Ever felt a lightning bolt shoot from your lower back down your leg? That could be sciatica. In this blog, we’ll explain what causes it, why it hurts so much, and how physio can be a game-changer for your recovery. Read on to discover how we helped a recent patient walk pain-free again.
What Is Sciatica?
Let’s start with the basics. Sciatica refers to pain that travels along the sciatic nerve — the largest nerve in your body. It typically runs from your lower back, through your buttocks, and down each leg.
Sciatica is not a condition in itself, but rather a set of symptoms caused by compression or irritation of the sciatic nerve. The most common culprit? A herniated disc or a bulging disc in your lumbar spine pressing on the nerve.
Common Symptoms of Sciatica
People with sciatica often describe the pain as:
- A sharp, electric-like shooting pain down the back of the leg
- Numbness or tingling
- Muscle weakness in the affected leg
- Lower back pain (sometimes, but not always)
- Pain that worsens when sitting, sneezing, or coughing
And here’s the kicker — the pain often shows up in the leg more than the back, which can confuse people.

What Causes Sciatica?
There are a few common triggers:
- Herniated or Bulging Disc – This is the most common cause. The inner gel of a spinal disc pushes out and compresses the sciatic nerve.
- Spinal Stenosis – Narrowing of the spinal canal can compress nerve roots.
- Piriformis Syndrome – The piriformis muscle in the buttock can irritate the nerve if it tightens or spasms.
- Spondylolisthesis – A vertebra slips forward over the one below it, narrowing the nerve exit space.
- Poor Posture or Prolonged Sitting – Especially with weak core muscles or poor ergonomics.
It can also be worsened by pregnancy, heavy lifting, or even just sitting on your wallet all day (yes, that’s a real thing).
How Physiotherapy Can Help Sciatica
If you’re dealing with sciatica, the right physio treatment can bring major relief. Here’s how we typically approach it:
1. Comprehensive Assessment
We’ll identify the true cause of your sciatic pain — whether it’s coming from a disc, muscle, or spinal joint. This involves checking your posture, movement patterns, muscle strength, and flexibility.
2. Pain Relief Techniques
We use a mix of hands-on therapy and gentle movements to calm the nerve:
- Manual therapy to mobilise stiff joints and reduce nerve irritation
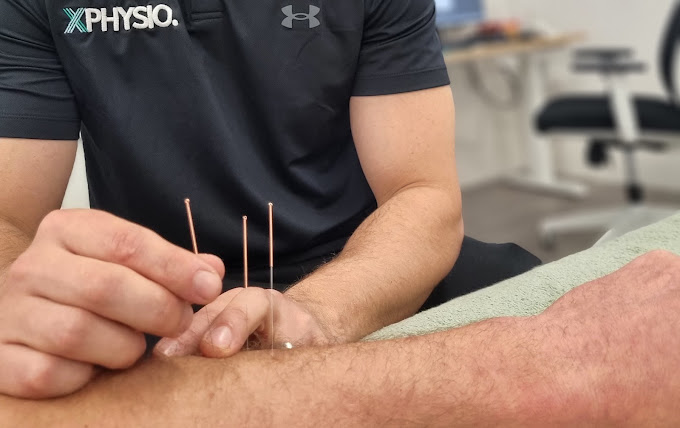
- Dry needling or massage to release tight muscles like the piriformis
- Taping or braces to improve posture or support your back in the early stages
3. Targeted Exercises
Once the acute pain settles, we get you moving with tailored stretches and strength work. This may include:
- Neural glides (nerve flossing) to reduce sensitivity
- Core strengthening to support your lower back
- Glute and hamstring activation to correct movement patterns
- If you are interested in learning more about pilates for core strengthening, CLICK HERE
4. Postural Correction and Ergonomics
We look at how you sit, stand, lift and even sleep. Small tweaks to your workstation or car setup can make a big difference.
5. Education and Prevention
We’ll teach you what to avoid and how to stay active without flaring things up again. Most people improve significantly with the right guidance and rehab plan.

Case Study: From Stuck on the Couch to Back on the Tools
“Rob,” a 42-year-old tradie, came into our clinic in absolute agony. He’d been suffering from lower back and leg pain for about two weeks after lifting heavy timber awkwardly. The pain was sharp and radiated from his glute all the way to his ankle, making it hard to walk, drive, or even put on socks.
He’d already seen his GP and was prescribed painkillers, but the relief was temporary. An MRI confirmed a mild L5-S1 disc bulge compressing the sciatic nerve.
Rob was sceptical at first — he thought he’d be sent home with some stretches and a heat pack. But after his initial assessment, we got to work with a targeted plan:
- Hands-on manual therapy helped reduce the stiffness in his lumbar spine
- Dry needling calmed down his tight piriformis muscle
- We showed him how to do nerve glides safely
- Gradually introduced core exercises like dead bugs and bridges
- Improved his lifting technique and adjusted his ute seat posture
After 3 weeks, Rob could stand and walk without pain. By week 6, he was back on light duties at work. After 8 weeks, he was moving freely and lifting without fear — and he’d tossed the painkillers for good.
He now trains twice a week in our clinic gym to maintain core and glute strength. No relapses. No injections. Just smart rehab.
Why Not Just Rest?
We get it — when your leg feels like it’s on fire, rest seems like the only option. But too much rest can actually slow down your recovery. Sciatic nerve irritation tends to settle faster with gentle movement and guided exercise.
Don’t let fear stop you from moving. A physiotherapist can help you find safe, effective ways to stay active while you heal.
When to See a Physio
If you’re experiencing the following, it’s time to book in:
- Pain that radiates below the knee
- Numbness or tingling in your leg or foot
- Difficulty standing, walking, or sleeping due to pain
- Weakness in the affected leg
- Symptoms persisting for more than a week
The sooner we get started, the sooner you’ll feel better.

Sciatica FAQs
Q: How long does sciatica last?
A: With the right treatment, most cases resolve in 6–8 weeks. Some people improve even faster. Chronic or severe cases can take longer but are still very treatable.
Q: Do I need a scan?
A: Not always. Physiotherapists can often diagnose sciatica based on symptoms and movement tests. Scans are useful if your symptoms aren’t improving, or if there are red flags like severe weakness.
Q: Will I need surgery?
A: Surgery is rarely needed. According to research, most people recover with conservative care like physio (Chou et al., 2018). Surgery is only recommended if there’s major nerve compression or no improvement after months of treatment.
Q: Is sciatica the same as back pain?
A: Not quite. Sciatica can occur with or without back pain. It’s defined more by the radiating nerve pain than by spine pain alone.
The Power of Early Treatment
Early physio intervention can reduce inflammation, calm the nerve, and speed up your recovery. Left untreated, sciatica can lead to more chronic problems like muscle weakness, altered walking patterns, and long-term pain.
You don’t have to suffer through it.
Final Thoughts
Sciatica can be a painful and frustrating experience — but it’s also highly treatable with the right approach. Physio can help you manage pain, restore movement, and get back to doing what you love without relying on medication or surgery.
Whether you’re a tradie like Rob, a desk worker, or a new mum dealing with postural strain, we’ve helped countless people ditch the nerve pain and reclaim their active life.
Don’t let sciatica sideline you. Get expert help today.
Need Help with Sciatica?
Give us a call today on 9806 3077, or book online — just CLICK HERE
References
- Chou, R., et al. (2018). Noninvasive Treatments for Acute, Subacute, and Chronic Low Back Pain: A Clinical Practice Guideline from the American College of Physicians. Annals of Internal Medicine
- Healthdirect Australia. (2023). Sciatica.
- Physiopedia. (2024). Sciatica.
- Better Health Channel – VicGov. (2024). Sciatica.
Let’s get you moving again.
Tennis elbow can strike even if you’ve never touched a racquet. This painful condition affects the outer part of your elbow and can make everyday tasks – like lifting a kettle or typing – feel impossible. In this blog, we’ll break down the causes, symptoms and most effective physiotherapy treatments to help you get lasting relief.
What is Tennis Elbow?
Tennis elbow, or lateral epicondylalgia, is a condition caused by overuse of the forearm muscles that attach to the outside of the elbow. Despite the name, most people who get tennis elbow don’t play tennis. It’s more common in people who do repetitive wrist and hand movements – think tradies, desk workers, baristas, or anyone who loves DIY.
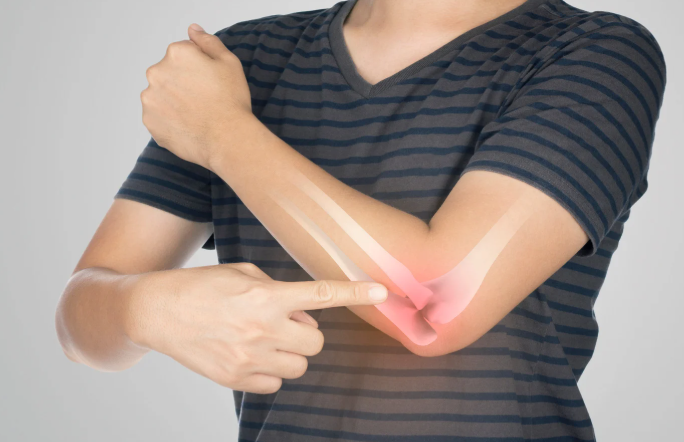
The pain comes from tiny tears and degeneration in the tendons that attach to the lateral epicondyle (the bony bump on the outside of your elbow). It’s your body’s way of saying, “Oi, give this arm a break!”

Symptoms of Tennis Elbow
The most common symptoms include:
- Pain or burning on the outside of the elbow
- Weak grip strength
- Pain that gets worse with wrist or hand activity
- Discomfort when lifting, shaking hands, or turning a doorknob
- Tenderness around the lateral epicondyle
It often develops gradually, starting as a niggle and turning into a full-blown ache that doesn’t go away.
Common Causes
Tennis elbow typically comes from:
- Repetitive motions like typing, painting, plumbing, using a screwdriver
- Poor lifting technique (especially twisting motions with the wrist)
- Overtraining without adequate recovery – common in gym-goers and athletes
- Poor posture, especially if you’re at a desk all day
- Sudden increase in activity levels (e.g., weekend warriors doing heaps of garden work or DIY)
Diagnosis – How Do You Know It’s Tennis Elbow?
Physiotherapists diagnose tennis elbow by doing a thorough history and clinical exam. We’ll often:
- Palpate (press) the outside of your elbow
- Test grip strength
- Ask you to extend your wrist against resistance
- Assess shoulder, neck and wrist movement
In some cases, we’ll also check your neck – referred pain or nerve irritation from the cervical spine can mimic elbow issues.
Imaging like ultrasound or MRI is rarely needed unless your symptoms don’t improve or there’s something unusual about your case.
If you think you may have a different elbow injury, read our blog on common elbow injuries.
Why Physiotherapy is the Gold Standard for Tennis Elbow
Physiotherapy is backed by research as the most effective conservative treatment for tennis elbow (Coombes et al., 2015). We focus on three main things:
- Pain relief
- Load management
- Tendon rehabilitation and strengthening
Let’s unpack each of those…
1. Pain Relief Techniques
When you first come in, your elbow might be too painful to do much. That’s where we pull out our toolkit:
- Manual therapy: Hands-on techniques to reduce tension in the forearm muscles
- Soft tissue release: Targeting trigger points to ease tightness
- Dry needling: For deeper muscle relaxation
- Ice or heat therapy: Depending on your symptoms
- Taping or bracing: Offloads the tendon and lets it rest
We’ll also give you advice on modifying your daily activities so you’re not aggravating it constantly.

2. Load Management – Not Just Rest!
Contrary to what some people think, complete rest isn’t the answer. Tendons need to be loaded – the trick is finding the right load.
We’ll guide you through:
- Reducing high-impact or repetitive tasks
- Modifying gym routines
- Alternating tasks at work to avoid overload
- Using ergonomic tools (especially for tradies or hairdressers)
It’s a bit of trial and error, but that’s where expert physio advice makes all the difference.

3. Strengthening and Tendon Rehab
Once your pain settles, the real work begins – rebuilding tendon capacity.
We use a graded program that might include:
- Isometric holds (great early on for pain relief)
- Eccentric exercises like wrist extension with weights
- Progressive resistance training with dumbbells or resistance bands
- Shoulder and postural strengthening (because weakness here can overload the elbow)
- Functional tasks specific to your work, sport or hobbies
A full rehab program usually runs for 6–12 weeks, but many patients start to feel better much sooner.
Do Injections Work?
Cortisone injections were once common, but studies show they only give short-term relief and can actually delay long-term recovery (Bisset et al., 2006). That’s why we ALWAYS recommend physio first – it’s safer and more effective long-term.
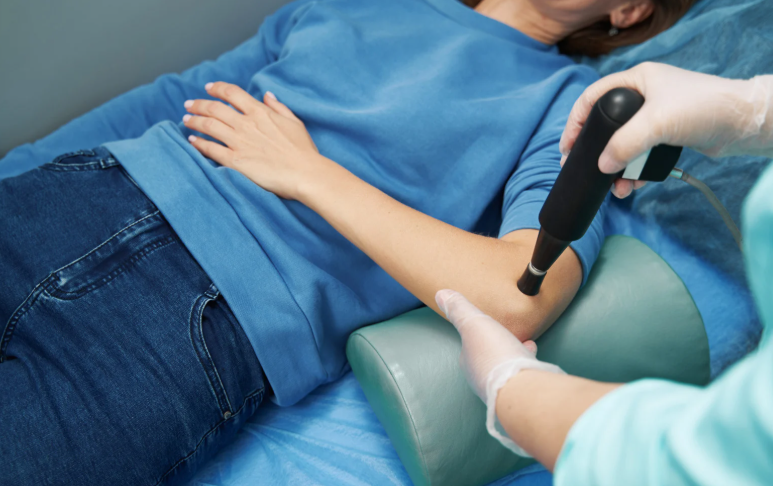
Shockwave Therapy – The New Kid on the Block
In stubborn or chronic cases, we might use shockwave therapy – a non-invasive treatment that stimulates healing in the tendon. It’s especially useful when pain’s been hanging around for months. Some clinics (including ours) offer this if needed.
Real Patient Story: Peter’s Elbow Comeback
Peter, a 48-year-old cabinetmaker from Allambie, came to us after dealing with elbow pain for nearly 4 months. It started as a mild ache while sanding and lifting tools, but it got so bad he couldn’t even grip a coffee cup without pain.
When he first saw us, Peter rated his pain 7/10 and said he was struggling to work a full day. We assessed him and confirmed tennis elbow, with marked tenderness at the lateral epicondyle and weakness in grip strength.
Over 8 weeks, we worked through:
✅ Manual therapy and dry needling to reduce muscle tension
✅ A tailored strengthening program – starting with isometric holds and progressing to eccentric loading
✅ Activity modifications at work
✅ Education on tendon load and recovery
By week 4, Peter said his pain had halved. By week 8, he was back on the tools full-time and no longer needed his brace. These days, he pops in for gym sessions in our clinic to stay strong and prevent flare-ups.
How Long Does Recovery Take?
Most people see significant improvement in 6–12 weeks, especially if they start treatment early. Chronic cases can take longer, but with the right guidance, you can get back to full strength – pain-free.
Can Tennis Elbow Come Back?
Yes, but it’s less likely if you:
- Finish your full rehab program
- Address postural issues and muscle imbalances
- Use correct lifting and tool-handling techniques
- Build up activity gradually if returning to sport or work
That’s why our focus isn’t just on fixing the pain – we work with you to build resilience and prevent recurrence.
Should You See a Physio or GP First?
You can go straight to a physiotherapist – no referral needed. We’re trained to assess, diagnose, and treat musculoskeletal conditions like tennis elbow.
If we think you need imaging, further medical tests, or another opinion, we’ll refer you on – but in most cases, physiotherapy is the first and best step.
Don’t Let Elbow Pain Drag On
Tennis elbow can be stubborn, but it’s also very treatable – especially with early physio intervention. Don’t wait for it to become chronic or start affecting your work, sport or sleep.
We’ve helped dozens of locals recover from tennis elbow and get back to the things they love – pain-free.
Give us a call today on 9806 3077, or book online, just CLICK HERE.
References
- Coombes, B. K., Bisset, L., & Vicenzino, B. (2015). Management of lateral elbow tendinopathy: One size does not fit all. Journal of Orthopaedic & Sports Physical Therapy, 45(11), 938–949.
Link - Bisset, L., Beller, E., Jull, G., Brooks, P., Darnell, R., & Vicenzino, B. (2006). Mobilisation with movement and exercise, corticosteroid injection, or wait and see for tennis elbow: randomised trial. BMJ, 333(7575), 939.
Link - Better Health Channel – Tennis Elbow
- Physiopedia – Lateral Epicondylitis
Let us help you power through the pain and take control of your recovery.
Call us today on 9806 3077, or CLICK HERE to book online.
Thinking about knee replacement or just had one done? Physiotherapy plays a critical role in getting you back on your feet—literally. In this blog, we break down the process, what to expect, and how physio can make your recovery smoother, faster, and more successful. Plus, we share a real patient story to inspire you.
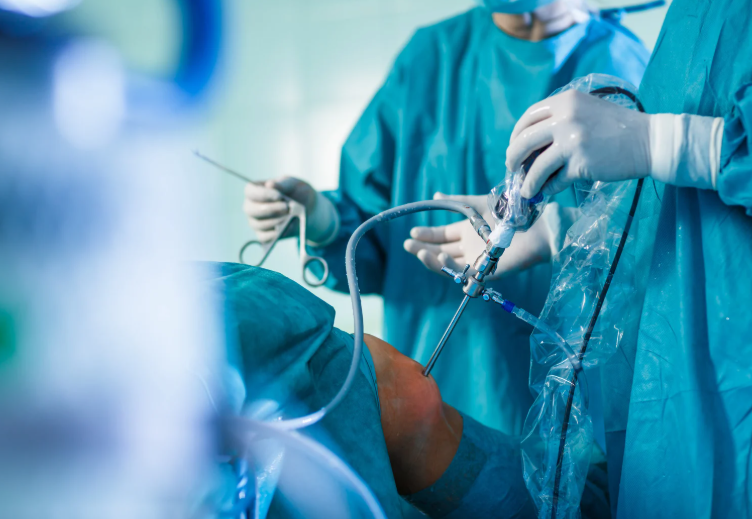
Why Knee Replacement Surgery?
Knee replacement surgery, or total knee arthroplasty, is usually the last resort when chronic knee pain and stiffness limit daily life. It’s most often recommended for people with severe osteoarthritis or joint damage that hasn’t responded to conservative treatments like medication, exercise, or physio.
You’re not alone—more than 65,000 Australians undergo knee replacements each year, and that number is steadily rising as our population ages and becomes more active (AIHW, 2023). The great news? With proper post-op rehab, the outcomes are fantastic.
The Role of Physiotherapy After Knee Replacement
Here’s the secret to a great outcome: the surgery is only half the story. The rest is all about rehab, especially physiotherapy.
Think of physio as your roadmap back to mobility, strength, and confidence. Without it, recovery is slower, stiffer, and often incomplete.
We help patients:
- Regain range of motion in the knee
- Build strength in the surrounding muscles
- Improve balance and walking patterns
- Reduce swelling and pain
- Avoid complications like scar tissue build-up or joint stiffness
Whether you’ve just come out of surgery or you’re weeks down the track and feeling stuck, physio is your best ally.
If you aren’t quite at the stage of a replacement, feel free to have a read about our blog on MENISCUS INJURIES, which will often be the issue before consider a knee replacment.
Common Challenges After Knee Replacement
Let’s be real—rehab can be tough. But understanding the common roadblocks helps you stay on track.
1. Pain and Swelling
Pain is normal post-op, but persistent or severe pain may signal issues like overdoing it, infection, or irritation of surrounding tissues. Swelling can also limit movement and slow down progress if not managed well.
2. Limited Range of Motion
Your new joint needs to move! If you don’t work early on to bend and straighten your knee properly, you risk long-term stiffness and may not regain full function.
3. Muscle Weakness
Surgery impacts the quadriceps, hamstrings, calves, and hip muscles. Weakness in any of these can lead to poor walking patterns or even back and hip pain.
4. Fear of Movement
It’s natural to be hesitant. But avoiding movement slows healing. A physio helps you build confidence, set goals, and move safely.
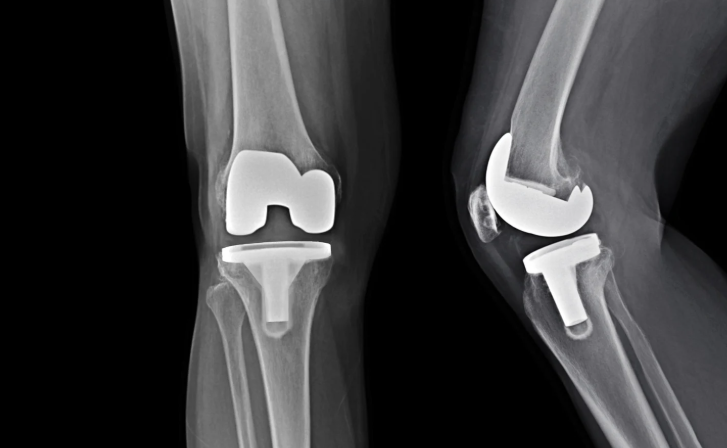
What to Expect in Physiotherapy After Knee Replacement
Week 1–2: Gentle Beginnings
- Pain and swelling management (ice, elevation, gentle massage)
- Bed-based mobility exercises (heel slides, quad sets, ankle pumps)
- Walking re-education with crutches or a frame
- Basic knee bends (aim for 90 degrees flexion by week 2)
Week 3–6: Gaining Momentum
- Weight-bearing exercises and stair practice
- Range of motion goals: aiming for 0° extension and 110° flexion
- Soft tissue work to reduce tightness and scar restriction
- Stationary cycling or gentle water-based exercise
Week 7–12: Strengthening and Function
- Squats, step-ups, resistance band work
- Return to light recreational activities (walking trails, low-impact sports)
- Balance and proprioception training
- Long-term plan to improve endurance
Beyond Week 12: Back to Doing What You Love
- Gym-based or home-based strength programs
- Return to sport (e.g. golf, swimming) if cleared by your surgeon
- Walking long distances, travelling, gardening—life as you want it
Real Patient Story: Barbara’s Recovery Journey
Meet Barbara, 72, from Frenchs Forest. She came to us six days post-op after a total knee replacement. At first, she was nervous—worried about pain, and unsure if she’d ever walk normally again.
In her first physio session, we focused on gentle movements, swelling management, and walking with a frame. By week three, she had graduated to walking with a stick and could bend her knee past 95 degrees.
We tailored her rehab with a mix of clinic and home-based exercises, including glute bridges, heel slides, step-ups, and squats using a chair.
Barbara’s turning point? Around week eight—she could walk around Warringah Mall without needing to sit every 10 minutes. She was so proud she bought us a thank-you card and a photo of her out hiking in Ku-ring-gai National Park at week 16.
Today, she continues strength training in our clinic gym, and tells us she’s “feeling younger than she has in 10 years!”
Top Tips to Maximise Your Knee Replacement Recovery
✅ Start Physio Early
The earlier we see you, the sooner we can guide your movement, manage pain, and prevent complications.
✅ Stay Consistent
Rehab doesn’t work if you don’t do it. Regular sessions + home exercises = best outcomes.
✅ Set Goals
Want to travel again? Garden? Walk the dog without limping? Tell your physio—we’ll create a plan to get you there.
✅ Don’t Compare Yourself to Others
Everyone recovers differently. Your journey is unique.
✅ Ask Questions
Unsure about your exercises or progress? We’re here to help you feel informed and confident.
Is It Too Late for Physio?
Not at all. Even if your surgery was months ago and you feel like you’ve hit a plateau, physiotherapy can still make a huge difference.
We often help people:
- Regain strength and confidence even a year after surgery
- Improve balance and reduce falls risk
- Break through stiffness and scar tissue
- Get back into activities they’ve avoided
How Long Will I Need Physio After a Knee Replacement?
There’s no one-size-fits-all answer, but here’s a rough guide:
- First 6 weeks: 1–2 sessions per week
- 6–12 weeks: Weekly or fortnightly
- 3–6 months: Check-ins and gym-based progressions
- 6–12 months: Occasional sessions if needed
Some patients like Barbara enjoy ongoing support to stay strong and mobile long-term. Others wrap up once they’ve met their goals. It’s all about your needs.
What If I Had a Partial Knee Replacement?
The principles are the same, but recovery is often faster. You may regain motion and strength quicker, but you still need physiotherapy to make sure the new joint integrates well with your body and movement patterns.
Your Local Physio in Frenchs Forest
Whether you’re just about to have surgery or you’re well into recovery, our experienced team at X Physio can help.
We offer:
- 1:1 physiotherapy tailored to your needs
- Post-op strength programs in our onsite rehab gym
- Hands-on treatments for stiffness and tight muscles
- Clear goal setting and progress tracking
- Strong relationships with local surgeons
You don’t have to do this alone. Let’s make your recovery a success story.
Final Thoughts
Knee replacement surgery is a big step—but with the right physiotherapy support, it can be a total game-changer. From day one post-op to hiking trails again, we’re here to guide, motivate and cheer you on.
Give us a call today on 9806 3077, or book online, just CLICK HERE
References
- Australian Institute of Health and Welfare. (2023). Knee replacements in Australia.
- Arthritis Australia. (2024). What is a knee replacement?
- Physio Network. (2022). Rehabilitation after total knee replacement.
- Healthdirect Australia. (2024). Total knee replacement.
- Better Health Channel. (2023). Knee replacement surgery.
Looking for physio but worried about the cost? With XPhysio Frenchs Forest being part of HCF’s More for Muscles program, you can see one of our experienced physiotherapists for a no-gap initial consultation. Read on to see how this powerful benefit could get you back on track—fast.

Struggling With Aches or Pains? Here’s Why You Shouldn’t Wait
When something hurts—whether it’s your back, neck, shoulder or knees—it’s tempting to wait it out and hope it gets better on its own. But let’s face it: most of the time, it doesn’t. That’s where physiotherapy steps in, offering hands-on treatment and tailored rehab to help you move better, feel stronger and live pain-free.
The good news? If you’re with HCF and have extras cover, you may not need to pay a cent for your first session.
That’s right—thanks to the HCF More for Muscles program, eligible members can access an initial consultation with one of our experienced physios with no out-of-pocket cost.
👉 Click here to book directly via the HCF website
What is the More for Muscles Program?
The More for Muscles initiative is HCF’s way of helping members prioritise their musculoskeletal health. It allows anyone with eligible extras cover to receive a fully covered initial physio consult at participating clinics—like ours.
There’s no catch. No paperwork. No complicated process. Just book in, swipe your card and get started on your journey to feeling better.
What You Get in That First Session:
- A full assessment of your issue or injury
- Diagnosis and education on what’s going on
- Hands-on treatment (if appropriate)
- A tailored rehab or exercise plan
- Advice on prevention strategies
Whether it’s a lingering niggle, a sports injury, or just some stiffness from sitting too long at work—this first session is your gateway to getting back on track.
Why Early Physio Matters
We often see patients who wait until pain gets unbearable before they reach out. But studies show that early intervention leads to faster recovery and fewer chronic issues. In fact, research from the Australian Physiotherapy Association (APA) shows that people who begin physio early for lower back pain recover quicker and have lower healthcare costs in the long run [1].
By taking advantage of a no-gap appointment, you’re essentially removing the financial hesitation that often causes delays in care.
And with Oliver Docker and our experienced team, you’re in safe hands.

Real Patient Success Story: Meet Sam from Frenchs Forest
Sam found us online while searching for “HCF no gap physio Frenchs Forest” after experiencing sharp lower back pain while lifting her toddler. She had been ignoring it for weeks, thinking it was just “mum life” catching up. But when it started affecting her sleep and ability to drive, she decided it was time to do something.
Through the HCF More for Muscles program, Sam booked her initial consultation with us at no cost. In that session, we uncovered that her back pain stemmed from gluteal weakness and tight hip flexors—a common postnatal issue.
We created a program tailored to her lifestyle and gradually restored her movement and strength through:
- Gentle manual therapy
- Core activation and control training
- Glute strengthening exercises
- Advice on lifting and posture around the house
After 5 sessions, Sam was back to doing school drop-offs and lifting her little one with confidence. She was so inspired by the progress that she joined Plus Fitness Frenchs Forest and now regularly strength trains to keep her back strong and her pain at bay.
She’s become one of our many More for Muscles success stories—and she’s not looking back.
If you want to read more about this topic, CLICK HERE to read a blog about Spine Pain
Who Can Use the More for Muscles Program?
If you’re an HCF member with eligible extras cover (check your level here: HCF Extras Cover), you’re most likely eligible.
It’s available to both new and existing HCF extras members, and the benefit resets each calendar year.
If you’re unsure, just give HCF a ring—or give us a call and we’ll help you figure it out.
Why Choose Us?
There are plenty of physios out there—but here’s what makes our team different:
✅ Expert, hands-on care
We don’t just hand you a print-out and send you home. We provide hands-on treatment and clear advice.
✅ Personalised rehab plans
Your life is unique—your treatment plan should be too. Whether you’re a desk jockey, busy parent, or weekend warrior, we tailor rehab to fit your lifestyle.
✅ Cutting-edge techniques
We use a combination of manual therapy, dry needling, strength training, Pilates, and functional rehab to get the best results.
✅ Integrated care with Plus Fitness
Our collaboration with Plus Fitness Frenchs Forest means many of our patients have access to gym-based rehab programs once they’re ready to level up.
✅ No-gap initial appointment
And best of all, if you’re with HCF—your first appointment might cost you absolutely nothing.
What Conditions Can We Treat?
The More for Muscles program isn’t just for one type of issue—it can be used for a wide range of musculoskeletal concerns, including:
- Lower back pain
- Neck and shoulder tension
- Knee pain or injuries
- Ankle sprains
- Posture-related problems
- Work-from-home stiffness
- Sports injuries
- Arthritis and age-related wear and tear
Don’t wait until the problem becomes unbearable. The earlier we get started, the quicker the results.
How Do I Book?
It’s simple:
👉 Click here to book directly via the HCF website
Or, if you prefer, contact our friendly team directly and we’ll guide you through it.
📞 Call us on 9806 3077
🖱️ Or book instantly via our online system:
👉 CLICK HERE
Make the Most of Your Private Health Cover
You’re already paying for private health—why not use it to its full potential? The More for Muscles program is one of the most generous physio benefits out there.
Here’s a little breakdown of how it works:
| What You Get | Details |
| Cost | $0 (if eligible HCF extras member) |
| What’s Included | Full initial physio consultation |
| Available For | All ages, all muscle & joint issues |
| Booking Required | Yes – via online or phone |
| Participating Provider Required | Yes – we’re a listed provider |
Your Body Deserves Better
Pain doesn’t have to be your norm. Whether you’re recovering from injury, managing a chronic condition or just tired of feeling stiff and sore, physiotherapy can help.
And with no-gap access through HCF, there’s never been a better time to try.
Final Word: Take The First Step
You don’t need to suffer through pain, rely on painkillers, or “wait and see”. With one call—or a couple of clicks—you could be booked in for your first session at no cost.
Just like Sam, you could be on your way to a stronger, pain-free body with the support of experienced physios and a gym-based strength program at Plus Fitness Frenchs Forest.
Don’t wait. Make use of what your health cover offers—and give your body the care it deserves.
Give us a call today on 9806 3077, or book online, just CLICK HERE
References:
- Australian Physiotherapy Association – Value of Early Physiotherapy
- HCF More for Muscles Program Info
- HealthShare – Oliver Docker HCF Provider Profile
- HCF Extras Cover Info
Got an annoying ache in your shoulder that just won’t go away? It could be bursitis. In this blog, we’ll break down what shoulder bursitis actually is, how to spot the signs early, and—most importantly—how physiotherapy can help you bounce back pain-free.
Why Is My Shoulder So Sore?
If you’ve been dealing with persistent shoulder pain, especially when reaching overhead or lying on your side, you’re not alone. Shoulder bursitis is a common culprit that can sneak up after repetitive movements, poor posture, or even a minor bump to the shoulder.
Bursitis refers to inflammation of the bursa—small, fluid-filled sacs that cushion the joint. When the bursa becomes irritated or inflamed, it can lead to swelling, pain, and stiffness, often affecting your day-to-day activities like dressing, driving, or even sleeping. Bursitis can occurr elsewhere in our body, click this LINK for our hip bursitis blog.
The good news? It’s very treatable—and that’s where physiotherapy comes in.

What Exactly Is Shoulder Bursitis?
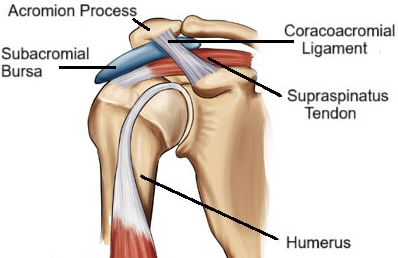
The shoulder has several bursae, but the subacromial bursa is the one most likely to cause trouble. It sits between your rotator cuff tendons and the bony arch of your shoulder blade (the acromion). When this bursa gets inflamed, it creates friction in the joint, which leads to that nasty, nagging pain.
Common Causes of Shoulder Bursitis
- Repetitive overhead movements (e.g. painting, throwing, swimming)
- Poor posture or slouching
- Direct trauma (falling on the shoulder)
- Rotator cuff injuries or impingement
- Age-related degeneration
Signs You Might Have Shoulder Bursitis
You might be dealing with bursitis if you notice:
- A dull ache or sharp pain in the shoulder
- Discomfort when lying on the sore side
- Pain with overhead activities like reaching or washing hair
- Swelling or warmth near the shoulder
- Limited range of motion
One tell-tale sign: the pain often feels worse at night, especially when trying to sleep on the affected shoulder.
Why Physiotherapy Is a Game-Changer
Too often, people try to “rest” their way through shoulder pain, only to find that it lingers or gets worse. While rest might temporarily ease symptoms, physiotherapy gets to the root of the issue.
At our clinic, we focus on:
1. Reducing Inflammation and Pain
In the early stages, your physio may use ice, gentle massage, taping, or modalities like ultrasound therapy or dry needling to calm things down.
2. Restoring Shoulder Mobility
Once inflammation settles, we’ll help you regain range of motion through gentle stretching, joint mobilisation, and guided movements to avoid stiffness.
3. Strengthening Supporting Muscles
We’ll target weaknesses in the rotator cuff, scapular stabilisers, and postural muscles—key players in preventing bursitis from returning.
4. Correcting Posture and Movement Patterns
Poor posture and movement habits are often the sneaky reason bursitis develops. Your physio will assess and coach you on better techniques—whether it’s your desk setup or your gym form.
What Happens If You Don’t Treat It?
Ignoring shoulder bursitis can lead to:
- Chronic pain that lingers for months
- Frozen shoulder (adhesive capsulitis)
- Rotator cuff impingement
- Reduced quality of life
That’s why early intervention is so important. Don’t just “put up with it”—sort it out before it gets worse.
Meet Jess: A Real Patient Story
Jess, a 43-year-old hairdresser from Frenchs Forest, came to us with intense shoulder pain that had been creeping in for months. She initially brushed it off as “just work strain,” but it gradually got to the point where she couldn’t lift her arm to blow-dry clients’ hair without wincing.
An ultrasound confirmed subacromial bursitis and mild rotator cuff tendinopathy. Jess was worried she’d need a cortisone injection—or worse, surgery.
But with a structured physiotherapy plan, she turned things around.
Here’s how Jess improved:
- Week 1–2: Pain relief strategies including taping, dry needling, and gentle stretches.
- Week 3–6: Progressive strengthening of her rotator cuff and shoulder blade muscles.
- Week 7–10: Return-to-work conditioning, including postural retraining and lifting techniques specific to her role.
- Outcome: Jess was back to full duties by week 8, pain-free and confident in her shoulder. No injections needed.
She now does maintenance exercises twice a week and pops in for a check-up every few months.
How Long Does Shoulder Bursitis Take to Heal?
With early treatment, mild cases can resolve in 3–6 weeks. More stubborn cases may take a couple of months—especially if there are coexisting issues like tendinopathy or impingement.
Your physio will guide you through each stage so you’re not stuck in limbo wondering if you’re doing too much—or not enough.
What About Cortisone Injections?
Cortisone can be effective at settling inflammation, but it’s not always necessary. In many cases, physiotherapy alone is enough, especially if you’re committed to a tailored program.
We usually suggest trying at least 4–6 weeks of physio first. If pain persists or significantly impacts your sleep and function, a cortisone shot may be considered in conjunction with ongoing rehab.
And for those who don’t love needles (like Jess!), physiotherapy is a great first-line option.

Top Tips to Prevent Bursitis
Whether you’re recovering or want to avoid shoulder issues down the track, these tips are golden:
- Check your posture—especially if you sit at a desk or drive a lot.
- Warm up before any overhead activities or sports.
- Balance your workouts—don’t just focus on chest and arms, strengthen the back and rotator cuff too.
- Avoid repetitive strain—take breaks if your job or hobby involves lots of overhead work.
- Get niggles checked early—small issues can snowball if ignored.
When to See a Physio
Come see us if:
- Your shoulder pain isn’t going away after a week or two
- It hurts to lift, reach, or lie on your shoulder
- You’ve had shoulder pain on and off for months
- You’re relying on painkillers or avoiding certain activities
- You’ve already tried rest, but it hasn’t worked
Ready to Take the Next Step?
Shoulder bursitis doesn’t have to drag you down. With the right physiotherapy treatment, most people make a full recovery and get back to doing what they love—pain-free.
At our clinic, we take the time to listen, assess, and tailor your rehab to your goals, whether that’s getting back to work, sport, or simply sleeping comfortably again.
Don’t let shoulder pain hold you back. Let’s fix it—together.
References and Further Reading
Give us a call today on 9806 3077, or book online, just CLICK HERE
Your spinal column is more than just a stack of bones — it’s the core of everything you do, from walking and lifting to simply sitting. In this blog, we break down the spinal column, bust common myths, and reveal how physiotherapy can be the game-changer for back pain and spinal health.
Let’s Talk About the Spine — The Unsung Hero of Your Body
When most people think of their spinal column, they just picture their back. But this incredible structure is way more than a bony column. It’s your central support system, the bridge between your brain and body, and the protector of your spinal cord. Yet somehow, it rarely gets the attention it deserves — until it starts hurting.
Sound familiar?
That’s when the “Google spiral” starts: bulging discs, degenerative changes, scoliosis, spinal stenosis… It all sounds scary, but the good news is that many spinal issues are treatable — and often preventable — with the right physiotherapy approach.
What Is the Spinal Column, Exactly?
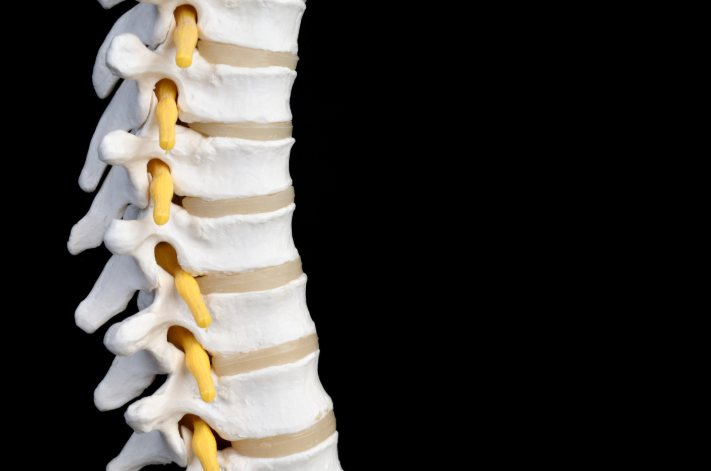
The spinal column (aka your vertebral column) is a series of 33 bones (vertebrae) stacked on top of each other. These bones are divided into five regions:
- Cervical spine (neck) – 7 vertebrae
- Thoracic spine (mid back) – 12 vertebrae
- Lumbar spine (lower back) – 5 vertebrae
- Sacrum – 5 fused vertebrae
- Coccyx (tailbone) – 4 fused vertebrae
Between most of these vertebrae are intervertebral discs – think of them as shock absorbers that help the spinal column move and carry loads. Add in muscles, ligaments, joints, and nerves, and you’ve got a highly mobile yet delicate system.
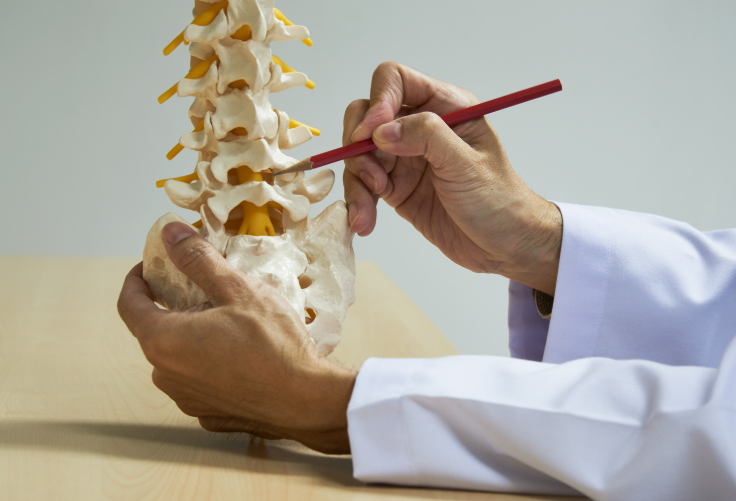
Common Spinal Column Conditions Physios See
Here’s a quick overview of some of the most common spinal problems we treat in the clinic:
🔹 Disc Injuries (e.g. herniation or “slipped” discs)
These occur when a disc bulges out and presses on nearby nerves. Symptoms might include back pain, numbness, tingling, or even shooting leg pain (sciatica).
🔹 Facet Joint Sprains
The facet joints connect each vertebra to the next. These can get inflamed from poor posture, sudden movement, or overuse.
🔹 Degenerative Disc Disease (DDD)
This is a natural part of ageing, where the discs lose hydration and height. It sounds scary but often doesn’t cause symptoms unless it compresses a nerve.
🔹 Spinal Stenosis
This is a narrowing of the spinal canal, often linked to age, which can cause nerve compression and leg symptoms.
🔹 Postural Back Pain
Prolonged sitting, slouching, and poor ergonomics can cause muscle fatigue and pain, especially in the neck and lower back.
Why Physiotherapy Works Wonders for the Spinal Column
Forget the quick fixes and short-term pain relief – spinal health needs a whole-body, long-term strategy. Physiotherapy helps by:
✅ Reducing Pain and Inflammation
Through manual therapy, dry needling, soft tissue release, and taping techniques.
✅ Improving Mobility and Flexibility
Spinal stiffness responds really well to targeted mobilisation and stretching.
✅ Strengthening Core and Postural Muscles
A stronger core supports the spinal column and reduces the load on discs and joints.
✅ Correcting Movement Patterns
Your physio will identify and correct poor movement habits that keep causing flare-ups.
✅ Educating and Empowering You
Understanding your condition is key. We teach you what’s safe to do (and what’s not), so you stay in control.

Case Study: Meet Brian – A Classic Example of Spinal Recovery Done Right
Brian, a 58-year-old accountant from Belrose, came to the clinic with ongoing lower back pain that had worsened after moving office furniture over the weekend. He described a dull ache that radiated into his right hip and thigh, especially after sitting for long periods. He was worried it might be a disc injury.
After a thorough assessment, we identified the root cause: a combination of lumbar disc irritation and gluteal muscle weakness, made worse by years of sitting and poor lifting technique.
🎯 Brian’s Physio Treatment Plan:
- Manual therapy to relieve joint stiffness and calm the irritated tissues
- Dry needling of the glutes and lumbar paraspinals
- Core and hip strengthening program (initially mat-based, then progressed to our clinic gym)
- Education on safe lifting and setting up a home workstation
Within four weeks, Brian reported 70% improvement. By the eight-week mark, he was pain-free, back to light gym sessions, and moving office furniture the right way this time.
Simple Stretches to Keep Your Spine Happy
Here are three physio-approved movements to add into your daily routine:
🧘♀️ 1. Cat-Cow Stretch (for mobility)
- Start on all fours.
- Arch your back up (cat), then dip it down (cow).
- Repeat slowly 10 times.
🪢 2. Knee-to-Chest Stretch (for lower back release)
- Lie on your back, bring one knee toward your chest.
- Hold for 20 seconds, switch sides.
🏹 3. Thoracic Extension Over Foam Roller (for mid-back posture)
- Lie with a foam roller under your upper back.
- Gently extend over the roller and breathe.
- Do 2–3 reps, hold each for 10–15 seconds.

Myths Busted: What People Get Wrong About the Spine
Let’s clear up a few things:
❌ “I need a scan to know what’s wrong.”
Not always. Many back issues don’t show up clearly on scans, and even scary-sounding findings (like disc bulges) are often seen in people with no pain. Your symptoms, movement, and history tell us much more.
❌ “If I have back pain, I should rest completely.”
Nope! Movement is medicine. While you might need to modify some activities, complete rest usually makes things worse.
❌ “I’ll need surgery.”
Surgery is rarely the first option. Most spinal issues respond well to conservative physiotherapy treatment.
When to See a Physio for Spinal Pain
Here are some signs it’s time to book in:
- Ongoing or recurring back or neck pain
- Pain that radiates down your leg or arm
- Stiffness or tightness that doesn’t ease with stretching
- A sudden “lock-up” feeling in the spine
- Reduced mobility or weakness
- Poor posture that’s affecting comfort or performance
Don’t wait until it’s severe – early treatment is far more effective (and cheaper) than dealing with chronic issues.

Looking After Your Spine: Everyday Tips That Work
- Switch positions often – no sitting or standing for too long
- Invest in an ergonomic setup – your desk, chair, and screen height matter
- Stay strong – regular exercise keeps spinal muscles and discs healthy
- Learn to lift properly – use your legs, not your back
- Sleep smart – a supportive mattress and good pillow alignment go a long way
Final Thoughts: Your Spine Is Resilient – Let’s Keep It That Way
The spinal column cops a lot – sitting, lifting, twisting, sleeping wrong – but it’s also incredibly strong and adaptable. The key is knowing how to care for it, and that’s where physiotherapy shines.
Whether you’re in pain now or just want to future-proof your spine, working with a physio can transform how you move and feel. We’re not just treating pain – we’re helping you build a stronger, smarter spine for life.
✅ Call to Action: Don’t Let Back Pain Run the Show
If your spine’s been giving you grief, don’t tough it out. Book an appointment with one of our experienced physiotherapists today and start feeling better, moving better, and living pain-free.
👉 Book Online Now or call us on 9806 3077 – your spine will thank you.
References and Further Reading:
- Australian Physiotherapy Association – Back Pain:
- Spine Health – Understanding Spinal Anatomy:
- Our blog:
When most people think about ankle pain, they immediately picture a sprained ankle. But there are loads of other culprits that can leave you hobbling — and some are trickier to diagnose. Whether it’s tendon issues, impingement, or nerve irritation, understanding the full picture is crucial for proper recovery. Let’s dive in! If you want to read more about ankle sprains: CLICK HERE
What Other Injuries Cause Ankle Pain?
While ankle sprains are the classic injury, there are several other conditions that can cause pain here — sometimes even worse than a sprain! Here are some of the big ones we see in the clinic:
1. Ankle Impingement
Impingement happens when soft tissues (like ligaments or tendons) or bony structures get pinched within the joint during movement. It’s a common issue after repeated sprains, but it can also develop from overuse — especially in sports like soccer, netball, and running.
There are two main types:
- Anterior impingement (front) – usually feels stiff or painful when you try to bend your foot upwards.
- Posterior impingement (back) – often hurts when pointing the toes down, like pushing off or kicking.
Signs you might have impingement:
- Sharp pain at a specific spot in the ankle
- Swelling around the front or back of the joint
- A feeling of “catching” or “blocking” with movement
- Loss of full range
Physiotherapy focuses on restoring normal movement, reducing swelling, and strengthening the surrounding muscles to unload the pinched joint. Early treatment is key to avoiding long-term stiffness or degeneration.

2. Peroneal Tendinopathy
The peroneal tendons run along the outside of your ankle and foot, helping stabilise your balance — especially on uneven ground. Overuse (think running, hiking, or even walking on sand) can lead to tendinopathy, a painful irritation of the tendon.
Common symptoms:
- Pain on the outside
- Pain that worsens with activity
- Swelling along the tendon
- A feeling of weakness or instability
Without treatment, this condition can drag on for months. Physiotherapy focuses on reducing load, strengthening the muscles, and retraining balance to get you back on track.
3. Posterior Tibial Tendinopathy
This injury often masquerades as a vague ache on the inside of the ankle or arch. It’s common in people who do a lot of walking, standing, or running — particularly if they have flat feet or poor footwear.
Signs to watch for:
- Pain along the inner gutter
- Swelling around the tendon
- Difficulty standing on your toes
- A slowly collapsing arch
Treatment usually involves supportive taping, orthotics, strengthening exercises, and sometimes a temporary rest from impact activities.

4. Osteochondral Lesions
Sounds fancy, right? An osteochondral lesion is damage to the cartilage and underlying bone inside the ankle joint, usually following a traumatic injury like a bad sprain or fall.
Key symptoms:
- Deep ankle pain (especially with weight-bearing)
- Swelling after activity
- Clicking or catching in the ankle
Left untreated, these can cause ongoing issues and even lead to early arthritis. Physiotherapy plays a massive role in restoring mobility and strength after this injury — often helping people avoid surgery.
5. Tarsal Tunnel Syndrome
Think of this as “carpal tunnel” but in your ankle. The tibial nerve runs through a tight space (the tarsal tunnel) on the inside of the ankle, and sometimes it gets compressed.
What you might notice:
- Burning or tingling in the ankle or foot
- Numbness
- Pain that worsens with standing or walking
Early physio can make a big difference by addressing underlying issues like swelling, biomechanics, or even nerve gliding exercises.
6. Ankle Arthritis
Ankle arthritis isn’t as common as hip or knee arthritis, but it can still wreak havoc — especially after an old injury. It usually develops over years and tends to be more common in people who’ve had multiple sprains, fractures, or high-impact careers (hello, tradies!).
Symptoms include:
- Stiffness in the morning or after rest
- Swelling and tenderness
- Pain that worsens with activity
Physiotherapy can help maintain ankle mobility, strengthen supporting muscles, and reduce pressure through the joint — delaying the need for surgery as long as possible.
How Physiotherapy Can Help
No matter the cause, getting a proper diagnosis and starting the right rehab early can save you months (or years) of ankle pain. Physiotherapy treatment may include:
✅ Detailed Assessment: Understanding the specific structures involved through movement tests, palpation, and sometimes referral for imaging.
✅ Pain Management: Taping, manual therapy, gentle exercises, and load management strategies.
✅ Strengthening and Balance Exercises: Building strength in the ankle and surrounding muscles (like the calf, glutes, and core) helps prevent future injuries.
✅ Activity Modification: Helping you stay active safely, without aggravating the injury.
✅ Return to Sport or Work Planning: Step-by-step guidance to get you back to full activity without setbacks.

Real Patient Story: Kate’s Journey Back to Hiking
Kate, a 36-year-old outdoor enthusiast, came to see us after feeling persistent pain on the outside of her right ankle. She initially thought it was “just a sprain” after a bushwalk six months earlier, but the pain hadn’t settled despite rest and ice.
After a thorough assessment, we diagnosed her with peroneal tendinopathy — likely aggravated by the uneven trails and her love for minimalist shoes. An ultrasound confirmed mild swelling and thickening of the tendon.
Here’s what her physio plan looked like:
- Short-term activity modification (no hills or unstable terrain initially)
- Targeted strengthening exercises for the peroneal muscles and glutes
- Taping to unload the tendon during walks
- Footwear advice, moving her to a more supportive shoe with slight ankle support
- Progressive return to hiking after 6 weeks of building up strength and endurance
After about 10 weeks, Kate was back hiking pain-free — and she even completed the Coast Track in the Royal National Park without a hitch! She still keeps up with her strength program twice a week to prevent future flare-ups.
Common Mistakes to Avoid
Here are a few things we often see that can stall recovery:
🚫 Pushing through pain too early: Just because you can walk doesn’t mean the ankle is ready for high loads.
🚫 Ignoring strength and balance exercises: These are crucial, even after pain settles.
🚫 Wearing the wrong shoes: Minimalist shoes can be great for some, but when dealing with an injury, a little extra support goes a long way.
🚫 Not seeking help soon enough: Chronic issues are harder to fix than acute ones — early intervention is key!
Final Thoughts
Ankle pain can sneak up in many different forms — not just sprains! Getting a proper diagnosis and starting a tailored rehab plan can be the difference between limping along for months and getting back to doing what you love.
If you’re dealing with stubborn ankle pain, don’t tough it out — book in for an assessment. With the right treatment, you can recover faster, stronger, and smarter.
References and Further Reading
- Better Health Channel: Ankle injuries and disorders
- Physiopedia: Ankle Impingement
- Sports Medicine Australia: Foot and Ankle Injuries
Tendon injuries can be sneaky—starting as a niggle, then becoming that one thing stopping you from doing what you love. In this blog, we break down what issues surrounding this structure, why they don’t just go away with rest, and how physiotherapy can help you turn things around.
What Are Tendons, Anyway?
Let’s start with the basics. Tendons are the strong, fibrous tissues that connect your muscles to bones. Their job? To transfer the force your muscles generate so you can move. Simple enough. But when they’re overused, overloaded or just not looked after properly, they can become irritated or damaged.
Tendon injuries, also called tendinopathies, are super common—especially if you’re active, over 30, or just pushing yourself a bit too hard too soon (hello, weekend warriors).
Some of the usual suspects when it comes to pain include:
- Achilles tendinopathy
- Patellar tendinopathy (aka “jumper’s knee”)
- Gluteal tendinopathy (pain on the side of the hip)
- Rotator cuff tendinopathy (in the shoulder)
- Tennis/golfer’s elbow (lateral/medial elbow tendinopathy)
Tendonitis, Tendinosis, or Tendinopathy?
You’ve probably heard these terms thrown around, but what’s the difference?
- Tendonitis: This used to be the go-to term, and it refers to inflammation of a tendon. But research shows that inflammation isn’t the main issue in most chronic injuries.
- Tendinosis: This refers to a degenerative process in the tendon, usually from overuse.
- Tendinopathy: This is the umbrella term we use now, because most tendon injuries involve a mix of mechanical overload and structural changes—not just inflammation or degeneration.
So next time someone says they’ve got “tendonitis,” chances are they’re actually dealing with tendinopathy.
Why Do Tendon Injuries Happen?
Tendon injuries usually come down to load—too much of it, too quickly, without giving it time to adapt. Think:
- Going too hard after a break (classic New Year’s resolution injuries)
- A sudden increase in training (like prepping for a half marathon)
- Weak supporting muscles or poor biomechanics
- Age-related changes in tendon structure
- Under-recovery between sessions
Tendons love slow, controlled loading. What they hate is a sudden spike in activity with no build-up. And unfortunately, once a tendon gets grumpy, it tends to stay that way for a while—unless you treat it properly.

Rest Doesn’t Work (Sorry!)
This is the part most people don’t want to hear: resting a tendon injury doesn’t fix it.
Sure, it might feel better after a few days or weeks of laying low. But as soon as you go back to your usual activity, the pain is back. That’s because rest doesn’t restore the strength or capacity—it just de-loads it temporarily.
The gold standard for rehab? Progressive, targeted loading. That’s where physiotherapy comes in.
How Physio Can Help
When it comes to tendon rehab, we don’t muck around. Here’s how we usually approach it in the clinic:
1. Accurate Diagnosis
We’ll start by figuring out exactly which tendon is affected and what stage of the injury you’re in—early reactive phase, disrepair, or degenerative. This helps us tailor your treatment plan. Furthermore, we will determine the specific part that has become injured as this will also determine the rehabilitation.
2. Load Management
This might involve reducing or modifying your activity (not just stopping altogether) while gradually building your tendon’s tolerance to load.
3. Strengthening Program
We’ll guide you through a tailored loading program, often using isometric, isotonic, or eccentric exercises depending on the phase of healing. These help rebuild the tendon’s capacity and reduce pain over time. The finish line will be determined by you. We will work towards your individual end goal, this could be reaching a faster pace with your 5km run or being able to complete 3000-5000 steps in a day.
4. Biomechanical Corrections
If your movement patterns or posture are contributing to the issue, we’ll help correct that. This could include strengthening weak muscles, improving joint mobility, or tweaking your technique.
5. Education
Understanding your injury is half the battle. We’ll chat about what to expect, how to pace yourself, and when to push versus pull back.
6. Adjunct Therapies
In some cases, we might use hands-on treatment, dry needling, taping, or shockwave therapy to complement your exercise program.
Real Patient Story: Meet Cam
Cam’s a 47-year-old dad of two, ex-footy player, and now a keen weekend runner. He came to us after noticing a persistent ache just above his heel that flared up every time he went for a run. He’d tried resting, stretching, and even new shoes—but nothing worked.
Turns out, Cam had mid-portion Achilles tendinopathy—a classic case.
Here’s what we did:
- Initial Phase: We started him on isometric calf holds (holding a heel raise for 45 seconds) to reduce his pain and gently load the tendon.
- Loading Progression: As his pain settled, we introduced slow calf raises with increasing load (eventually adding dumbbells).
- Running Technique: We noticed he was overstriding and landing too hard through the heel, so we worked on cadence and foot strike.
- Cross Training: While we deloaded his running, he kept up his fitness with cycling and pool running.
- Return to Running: After about 6 weeks, he started a graded return-to-run program. By 12 weeks, he was comfortably back to 5km runs with no pain.
Now? Cam’s running three times a week and mixing in strength training to keep his tendon happy. No niggles. No flare-ups. And he reckons he’s running better than he did in his 20s.

Common Tendon Injury Myths—Busted
“It’ll go away on its own.”
Probably not. Most tendon injuries are persistent and can get worse if ignored.
“I just need to stretch more.”
Stretching a grumpy tendon can actually make things worse, especially if it’s already overloaded. Strengthening is the priority.
“Cortisone will fix it.”
Cortisone might reduce pain in the short term, but it doesn’t address the underlying issue—and repeated injections can weaken the structure long-term.
“I’m too old to fix this.”
Nope! They respond to load at any age. It just takes a bit more time and consistency
What Recovery Looks Like
Tendon injuries don’t follow the quick-fix timeline. They heal on their own clock. Here’s a rough idea:
| Phase | Focus | Duration |
| Acute (0–3 weeks) | Pain relief, isometric loading, activity modification | 1–3 weeks |
| Subacute (3–6 weeks) | Load progression, address contributing factors | 3–6 weeks |
| Remodeling (6–12+ weeks) | Build tendon capacity, return to full sport/activity | 6–12+ weeks |
Consistency is key. Stick to your program and avoid the temptation to jump ahead too soon.
When to See a Physio
If you’ve got tendon pain that’s:
- Sticking around for more than a few weeks
- Worse with activity and settles with rest
- Tender to touch or sore the next day
- Starting to limit your usual exercise or daily tasks
…it’s time to book in.
The earlier we catch it, the quicker you’ll bounce back.
Final Word
Tendon injuries can be annoying—but they’re also very treatable. With the right mix of education, progressive loading, and a bit of patience, you can get back to doing what you love, pain-free.
So if your Achilles, knee, shoulder or hip is holding you back, don’t just rest and hope for the best. Come see us at XPhysio, and let’s put a proper plan in place. You can book online via this LINK
References and Further Reading
- Achilles Tendinopathy – Physiopedia
- Patellar Tendinopathy – Clinical Edge
- Gluteal Tendinopathy – Latrobe University
- Shoulder Tendinopathy – British Journal of Sports Medicine
Torn your Anterior Cruciate Ligament (ACL)? You’re not alone—and it’s not the end of your sport. ACL injuries are common, especially among active Aussies, but with the right rehab plan, you can come back strong. In this blog, we’ll break down what an ACL injury actually is, how physio helps, and share a real success story from our clinic.
What is the ACL?
The anterior cruciate ligament (ACL) is one of the key ligaments that stabilise your knee joint. It connects the thigh bone (femur) to the shin bone (tibia) and helps control back-and-forth movement and rotation of the knee.
It plays a massive role when you’re:
- Changing direction quickly
- Landing from a jump
- Stopping suddenly while running
- Pivoting or twisting
Which is why sports like soccer, netball, basketball, footy, and skiing tend to see a lot of ACL injuries. When it tears, the knee often gives way—and so does the heart of anyone who’s ever heard that dreaded “pop”.

How Does an ACL Tear Happen?
Most ACL injuries are non-contact. That means they happen without a tackle or direct blow—often during a sudden stop, twist, or awkward landing.
You might hear or feel a “pop”, followed by:
- Immediate swelling
- Pain (though not always intense)
- A sense of instability or “giving way”
- Difficulty walking or bearing weight
Do You Need Surgery?
Here’s the thing—not everyone with an ACL tear needs surgery. While some high-level athletes or people with very unstable knees may opt for reconstruction, others do really well with a structured physiotherapy program.
In fact, recent research has shown that non-operative rehab can be just as effective in many cases, especially for people who aren’t involved in pivot-heavy sports (Grindem et al., 2016).
The Role of Physiotherapy
Whether you’re going down the surgical or non-surgical route, physiotherapy is essential for:
1. Regaining Range of Motion
We’ll get that knee moving again (safely), focusing on bending, straightening, and easing stiffness.
2. Reducing Swelling and Pain
With manual therapy, taping, ice, and gentle movement, we can bring swelling down and get your pain under control.
3. Building Strength
The quads, hamstrings, glutes, and calves all play a role in stabilising the knee. We gradually strengthen these through a targeted program.
4. Restoring Stability
Balance and proprioception exercises help retrain the brain and body to work together again—especially after that trust in your knee has taken a hit.
5. Sport-Specific Drills
Closer to the end of rehab, we introduce jumping, pivoting, and change-of-direction training tailored to your sport.
Phases of ACL Rehabilitation
Rehab isn’t a one-size-fits-all journey, but here’s a rough breakdown of what the process looks like:
Phase 1: Acute Management (Weeks 0–2)
- Rest, ice, compression, elevation (RICE)
- Gentle movement to restore range
- Reduce swelling and protect the knee
Phase 2: Early Strength (Weeks 2–6)
- Static and dynamic strength work
- Isolated muscle activation (especially quads and glutes)
- Begin weight-bearing as tolerated
Phase 3: Progressive Loading (Weeks 6–12)
- Functional strength (squats, lunges, bridges)
- Balance and proprioception training
- Low-impact cardio (bike, elliptical)
Phase 4: Return to Running (From Week 12+)
- Treadmill or grass running program
- Plyometrics and agility drills
- Increased sport-specific movements
Phase 5: Return to Sport (6–12 months)
- Sport-specific training
- Decision-making under fatigue
- Clearance testing (e.g. hop tests, strength ratios)
Note: These timelines vary depending on whether surgery is involved and how your body responds to rehab.
Bracing and Supports
Some patients choose to wear an ACL brace for extra support—especially during the early stages or when returning to sport. While braces don’t replace strong muscles and good control, they can help with confidence.
Your physio can help you decide if a brace is right for your goals.
Common Mistakes We See
❌ Rushing back too soon
Don’t skip steps. Even if your knee feels okay, skipping strength or neuromuscular control work increases your risk of re-injury.
❌ Avoiding movement altogether
Yes, it’s injured—but total rest isn’t the answer. Safe, guided movement early on prevents stiffness and helps circulation.
❌ Copying someone else’s rehab plan
Everyone’s injury, goals, and body are different. What works for one person might not suit you. That’s why seeing a physio makes a big difference.
Real Case Study: Emily’s ACL Comeback
Emily, 27, came to our clinic after a netball injury. She landed awkwardly after a jump and felt a sudden “pop” followed by intense swelling. A trip to the physio the next day confirmed the signs of an ACL tear, and an MRI confirmed it: complete ACL rupture with no other ligament damage.
Emily was devastated—she’d just made it into a local rep team and thought her season was over. After consulting with her orthopaedic surgeon, she decided to try conservative management (no surgery) with a 6-month structured physiotherapy program.
Here’s what we did:
- Phase 1: We focused on swelling reduction, gentle movement, and basic quad activation.
- Phase 2–3: We built up her strength with glute bridges, step-ups, resistance band work, and core exercises.
- Phase 4: We introduced treadmill running, hopping, and sport-specific drills like side-stepping and landing practice.
- Phase 5: She passed her hop tests and strength benchmarks—and was cleared for sport 7 months post-injury.
Now, Emily’s back on the netball court and plays with more confidence than ever. She still does her rehab exercises twice a week and sees us for a monthly check-in.
Prevention: Can You Stop an ACL Tear?
You can’t prevent every injury, but certain programs have been shown to lower ACL injury risk—especially in young athletes and females. These include:
- Proper warm-ups: Dynamic, not static stretching
- Landing mechanics: Soft landings, knees aligned
- Strengthening: Especially hamstrings and glutes
- Neuromuscular training: Jumping, cutting, and agility drills with good form
Ask us about programs like the FIFA 11+ or Netball Australia’s KNEE program—we often run workshops for local clubs.
When to See a Physio
If you’ve had a knee injury and feel any instability, swelling, or limited motion, book in with a physio. Even if you’re not sure it’s the ACL, we can assess it properly, refer you for imaging if needed, and get you started on the right path—whether you go down the surgery track or not.
Final Thoughts
An ACL injury can be a major setback, but it doesn’t have to be the end of your story. With proper physio guidance, targeted rehab, and a bit of patience, you can get back to sport—and maybe even come back stronger.
Got a niggling knee issue? Reach out to your physio. The earlier you act, the better the outcome.
Give us a call today if you want to ask us a question: 9806 3077
References & Further Reading
- Grindem, H., et al. (2016). “How does a combined preoperative and postoperative rehabilitation program influence the outcome of ACL reconstruction?” British Journal of Sports Medicine.
- Netball Australia’s KNEE Program
- FIFA 11+ Warm-Up Program
- Physio Network ACL Rehab Guide
- Australian Physiotherapy Association – ACL Injuries: https://australian.physio
Feeling a weird burning or zapping pain that just won’t quit? It might be nerve pain—and physio can actually help more than you think. In this blog, we’ll unpack what nerve pain really is, why it happens, and how physiotherapy can play a powerful role in calming things down.
What is Nerve Pain?
Nerve pain (also known as neuropathic pain) is one of those things that can really throw people. It’s different from the dull ache of sore muscles or the sharp stab of a sprain. It’s more like a burning, tingling, zapping, or electric shock kind of sensation. Sometimes it feels like your skin is overly sensitive. Other times, it’s like pain is coming from nowhere.
The most confusing part? The pain doesn’t always start where the problem is. For example, someone might feel pain in their foot, but the real issue could be up near the lower back or hip where the nerve is getting irritated.

Common Causes of Nerve Pain
Nerves can become irritated, compressed, or inflamed for a variety of reasons. Here are a few of the more common ones we see in clinic:
- Herniated discs: Pressure from a bulging disc can pinch a spinal nerve.
- Post-surgery changes: Scar tissue from surgery can sometimes irritate nearby nerves.
- Diabetes: Can lead to peripheral neuropathy, especially in the feet.
- Tight muscles: Believe it or not, tight muscles like the piriformis or hamstrings can entrap nerves like the sciatic or tibial nerve.
- Trauma: A direct hit or sudden stretch can irritate or even damage a nerve.
- Repetitive strain: Poor posture, long hours at a desk, or repeated movements can lead to chronic nerve irritation.

Symptoms to Watch Out For
If you’ve got nerve pain, you might notice:
- Burning or searing pain
- Pins and needles
- Tingling or numbness
- Weakness in a limb
- Shooting or zapping sensations down the arm or leg
- Sensitivity to touch (even clothes can feel painful)
Symptoms often follow the path of the affected nerve—so the location of pain can help us figure out which nerve is involved.

The Science Behind It: Why Nerves Hurt
Nerves are like the body’s communication cables. When one gets irritated, it starts sending distress signals. But here’s the thing—those signals don’t always make sense. The brain might interpret them as burning, zapping, or hypersensitivity.
Once a nerve becomes “sensitised”, it can become more reactive. This means it starts firing off pain signals even when there’s no actual danger. It’s like your body’s alarm system getting stuck on high alert.
How Physiotherapy Can Help with Nerve Pain
You might not think of physio as the go-to treatment for nerve pain—but it absolutely can be.
Here’s how we help:
1. Identify the Source
We don’t just treat the pain—we track down where it’s coming from. That might mean testing nerve mobility, looking at posture, assessing joint movement, and checking muscle tension.
2. Nerve Glides and Mobilisations
These gentle movements help the nerve slide and move more freely through its pathway. Think of it like flossing for your nerves—helping reduce tension and irritation.
3. Addressing the Root Cause
If the nerve is irritated because of a stiff joint, tight muscle, or poor biomechanics, we’ll treat that directly. This might involve hands-on therapy, stretching, strengthening, or movement retraining.
4. Postural Advice
Sometimes a simple change in how you sit or move during the day can reduce nerve tension and stop flare-ups.
5. Exercise Programming
Gradual, targeted strengthening helps support the body and reduce risk of future flare-ups. Plus, movement helps desensitise the nervous system over time.

Real Life Example: The Mysterious Burning Foot
We recently had a patient come in with a burning pain in their foot. They thought they must’ve kicked something or bruised it, but couldn’t remember doing so. The pain was constant, especially after walking or standing for long periods. Shoes made it worse. They described it as “like fire ants crawling on my foot.”
Assessment
We ruled out common things like plantar fasciitis, fractures, and local trauma. On testing, there was no obvious injury to the foot muscles or joints. But when we assessed nerve tension, we found the sural nerve was extremely sensitive.
The sural nerve runs down the back and outer part of the leg and ends near the heel and foot. Interestingly, this nerve can become irritated not just at the foot, but higher up, especially where it branches from the sciatic nerve.
Treatment
We started treatment not at the foot—but up around the sciatic nerve. We used nerve mobilisation techniques, soft tissue work to reduce tension in the hamstrings and glutes, and added some nerve gliding exercises to do at home.
Within a few sessions, the patient started noticing the burning was easing. After a couple of weeks, they could wear shoes again without pain. The best part? No injections or medication were needed—just good old-fashioned physio and a targeted plan.
Different Nerves, Different Pains
Depending on which nerve is involved, you might feel symptoms in different places. Here are a few common ones:
| Nerve | Typical Pain Area | Common Cause |
|---|---|---|
| Sciatic Nerve | Buttock, back of thigh, calf | Disc herniation, piriformis syndrome |
| Tibial Nerve | Bottom of foot, heel | Tarsal tunnel syndrome |
| Peroneal Nerve | Outer leg, top of foot | Fibular head compression |
| Sural Nerve | Outer lower leg, foot | Sciatic tension, tight calves |
| Median Nerve | Thumb, index, middle fingers | Carpal tunnel syndrome |
| Ulnar Nerve | Ring and little finger | Elbow compression (cubital tunnel) |
Knowing which nerve is involved helps us choose the right treatments—and avoid chasing the wrong problem.
How Long Does Nerve Pain Take to Settle?
This depends on:
- How long you’ve had the symptoms
- The severity of nerve irritation
- How sensitised the nervous system has become
- Whether you stick to your treatment plan
Some people feel relief in a few sessions. For others, especially if it’s been going on for months, it might take a bit longer. The key is consistency, patience, and not giving up.
What Can You Do At Home?
Here are a few self-care tips if you’re dealing with nerve pain:
- Avoid aggravating positions: Like prolonged sitting or crossing your legs if that makes it worse.
- Gentle nerve glides: Only if prescribed by your physio—these help restore normal nerve movement.
- Stay active: Light walking or swimming can help keep the nervous system happy.
- Don’t stretch too hard: Aggressive stretching can actually make nerve pain worse.
- Mind your posture: Especially if you work at a desk or spend hours in the car.
When to See a Physio
If you’re experiencing:
- Ongoing tingling, burning, or shooting pain
- Numbness or weakness in a limb
- Pain that doesn’t respond to basic rest or ice
- Pain that seems to travel or doesn’t make sense
…it’s time to book in.
We’ll do a thorough assessment, explain what’s going on in plain English, and put together a clear plan to help you feel normal again.
Final Thoughts
Nerve pain might feel scary and mysterious, but it’s often treatable without medication or surgery. Physiotherapists are trained to understand the nervous system, track down the source of your symptoms, and get you back to doing what you love.
Just like our patient with the burning foot—sometimes the pain is coming from somewhere you wouldn’t expect, and you just need the right treatment to unlock relief.
References
- Physiopedia. Neuropathic Pain
- Pain Australia. Neuropathic Pain
- British Journal of Sports Medicine. Nerve mobilisation for the treatment of pain
- Neuro Orthopaedic Institute. The Sensitive Nervous System
- Health Direct Australia. Nerve Pain
Want to know if nerve pain is behind your weird symptoms? Book an appointment today just CLICK HERE
Let us untangle your nerves (literally!).
