Knee pain can be a real game-changer – it can stop you from running, squatting, climbing stairs, or even enjoying a simple walk around the block. But here’s the good news: with the right physiotherapy treatment in Frenchs Forest, most knee pain can be managed effectively. In this blog, we’ll cover causes, treatment options, and real results we’ve seen in our clinic.
Why Is Knee Pain So Common?
Knee pain is one of the most frequent reasons people book a physiotherapy appointment. Whether you’re an athlete, a tradie, or simply dealing with everyday wear and tear, your knees take on a lot of load.
Common causes include:
- Overuse injuries – running, cycling, or repetitive kneeling.
- Acute injuries – ACL tears, meniscus injuries, ligament sprains.
- Osteoarthritis – age-related wear and tear of cartilage.
- Patellofemoral pain syndrome (runner’s knee) – pain around the kneecap, often worse with stairs.
- Muscle imbalances – weak glutes or quads leading to poor tracking.
- Post-surgical pain – following arthroscopy, ACL reconstruction, or knee replacement.

Real Patient Success Story – Knee Pain Treatment Near Frenchs Forest
Recently, we treated Sarah, a 42-year-old from Forestville, just minutes from Frenchs Forest. She had ongoing knee pain that was stopping her from playing netball and even walking her dog.
After a detailed physiotherapy assessment, we found her pain was linked to patellofemoral joint irritation caused by weak hip muscles and thigh imbalance.
Her personalised treatment plan included:
- Manual therapy and massage to release tight tissues.
- Targeted strengthening for glutes and quadriceps.
- Knee taping techniques for better tracking.
- Education on training loads and recovery.
✅ Within six weeks, Sarah was back on the netball court – pain-free and stronger than before.
How Physiotherapy Helps with Knee Pain
If you’re searching for “knee pain physio near me” in Frenchs Forest, here’s what to expect from treatment:
Step 1: Comprehensive Assessment
Your physio will check movement, strength, flexibility, and joint mechanics.
Step 2: Hands-On Treatment
This may include joint mobilisation, massage, or dry needling to reduce stiffness and pain.
Step 3: Tailored Exercise Program
Custom rehab exercises address weaknesses and improve long-term joint function. Focus areas often include:
- Glute strengthening
- Quadriceps activation
- Core and balance retraining
Step 4: Load Management
We’ll help you stay active while protecting your knee.
Step 5: Prevention & Education
Learn the best footwear, posture, and activity modifications to stop pain returning.
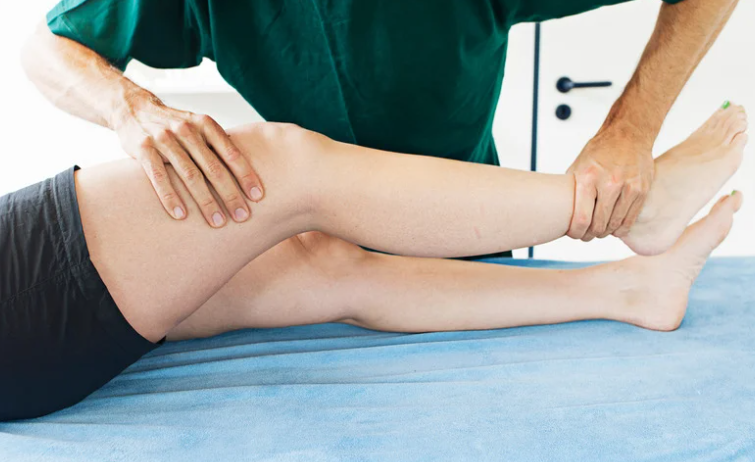
Types of Knee Pain We Treat at X Physio Frenchs Forest
Osteoarthritis of the Knee
- Morning stiffness, grinding, difficulty walking.
- Treatment: Strength training, hydrotherapy, mobility exercises, weight management.
Patellofemoral Pain Syndrome (Runner’s Knee)
- Pain around the kneecap, worse with stairs or squats.
- Treatment: Taping, hip and quad strengthening, movement retraining.
Meniscus Injuries
- Catching, locking, twisting pain.
- Treatment: Stability rehab, gentle loading, post-surgical recovery programs.
- To learn more about meniscus injuries, CLICK HERE
ACL Injuries (Surgical & Non-Surgical)
- Instability, swelling, giving way.
- Treatment: Progressive strength, proprioception training, return-to-sport guidance.
Iliotibial Band Syndrome (ITB Pain)
- Pain on the outer side of the knee.
- Treatment: Tissue release, glute strengthening, running technique correction.

Lifestyle Habits That Worsen Knee Pain
- Sitting too much (weakens supporting muscles).
- Weight gain (adds pressure to joints).
- Poor footwear or worn-out runners.
- Overtraining without recovery.

Self-Management Tips Before Seeing a Physio
- Use ice after flare-ups.
- Wear supportive shoes.
- Strengthen hips and thighs regularly.
- Avoid full rest – keep moving within limits.
- See a physiotherapist early for long-term results.

FAQs – Knee Pain & Physiotherapy
How do I know if my knee pain is serious?
If your knee pain is sudden, severe, or comes with swelling, locking, or giving way, it’s best to see a physiotherapist or GP. Pain lasting longer than a few weeks also needs professional assessment.
Can physiotherapy really help knee arthritis?
Yes. Physiotherapy helps strengthen the muscles around the knee, improve flexibility, and reduce stiffness. Many patients with arthritis report significant pain relief and better mobility with consistent physiotherapy.
Should I rest or exercise with knee pain?
Complete rest often makes knee pain worse. The key is finding the right type and amount of movement. Physiotherapists can guide you with safe, tailored exercises that reduce pain and build strength.
Final Thoughts
Knee pain doesn’t have to control your life. Whether it’s arthritis, sports injuries, or day-to-day aches, physiotherapy offers proven solutions to get you moving again. Just like Sarah from Belrose, you too can bounce back stronger with the right treatment.
👉 Give us a call today on 9806 3077, or book online, just CLICK HERE
References
What is a Meniscus Injury?
A meniscus injury is one of the most common knee problems, affecting people of all ages, from weekend warriors to professional athletes. The meniscus is a piece of cartilage that acts as a cushion between your thigh bone (femur) and shin bone (tibia). It helps absorb shock, stabilise the knee joint, and distribute weight evenly when you move.
Meniscus injuries usually occur when you twist or pivot suddenly. Alternatively, if your knee over bends suddenly, this can often compress and damage the meniscus at the back of your knee. Whereas if the knee hyper extends or straightens suddenly, the meniscus at the front of your knee becomes compressed and possibly damanged. The mechanisms of injury can occur during sports like soccer, netball, or skiing. However, they can also develop gradually due to wear and tear, particularly as we age.
Signs and Symptoms
If you’ve hurt your meniscus, you may experience:
- Pain, especially when twisting or squatting
- Swelling that develops within hours or over a couple of days
- A catching or locking sensation in the knee
- Stiffness and difficulty fully straightening or bending the knee
- A feeling like the knee might give way
How is a Meniscus Injury Diagnosed?
A physiotherapist can often diagnose a meniscus injury based on your mechanism of injury, symptoms and a series of clinical tests. These may involve bending, straightening, and rotating your knee to see if it reproduces your pain. In some cases, an MRI may be needed to confirm the diagnosis and assess the severity of the tear.

Can a Meniscus Heal on Its Own?
It depends on where the tear is located. The outer third of the meniscus has a good blood supply, meaning it has a better chance of healing naturally. However, the inner two-thirds have limited blood flow, making it harder for the body to repair the damage. Even if the tear doesn’t fully heal, many people can manage their symptoms effectively with physiotherapy and avoid surgery altogether.
Physiotherapy Treatment for Meniscus Injuries
1. Reducing Pain and Swelling
In the early stages, managing pain and inflammation is a priority. This may involve:
- Rest and avoiding aggravating activities
- Ice therapy
- Compression and elevation
- Taping or bracing for support
- Crutches are sometimes required to reduce weight bearing
2. Restoring Knee Movement
A stiff knee can make daily activities difficult. Gentle exercises and hands-on therapy help restore flexibility and prevent long-term movement restrictions. This should be replicated at home with a home exercise program that is taught by your physiotherapist.
3. Strengthening the Knee
This is where physiotherapy makes the biggest impact. Strengthening the muscles around the knee, particularly the quadriceps and hamstrings, provides better support and stability to the joint. Below is an example of a structured 16-week strength program:
Weeks 1-4: Foundation Phase (Bodyweight and Low Resistance)
- Bodyweight Squats – 3 sets of 10 reps
- Step-ups (low step) – 3 sets of 10 reps per leg
- Hamstring Bridges – 3 sets of 10 reps
- Calf Raises – 3 sets of 12 reps
- Balance Exercises (Single-leg stand) – 30 seconds per leg
Weeks 5-8: Progression Phase (Introducing Resistance)
- Goblet Squats (Light Dumbbell) – 3 sets of 10 reps
- Step-ups (Higher Step, Weighted if Comfortable) – 3 sets of 10 reps per leg
- Hamstring Curls (Resistance Band or Machine) – 3 sets of 12 reps
- Calf Raises (Weighted) – 3 sets of 12 reps
- Single-leg Balance on Wobble Board – 30 seconds per leg
Weeks 9-12: Strength Phase (Moderate to Heavy Resistance Training)
- Barbell Squats or Leg Press – 3 sets of 8 reps
- Weighted Step-ups (Dumbbells) – 3 sets of 8 reps per leg
- Hamstring Curls (Gym Machine) – 3 sets of 10 reps
- Calf Raises (Smith Machine or Dumbbells) – 3 sets of 10 reps
- Single-leg Deadlifts (Dumbbells) – 3 sets of 8 reps per leg
Weeks 13-16: Advanced Strength & Plyometrics Phase
- Back Squats (Challenging Weight) – 3 sets of 6 reps
- Bulgarian Split Squats (Weighted) – 3 sets of 8 reps per leg
- Romanian Deadlifts (Barbell or Dumbbells) – 3 sets of 8 reps
- Box Jumps or Depth Jumps – 3 sets of 6 reps
- Lateral Hops and Agility Drills – 3 sets of 10 reps

4. Improving Proprioception and Stability
Your knee relies on tiny receptors to sense movement and position. After a meniscus injury, these receptors can be affected, increasing the risk of re-injury. Balance exercises, such as single-leg stands and wobble board drills, help retrain these receptors.
5. Gradual Return to Sport or Activity
Once strength and stability improve, we gradually reintroduce sport-specific movements to ensure you can return safely without risking further injury. For instance, if you played soccer, we would get you on a soccer pitch and attempt to create various drills that mimic a game of soccer to best prepare you before returning to training with your team.
Case Study: How Strength Training Kept the Knee Stable
A recent patient at our clinic, 42-year-old Peter, came in with persistent knee pain after a hiking trip. An MRI showed a degenerative meniscus tear. Initially, Peter struggled with pain and swelling, making it difficult to squat or climb stairs. He was worried that surgery was the only option.
With a structured physiotherapy program, Peter saw gradual improvements. We focused on:
- Reducing swelling with ice, compression, and hands-on treatment
- Gentle range-of-motion exercises to restore movement
- Progressive strength training targeting his quadriceps, hamstrings, and glutes
- Balance and proprioception drills
After three months of consistent rehab, Peter noticed a huge improvement. He was able to return to hiking with minimal discomfort. However, the biggest game-changer was introducing strength training at our gym. Peter now trains regularly, and he’s found that keeping up with his strength program is the only thing keeping his knee symptoms stable. Without it, his pain starts creeping back.

Do You Need Surgery for a Meniscus Tear?
Surgery isn’t always necessary. In fact, research suggests that many people with meniscus injuries recover just as well with physiotherapy compared to surgery (Katz et al., 2013). Surgery may be needed if:
- The knee is locked and won’t straighten
- The tear is large and causing persistent symptoms
- Physiotherapy hasn’t improved symptoms after several months
For most people, strengthening the knee and managing symptoms conservatively leads to great long-term outcomes.
Key Takeaways
- Meniscus injuries are common and can be managed without surgery in most cases.
- Physiotherapy focuses on reducing pain, restoring movement, and strengthening the knee.
- Strength training plays a crucial role in keeping symptoms stable.
- A structured rehab program, like the one Mark followed, can help you return to your normal activities without needing surgery.
If you’re struggling with knee pain and suspect a meniscus injury, book an appointment with our physiotherapists today. We can assess your condition and create a personalised rehab plan to get you back to doing what you love! Give us a call at XPhysio on (02) 9806 3077.
References
- Katz JN, Brophy RH, Chaisson CE, et al. Surgery versus physical therapy for a meniscal tear and osteoarthritis. N Engl J Med. 2013;368(18):1675-1684. Link
- Logerstedt DS, Snyder-Mackler L, Ritter RC, Axe MJ. Knee pain and mobility impairments: meniscal and articular cartilage lesions. J Orthop Sports Phys Ther. 2010;40(6):A1-A35. Link
- American Academy of Orthopaedic Surgeons. Meniscus tears. Link
