strength
- Poor control
- Increased injury risk
What Causes Scapular Winging?
Understanding the cause is key to getting the right treatment. Here are the most common reasons we see in clinic:
1. Serratus Anterior Weakness
This is by far the most common cause.
The serratus anterior is the muscle responsible for holding your shoulder blade flat against your ribcage. When it’s weak or not activating properly, the scapula starts to wing.
2. Long Thoracic Nerve Dysfunction
The long thoracic nerve controls the serratus anterior.
If this nerve is irritated or damaged, the muscle won’t function properly—leading to more pronounced winging.
This can happen due to:
- Trauma
- Repetitive overhead activity
- Viral illness
- Post-surgical complications
3. Poor Posture
Long hours sitting at a desk or on your phone can lead to:
- Rounded shoulders
- Tight chest muscles
- Weak upper back muscles
Over time, this creates the perfect environment for scapular winging to develop.
4. Previous Shoulder Injuries
Past injuries like:
- Rotator cuff issues
- Shoulder instability
- AC joint injuries
…can disrupt normal shoulder mechanics and lead to poor scapular control.

Symptoms of Scapular Winging
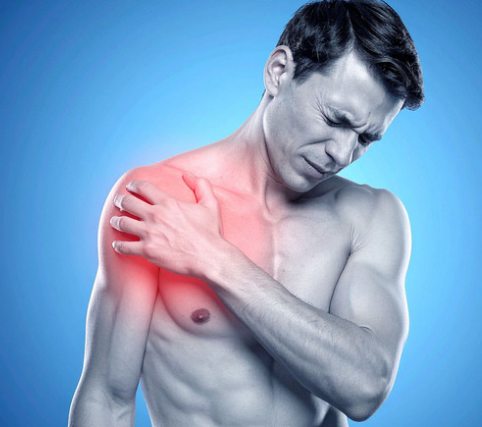
Not everyone notices the winging straight away. Most people come in with symptoms like:
- A dull ache around the shoulder blade
- Pain when lifting overhead
- Weakness when pushing or pulling
- Early fatigue in the upper back
- Clicking or grinding sensations
- Difficulty with gym exercises
A simple test you can try:
👉 Do a wall push-up. If your shoulder blade sticks out noticeably, that’s a strong sign of scapular winging.
Why You Shouldn’t Ignore It
Scapular winging isn’t just a minor issue—it can lead to bigger problems if left untreated.
When your shoulder blade isn’t stable, it affects:
- Rotator cuff function
- Shoulder alignment
- Force production
This increases your risk of:
- Shoulder impingement
- Tendinopathy
- Chronic pain
- Ongoing weakness
Fixing the scapula is often the missing piece in resolving stubborn shoulder pain.
To learn more about shoulder impingement CLICK HERE to read our blog on this.
How Scapular Winging Physiotherapy Fixes the Problem
This is where scapular winging physiotherapy really shines.
The goal isn’t just to strengthen your shoulder—it’s to retrain how your entire shoulder complex works.
1. Activate the Right Muscles
The first step is getting the key stabilisers firing again.
We focus heavily on:
- Serratus anterior
- Lower trapezius
- Middle trapezius
Common exercises include:
- Wall slides with resistance bands
- Push-up plus
- Serratus punches
- Prone Y and T raises
2. Retrain Movement Patterns
Strength alone isn’t enough—you need control.
We work on:
- Timing of muscle activation
- Smooth scapular movement
- Coordination between shoulder and scapula
This is what creates lasting change.
3. Improve Posture and Mobility
We address contributing factors like:
- Tight chest muscles
- Stiff thoracic spine
- Poor desk setup
These small changes can dramatically reduce strain on your shoulder.
4. Hands-On Treatment
Depending on your presentation, we may also use:
- Joint mobilisation
- Soft tissue release
- Dry needling
This helps reduce pain and improve movement more quickly.
5. Gradual Strength Progression
Once control improves, we build strength back into:
- Gym movements
- Overhead activities
- Sport-specific tasks
The goal is to get you back to full function—not just pain-free, but stronger than before.

Real Patient Example (From Our Clinic)
We recently saw a patient in his early 30s who travelled from Belrose to our clinic in Frenchs Forest NSW with ongoing shoulder pain.
He’d been dealing with discomfort for over 6 months, especially during gym workouts—particularly push-ups and overhead pressing.
Previous treatment had focused purely on the rotator cuff, but nothing was improving.
On assessment, it was clear:
👉 Significant scapular winging due to poor serratus anterior activation.
What We Did:
- Targeted serratus anterior strengthening
- Scapular control retraining
- Postural corrections
- Gradual return-to-gym programming
The Outcome:
Within 6 weeks:
- Pain significantly reduced
- Strength improved
- Returned to gym training pain-free
By 10–12 weeks:
- Full return to all activities
- No visible winging during movement
This is a perfect example of how addressing the real cause makes all the difference.
How Long Does Recovery Take?
Recovery depends on the severity and cause:
- Mild cases: 4–8 weeks
- Moderate cases: 8–16 weeks
- Nerve-related cases: several months+
The key?
👉 Consistency with the right exercises.
When Should You See a Physio?
You should get assessed if you have:
- Ongoing shoulder blade pain
- Weakness or instability
- Difficulty lifting your arm
- Visible winging
The earlier you start, the faster you recover.
Final Thoughts
Scapular winging is often the hidden reason behind stubborn shoulder pain and weakness. The good news is that with the right scapular winging physiotherapy, you can restore proper movement, build strength, and get back to doing what you love—without pain holding you back.
FAQs
What is scapular winging?
Scapular winging is when the shoulder blade lifts away from the ribcage instead of sitting flat, often due to muscle weakness or nerve issues.
Can scapular winging be fixed with physiotherapy?
Yes, most cases improve significantly with targeted physiotherapy focusing on strength, control, and movement retraining.
How long does scapular winging take to heal?
Recovery can take anywhere from 4 weeks to several months depending on severity and underlying cause.
Is scapular winging serious?
It can lead to ongoing shoulder pain and dysfunction if left untreated, but is usually very manageable with the right treatment.
What exercises help scapular winging?
Exercises that target the serratus anterior and lower trapezius—like wall slides and push-up plus—are highly effective.
References
- https://www.physio-pedia.com/Scapular_Winging
- https://www.ncbi.nlm.nih.gov/books/NBK541005/
- https://www.jospt.org/
- https://www.shoulderdoc.co.uk/
- https://www.healthline.com/health/scapular-winging
If you’re dealing with shoulder pain, weakness, or think you might have scapular winging, don’t leave it to chance.
Give us a call today on 9806 3077, or book online, just CLICK HERE: https://x-physio.au4.cliniko.com/bookings#service
A high ankle sprain often takes longer to recover than a typical ankle sprain because it involves the ligaments that stabilise the lower leg bones rather than just the ankle joint itself. If you’re struggling with high ankle sprain recovery, the right physiotherapy treatment can speed things up, prevent long-term problems, and get you back to sport or work sooner.
What Is a High Ankle Sprain?
Most people think all ankle sprains are the same. In reality, there are different types.
A high ankle sprain occurs when the ligaments connecting the tibia and fibula (the two bones of the lower leg) are injured. These ligaments are called the syndesmosis and they help stabilise the ankle when you twist, run, or change direction.
This is different from a standard ankle sprain, which usually affects the ligaments on the outside of the ankle.
High ankle sprains commonly occur during:
- Football or rugby tackles
- Sudden twisting while the foot is planted
- Skiing or snowboarding falls
- Running or pivoting sports
- Slipping or awkward landings
Because these ligaments stabilise the entire lower leg, injuries here often take significantly longer to heal.
Why High Ankle Sprain Recovery Takes Longer
A lot of patients ask us the same question:
“Why is my ankle sprain taking so long to heal?”
The answer usually comes down to the type of ligament involved.
1. The Ligaments Are Under Constant Stress
The syndesmosis ligaments hold the tibia and fibula together.
Every time you:
- Walk
- Run
- Jump
- Twist your foot
Those bones naturally separate slightly.
When the ligaments are injured, every step stresses the injury, which slows healing.
2. Poor Blood Supply
Ligaments naturally have less blood supply than muscles, which means slower healing.
The syndesmosis area has even less circulation, which can extend recovery time.
3. The Injury Is Often More Severe
High ankle sprains are commonly seen in contact sports and high-impact injuries.
This often means:
- Greater ligament damage
- More swelling
- More joint instability
In some cases, the injury may even involve a small fracture or severe ligament tear.
4. The Joint Needs Time to Regain Stability
Even after pain settles, the ankle may still feel:
- Weak
- Unstable
- Stiff
- Painful during twisting movements
Without proper rehabilitation, people often return to activity too soon, leading to reinjury.
This is why structured physiotherapy is essential for high ankle sprain recovery.

Symptoms of a High Ankle Sprain
A high ankle sprain can sometimes be mistaken for a regular ankle sprain.
However, there are a few signs that make it different.
Common symptoms include:
- Pain above the ankle joint
- Pain when twisting the foot outward
- Difficulty pushing off when walking
- Swelling in the front of the ankle
- Tenderness between the tibia and fibula
- Pain when walking uphill or running
Many patients also report that walking feels unstable or weak.
If these symptoms persist for more than a few days, it’s worth getting assessed by a physiotherapist.
How Long Does High Ankle Sprain Recovery Take?
Recovery depends on the severity of the ligament injury.
Typical recovery timelines are:
| Injury Severity | Recovery Time |
|---|---|
| Mild syndesmosis sprain | 4–6 weeks |
| Moderate sprain | 6–10 weeks |
| Severe sprain | 10–16+ weeks |
Athletes may require even longer rehabilitation before returning to sport.
Without proper treatment, symptoms can linger for months or even years.
Why Early Physiotherapy Is Important
Many people wait weeks before getting treatment.
Unfortunately, this can slow recovery.
Early physiotherapy helps to:
- Reduce swelling and pain
- Restore ankle movement
- Improve joint stability
- Prevent chronic ankle instability
- Speed up return to sport or work
Early treatment also helps identify whether further scans or specialist care are required.
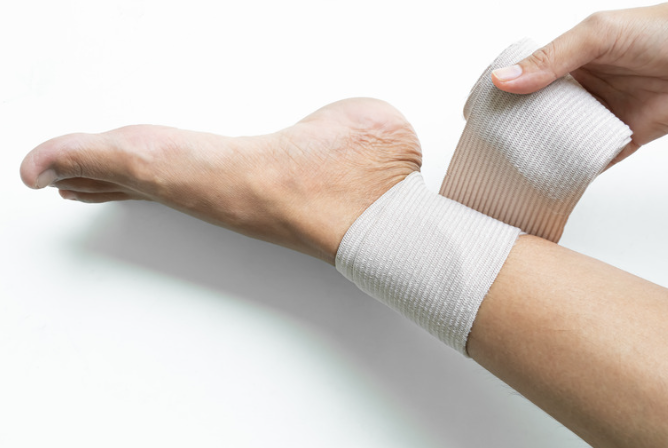
How Physiotherapy Helps High Ankle Sprain Recovery
Physiotherapy focuses on restoring strength, mobility and stability to the ankle.
Treatment usually progresses through several phases.
Phase 1: Pain and Swelling Reduction
Early treatment focuses on calming the injury.
This may include:
- Manual therapy
- Gentle mobility exercises
- Taping or bracing
- Load management advice
Reducing inflammation early helps create the right environment for healing.
Phase 2: Restoring Mobility
Once pain improves, treatment focuses on restoring ankle movement.
Stiffness often develops in the:
- ankle joint
- calf muscles
- surrounding ligaments
Your physio may guide you through:
- ankle mobility drills
- stretching exercises
- joint mobilisation techniques
This helps restore normal movement patterns.
Phase 3: Strength and Stability Training
This stage is essential for preventing reinjury.
Exercises typically include:
- calf strengthening
- balance training
- resistance band exercises
- foot stability drills
These exercises retrain the muscles that protect the ankle during sport and daily activity.
Phase 4: Return to Sport or Activity
The final stage prepares the ankle for higher loads and impact.
This might involve:
- hopping drills
- running progressions
- agility training
- change-of-direction exercises
Returning too early is a common cause of recurrent ankle sprains, so gradual progression is key.
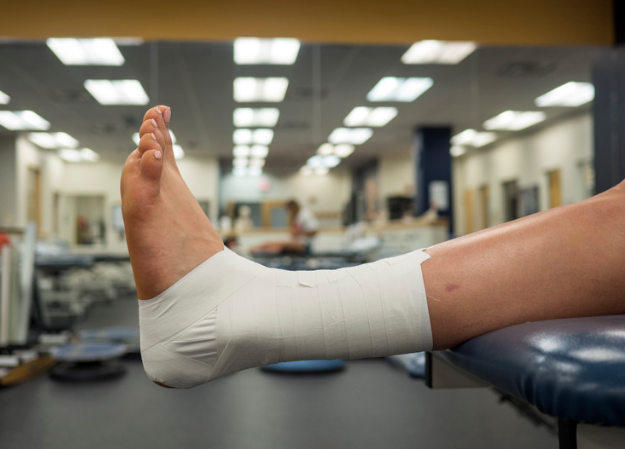
A Recent Patient Success Story
We recently saw a patient in our clinic who had been struggling with high ankle sprain recovery for over six weeks.
He came to see us at X-Physio in Frenchs Forest NSW after injuring his ankle playing social football.
The patient travelled from Belrose, a nearby suburb, because he was frustrated that the pain simply wasn’t improving.
His symptoms included:
- pain above the ankle joint
- difficulty pushing off when walking
- swelling after activity
- weakness during single-leg movements
Assessment confirmed a syndesmosis (high ankle) sprain.
We started a structured physiotherapy program that included:
- ankle joint mobilisation
- strength and stability exercises
- progressive loading
- return-to-running drills
Within three weeks, he reported significant improvements in:
- pain levels
- ankle strength
- walking tolerance
By week five, he had returned to light jogging and training.
This is a great example of how targeted physiotherapy can accelerate high ankle sprain recovery and help patients return to the activities they enjoy.
What Happens If a High Ankle Sprain Is Left Untreated?
Ignoring the injury or returning to activity too early can lead to long-term problems.
Potential complications include:
- chronic ankle instability
- persistent pain
- reduced ankle mobility
- recurring ankle sprains
- early ankle arthritis
Proper rehabilitation dramatically reduces these risks.
When Should You See a Physiotherapist?
You should seek assessment if:
- ankle pain lasts longer than 5–7 days
- swelling keeps returning
- walking is painful or unstable
- sport or exercise aggravates symptoms
- you suspect a high ankle sprain
Early assessment ensures the correct diagnosis and treatment plan.
Key Takeaways
A high ankle sprain is more complex than a standard ankle sprain and often takes longer to heal.
Because the ligaments connect the lower leg bones, they experience stress with every step.
The good news is that physiotherapy can significantly speed up recovery and help prevent long-term ankle problems.
If your ankle sprain isn’t improving as expected, getting the right treatment early can make a huge difference.
FAQs About High Ankle Sprain Recovery
How do I know if I have a high ankle sprain?
High ankle sprains typically cause pain above the ankle joint, particularly when twisting the foot outward or pushing off while walking or running. Swelling and instability may also occur.
How long does high ankle sprain recovery take?
Recovery can take 4–12 weeks depending on the severity of the ligament injury. Severe cases may take longer, particularly for athletes returning to sport.
Can I walk on a high ankle sprain?
Some people can walk, but it is often painful and unstable. Continuing to walk on the injury without proper treatment may delay recovery and worsen ligament damage.
Do high ankle sprains require surgery?
Most high ankle sprains recover with physiotherapy and conservative treatment. Surgery is only required in severe cases where the ligaments are completely torn or the bones become unstable.
Does physiotherapy help high ankle sprain recovery?
Yes. Physiotherapy helps restore mobility, strength, and stability, which speeds recovery and reduces the risk of ongoing ankle problems.
References
- https://www.sportsmedtoday.com/high-ankle-sprains-va-236.htm
- https://my.clevelandclinic.org/health/diseases/21868-high-ankle-sprain
- https://www.physio-pedia.com/Syndesmotic_Ankle_Sprain
- https://www.foothealthfacts.org/conditions/high-ankle-sprain
- https://xphysio.com.au/blog/
Give us a call today on 9806 3077, or book online, just CLICK HERE:
https://x-physio.au4.cliniko.com/bookings#service
Osteopenia is an early stage of bone loss that can quietly increase your risk of fractures if left untreated. The good news? With the right exercise, lifestyle changes, and physiotherapy guidance, you can slow – and sometimes even reverse – bone loss. In this blog, we’ll explain what osteopenia is and how physiotherapy can help keep your bones strong.
What is Osteopenia?
Osteopenia is a condition where bone mineral density is lower than normal, but not low enough to be classified as osteoporosis. To learn more about osteoporosis, read our blog HERE.
Think of it as a warning sign that your bones are starting to lose strength. If nothing is done, osteopenia can progress to osteoporosis, which significantly increases the risk of fractures.
Bones are constantly renewing themselves. Old bone tissue is broken down and replaced with new bone. As we age, the balance can shift so that bone is lost faster than it is rebuilt.
This gradual loss leads to weaker bones.
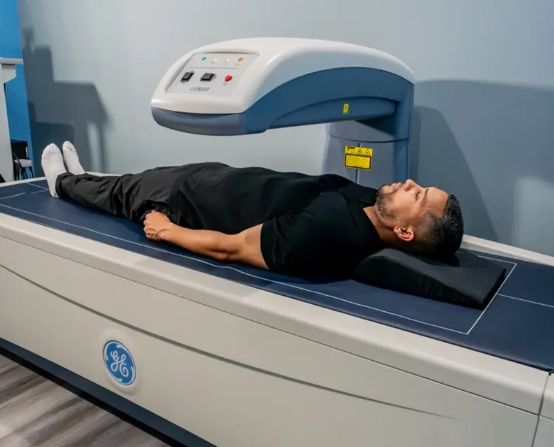
A bone density scan (DEXA scan) measures bone density and gives a T-score:
- Normal: Above -1
- Osteopenia: Between -1 and -2.5
- Osteoporosis: Below -2.5
Many people only discover osteopenia during routine screening or after an unexpected fracture.
The key message is simple: osteopenia is the best time to intervene before major bone loss occurs.
Why Osteopenia Matters
Bone health is often overlooked because osteopenia usually has no symptoms.
You won’t feel your bones getting weaker.
However, the consequences can be serious if bone density continues to decline.
People with osteopenia have an increased risk of:
- Wrist fractures
- Hip fractures
- Spinal compression fractures
- Height loss
- Chronic back pain
Hip fractures in particular can be life-changing and are associated with loss of independence in older adults.
The good news is that bone loss is highly responsive to exercise, which is where physiotherapy plays a major role.
What Causes Osteopenia?
Several factors contribute to reduced bone density.
Ageing
Bone density naturally peaks around age 30. After that, bone loss slowly begins.
Hormonal Changes
Hormonal changes play a major role, particularly after menopause.
Lower oestrogen levels accelerate bone loss in women.
Physical Inactivity
Bones respond to load. Without regular weight-bearing activity, bone strength declines.
Sedentary lifestyles significantly increase the risk of osteopenia.
Poor Nutrition
Bones require key nutrients including:
- Calcium
- Vitamin D
- Protein
- Magnesium
Low intake of these nutrients can contribute to bone loss.
Medical Conditions
Certain conditions increase risk:
- Thyroid disorders
- Rheumatoid arthritis
- Coeliac disease
- Hormonal disorders
Medications
Long-term use of some medications can affect bone density, including:
- Corticosteroids
- Some cancer treatments
- Certain anticonvulsants
Symptoms of Osteopenia
Osteopenia is often called a “silent condition” because symptoms rarely appear until bone loss becomes more severe.
However, some warning signs may include:
- Reduced height
- Poor posture
- Back pain from vertebral compression
- Fractures from minor trauma
Many people are diagnosed after having a DEXA scan recommended by their GP.

How Physiotherapy Helps Osteopenia
Physiotherapy is one of the most effective non-medication treatments for osteopenia.
Exercise stimulates bone cells to produce stronger bone tissue. This process is known as bone remodelling.
When bones experience controlled stress through exercise, they respond by becoming stronger.
A physiotherapy program focuses on several key areas.
1. Weight-Bearing Exercise
Weight-bearing exercises force the skeleton to support body weight.
Examples include:
- Walking
- Stair climbing
- Hiking
- Light jogging
- Dancing
These activities stimulate bone growth in the hips and spine.
2. Resistance Training
Strength training places controlled load through bones via muscles.
Research consistently shows resistance training improves bone density.
Examples include:
- Squats
- Lunges
- Step ups
- Deadlifts
- Resistance bands
- Weight machines
A physiotherapist ensures exercises are performed safely and progressively.
3. Balance Training
Falls are the leading cause of fractures.
Improving balance significantly reduces fracture risk.
Balance training may include:
- Single-leg standing
- Stability exercises
- Core strengthening
- Proprioception drills
4. Posture Correction
Poor posture increases spinal compression forces and fracture risk.
Physiotherapy helps strengthen the muscles that support the spine.
This improves:
- Spinal alignment
- Breathing mechanics
- Overall movement efficiency
5. Education and Lifestyle Advice
Physiotherapists provide guidance on:
- Safe exercise progression
- Activity modifications
- Bone-friendly habits
- Fall prevention strategies
A Real Patient Story From Our Clinic
Recently, we saw a patient named Sarah (name changed for privacy) who travelled from Belrose, a suburb close to Frenchs Forest, after being diagnosed with osteopenia during a routine health check.
She was in her early 60s and had always considered herself relatively active, but a DEXA scan revealed her bone density had dropped into the osteopenia range.
Sarah’s biggest concern was that her mother had suffered a hip fracture in her seventies.
After an initial physiotherapy assessment in Frenchs Forest NSW, we identified several issues:
- Reduced lower limb strength
- Poor single-leg balance
- Forward-rounded posture
- Low confidence with strength training
We designed a structured physiotherapy program focusing on:
- Progressive resistance training
- Hip and spinal loading exercises
- Balance training
- Postural strengthening
Over the next three months, Sarah attended physiotherapy and completed a home exercise program.
The results were excellent.
She reported:
- Improved strength
- Better balance
- Increased confidence with exercise
- No fear of lifting weights
Most importantly, she had developed a long-term exercise routine that will help protect her bones for years to come.
The Best Exercises for Osteopenia
The most effective exercise programs combine three key components.
Strength Training
Strength training should ideally be performed 2–3 times per week.
Key exercises include:
- Squats
- Lunges
- Step-ups
- Deadlifts
- Rows
- Overhead press
These exercises load the skeleton and stimulate bone growth.

Impact Training
Low to moderate impact helps stimulate bone density.
Examples include:
- Brisk walking
- Jogging
- Skipping
- Small jumps
These should be introduced gradually and supervised if needed.
Balance and Stability Work
Improving balance reduces the risk of falls.
Exercises may include:
- Heel-to-toe walking
- Single-leg balance
- Stability ball work
- Core strengthening
Lifestyle Tips to Protect Bone Health
Exercise works best when combined with healthy lifestyle habits.
Calcium Intake
Adults generally require around 1000–1300 mg of calcium per day.
Good sources include:
- Dairy products
- Almonds
- Leafy greens
- Tofu
- Sardines
Vitamin D
Vitamin D helps the body absorb calcium.
Sun exposure and supplementation may be required depending on levels.
Protein Intake
Protein is essential for maintaining bone and muscle.
Include adequate protein with each meal.
Avoid Smoking
Smoking significantly accelerates bone loss.
Limit Alcohol
Excessive alcohol intake negatively affects bone health.
When Should You See a Physiotherapist?
You should consider physiotherapy if:
- You have been diagnosed with osteopenia
- You have low bone density
- You want a safe strength training program
- You have had previous fractures
- You are worried about falls
- You want to prevent osteoporosis
Early intervention can make a huge difference to long-term bone health.
The Takeaway
Osteopenia is a warning sign that your bones need attention, but it is also a valuable opportunity to take action before osteoporosis develops.
With the right physiotherapy program, strength training, and lifestyle changes, you can slow bone loss and significantly reduce fracture risk.
If you’ve recently been diagnosed with osteopenia or want to protect your bone health, physiotherapy can help you develop a safe and effective exercise plan tailored to your needs.
FAQs About Osteopenia
What is osteopenia?
Osteopenia is a condition where bone mineral density is lower than normal but not low enough to be diagnosed as osteoporosis. It is considered an early stage of bone loss and increases the risk of fractures if untreated.
Can osteopenia be reversed?
In many cases, bone density can improve with the right combination of resistance training, weight-bearing exercise, adequate nutrition, and medical management.
What exercises are best for osteopenia?
The most effective exercises include resistance training, weight-bearing activity such as walking, and balance exercises to reduce fall risk.
How is osteopenia diagnosed?
Osteopenia is diagnosed using a DEXA bone density scan, which measures bone mineral density and provides a T-score.
Should people with osteopenia lift weights?
Yes. Strength training is one of the most effective ways to improve bone density. However, exercises should be introduced gradually and ideally under physiotherapy supervision.
References
- Osteoporosis Australia – Bone Health Resources
https://healthybonesaustralia.org.au - Royal Australian College of General Practitioners – Osteoporosis Management
https://www.racgp.org.au - International Osteoporosis Foundation
https://www.osteoporosis.foundation - Mayo Clinic – Osteopenia Overview
https://www.mayoclinic.org - National Institutes of Health – Bone Health and Exercise
https://www.nih.gov
Give us a call today on 9806 3077, or book online, just CLICK HERE
