If you’ve developed aching along the inside of your ankle and your arch seems to be collapsing, you might be dealing with posterior tibial tendon dysfunction physiotherapy could help fix. This common but often missed condition is a leading cause of adult flat foot pain — and the earlier you treat it, the better the outcome.
Why Your Arch Is Suddenly Dropping
Adult flat foot doesn’t usually happen overnight. Most people don’t wake up one day with a completely collapsed arch. It’s gradual.
One of the biggest culprits? Posterior Tibial Tendon Dysfunction (PTTD) — now often referred to as Progressive Collapsing Foot Deformity.
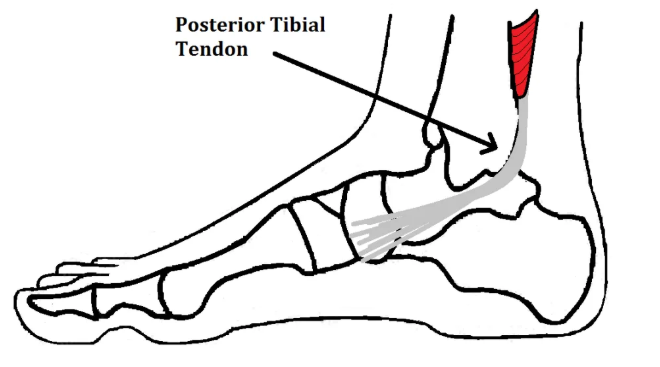
The posterior tibial tendon runs from a key calf muscle (tibialis posterior), behind the inside ankle bone, and attaches into the arch of your foot. Its job is simple but critical:
- Support your arch
- Control foot position while walking
- Help you push off when you step
When this tendon becomes overloaded, irritated, or degenerative, it can’t hold the arch up anymore. The result? Pain, weakness, and flattening of the foot.
What Is Posterior Tibial Tendon Dysfunction?
Posterior Tibial Tendon Dysfunction is a condition where the tendon gradually becomes:
- Inflamed (early stage)
- Thickened and degenerative
- Weak and unable to support the arch
Over time, this leads to:
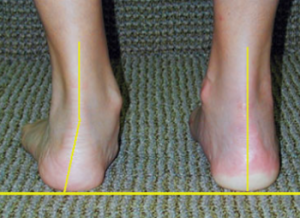
- Arch collapse
- Heel drifting outward
- Forefoot turning outward
- Difficulty standing on one leg
- Trouble doing a single heel raise
If untreated, it can become rigid and arthritic.
This is why early posterior tibial tendon dysfunction physiotherapy is crucial.
Who Is Most At Risk?
PTTD is more common in:
- Adults over 40
- Women
- Runners and walkers
- People who stand all day for work
- Those with previous ankle sprains
- People with higher body weight
- Diabetics
We commonly see it in busy tradies, nurses, teachers, and parents who are constantly on their feet.
The Early Warning Signs
Most patients tell us:
- “It started as a dull ache along the inside of my ankle.”
- “My foot feels tired and heavy.”
- “My shoes are wearing unevenly.”
- “My arch looks flatter than the other side.”
A big red flag is pain behind the inside ankle bone (medial malleolus) that worsens with walking.
Another key test: try standing on one leg and doing a heel raise. If the heel doesn’t roll inward or you can’t lift at all — that’s often posterior tibial tendon dysfunction.
What Happens If You Ignore It?
Here’s the tough truth.
If untreated, posterior tibial tendon dysfunction can progress through stages:
Stage 1
Painful tendon but normal foot shape.
Stage 2
Arch collapse begins. Foot becomes flexible flat.
Stage 3
Flat foot becomes stiff and arthritic.
Stage 4
Ankle joint involvement develops.
By Stage 3 or 4, surgery is often considered.
This is why conservative management early is so important.
How Physiotherapy Fixes Posterior Tibial Tendon Dysfunction
The good news? Most cases respond very well to targeted physiotherapy.
At our Frenchs Forest clinic, our approach to posterior tibial tendon dysfunction physiotherapy focuses on:
1. Reducing Tendon Load
Early on, we may modify activity and temporarily reduce aggravating loads. That doesn’t mean complete rest — it means smart load management.
2. Strengthening the Tibialis Posterior
The tendon needs progressive loading. Research shows tendons respond positively to the right strengthening program.
Key exercises include:
- Resisted foot inversion
- Heel raises (progressing to single-leg)
- Slow controlled calf raises
- Arch control drills
3. Foot Intrinsic Muscle Training
Strengthening the small stabilisers in the foot helps support the arch naturally.
4. Ankle and Calf Mobility
Restricted ankle dorsiflexion increases strain on the tendon. Improving mobility reduces stress.
5. Taping or Temporary Orthotics
Short-term arch support can unload the tendon while it heals.
6. Gait Retraining
Subtle walking changes can significantly reduce medial foot overload.
A Recent Patient Story (Frenchs Forest NSW)
Recently, we saw a 52-year-old woman who travelled from a surrounding suburb near Frenchs Forest NSW. She works in retail and stands all day.
She came in with:
- 6 months of inner ankle pain
- Progressive flattening of her right arch
- Inability to do a single heel raise
- Increasing difficulty walking more than 20 minutes
She had been told she “just had flat feet.”
After assessment, we diagnosed Stage 2 posterior tibial tendon dysfunction.
Her treatment plan included:
- Load modification (reducing long walking initially)
- Structured strengthening program
- Calf and tibialis posterior progressive loading
- Temporary arch taping
- Education around footwear
Within 4 weeks, pain reduced significantly.
By 8 weeks, she could perform 15 single-leg heel raises.
At 12 weeks, she returned to full work shifts pain-free.
The key? Early, progressive physiotherapy rather than ignoring it or relying purely on passive supports.
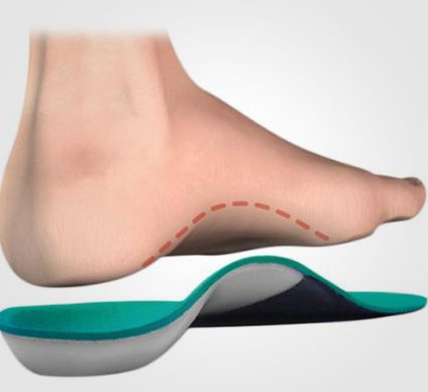
Do Orthotics Fix It?
Orthotics can help — but they are not the full solution.
They reduce strain on the tendon temporarily. However:
- They don’t strengthen the tendon
- They don’t improve muscle control
- They don’t address mobility deficits
The best outcomes occur when orthotics are combined with active rehabilitation.
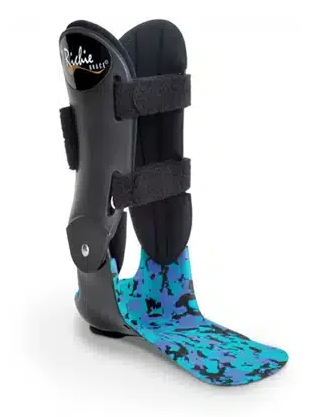
What is a Richie Brace?
In more advanced or stubborn cases, we sometimes discuss the use of a Richie Brace. A Richie Brace is a custom-made ankle-foot orthosis (AFO) that combines a supportive foot orthotic with semi-rigid uprights that stabilise the ankle. It’s typically used in moderate to more advanced posterior tibial tendon dysfunction where the arch is significantly collapsing and the tendon needs substantial offloading. The goal isn’t to rely on it forever — it’s to reduce strain enough to calm symptoms while we continue strengthening and rehabilitation. For some patients, particularly those wanting to avoid surgery, a Richie Brace can be an effective middle-ground option alongside physiotherapy.
Can It Heal Without Surgery?
Yes — especially in Stages 1 and 2.
Evidence supports exercise-based tendon rehab for tendon dysfunction conditions, similar to what we use in Achilles and patellar tendinopathy.
Surgery is usually considered only when:
- Conservative care fails
- Deformity becomes rigid
- Severe arthritis develops
Most people we see respond well to a 8–16 week progressive rehab program.
Footwear Matters More Than You Think
Shoes that are:
- Too flexible
- Worn out
- Completely flat
- Minimal support
can worsen tendon overload.
We often recommend:
- Firm heel counter
- Mild arch support
- Structured midsole
- Avoiding very flexible minimalist shoes during rehab
How Long Does Recovery Take?
It depends on:
- Stage of dysfunction
- Duration of symptoms
- Compliance with rehab
- Body load and activity demands
General guide:
- Mild cases: 6–8 weeks
- Moderate cases: 8–16 weeks
- Chronic cases: 3–6 months
Consistency is key.
Why Early Physiotherapy Matters
The longer you wait:
- The more the arch collapses
- The harder it becomes to reverse
- The greater the risk of joint damage
Early posterior tibial tendon dysfunction physiotherapy can stop progression and restore strength before permanent changes occur.
When Should You Book In?
You should get assessed if:
- You have pain along the inside of your ankle
- Your arch is dropping
- You struggle with heel raises
- Walking distance is reducing
- You’ve had repeated ankle sprains
Don’t wait until it becomes rigid and painful daily.
FAQs – Posterior Tibial Tendon Dysfunction
What is posterior tibial tendon dysfunction?
Posterior tibial tendon dysfunction is a condition where the tendon supporting your arch becomes inflamed or degenerative, leading to adult flat foot and inner ankle pain.
Can physiotherapy fix posterior tibial tendon dysfunction?
Yes. Early-stage PTTD responds very well to progressive strengthening, load management, and foot control retraining.
How long does posterior tibial tendon dysfunction take to heal?
Most cases improve within 8–16 weeks with consistent physiotherapy. More advanced cases may take longer.
Do I need orthotics for posterior tibial tendon dysfunction?
Orthotics can help reduce strain but work best when combined with strengthening and rehabilitation exercises.
Can posterior tibial tendon dysfunction cause permanent flat feet?
If left untreated, it can lead to progressive arch collapse and arthritis. Early treatment reduces this risk significantly.
References
- American Academy of Orthopaedic Surgeons – Posterior Tibial Tendon Dysfunction
https://orthoinfo.aaos.org - Cleveland Clinic – Posterior Tibial Tendonitis
https://my.clevelandclinic.org - Journal of Orthopaedic & Sports Physical Therapy – Tendon Rehabilitation Guidelines
https://www.jospt.org - X-Physio Blog – Snapping Hip Syndrome
https://xphysio.com.au/blog
If you’re noticing arch collapse or inside ankle pain, don’t wait for it to get worse.
Give us a call today on 9806 3077, or book online, just CLICK HERE: https://x-physio.au4.cliniko.com/bookings#service
Woken up and suddenly can’t turn your head? You’ve likely developed a wry neck (acute torticollis). It’s painful, stiff, and frustrating — but the good news is it’s usually very treatable. In this blog, we’ll explain exactly what causes it, what to do immediately, and how physiotherapy can speed up your recovery.
Woke Up Crooked? You’re Not Alone.
There’s nothing quite like that moment.
You roll over in bed… and realise your neck won’t move. One side feels locked. Turning your head sends a sharp jolt of pain. You’re stuck looking slightly sideways like you’ve permanently spotted something interesting.
This is wry neck, also known as acute torticollis — a common condition we see regularly in clinic.
The good news?
It’s rarely serious.
And with the right wry neck treatment, most people improve quickly.
Let’s break it down.

What Is Wry Neck (Acute Torticollis)?
Wry neck is a sudden onset neck spasm that causes your head to tilt or rotate to one side. The medical term is acute torticollis.
It usually:
- Appears suddenly (often overnight)
- Causes sharp pain on one side of the neck
- Limits rotation (you can’t turn your head properly)
- Feels “locked” or stuck
The muscles most commonly involved include:
- Upper trapezius
- Levator scapulae
- Sternocleidomastoid
- Deep cervical muscles
When these muscles go into protective spasm, movement becomes painful and restricted.
What Causes Wry Neck?
Most cases happen for simple mechanical reasons. Common triggers include:
1. Sleeping Position
Awkward pillow height or sleeping twisted can irritate joints and soft tissues.
2. Sudden Movement
Quick head turn, sport, gym movement, or even reversing the car.
3. Joint Irritation
Minor facet joint irritation in the cervical spine can trigger reflex muscle spasm.
4. Stress & Tension
High stress can increase muscle tone in the neck and shoulders.
5. Prolonged Posture
Long hours at a desk, laptop, or phone can overload neck structures.
It’s often a combination of factors rather than one clear cause.

What’s Actually Happening in Your Neck?
In simple terms:
- A small joint or structure becomes irritated.
- The nervous system reacts.
- Muscles tighten to protect the area.
- Movement becomes restricted and painful.
The muscle spasm isn’t the primary problem — it’s your body’s protective response.
That’s why simply stretching aggressively often makes it worse.
What To Do Immediately (First 24–48 Hours)
If you wake up with a wry neck, here’s what we recommend.
✅ Keep Moving (Gently)
Avoid forcing movement, but don’t completely immobilise it either. Small pain-free movements help calm the nervous system.
✅ Use Heat
A warm pack for 10–15 minutes can relax muscle spasm.
✅ Simple Pain Relief
Paracetamol or anti-inflammatories (if safe for you) may help.
❌ Avoid Aggressive Stretching
Cranking your head into the painful direction can flare it.
❌ Avoid Complete Rest
Staying still all day stiffens it further.
If it’s not improving within 48–72 hours — or if pain is severe — physiotherapy helps significantly.

When Should You See a Physio?
Seek assessment if:
- Pain is severe
- You can’t rotate your head at all
- It’s not improving after 2–3 days
- You get pins and needles or arm symptoms
- It keeps recurring
Most cases are mechanical and straightforward — but proper assessment ensures nothing more serious is going on.
How Physiotherapy Helps Wry Neck Treatment
This is where we see the biggest improvements.
Effective wry neck treatment isn’t just massage. It’s targeted, specific care.
1. Accurate Diagnosis
We assess:
- Cervical joint mobility
- Muscle tone
- Neural involvement
- Postural drivers
- Contributing factors
2. Gentle Joint Mobilisation
Specific hands-on techniques reduce joint irritation and reset movement.
3. Muscle Release
Targeted soft tissue work reduces protective spasm.
4. Movement Retraining
We guide safe movement patterns to restore normal range.
5. Education
Understanding what’s happening reduces fear and muscle guarding.
A Recent Case From Our Clinic
Just last month, we saw a 42-year-old patient who drove from Roseville to our clinic in Frenchs Forest NSW after waking up unable to turn her head.
She’d slept awkwardly after a long week at work. By morning, her head was stuck rotated to the right. Pain was sharp and she couldn’t check her blind spot while driving.
Assessment showed:
- Acute facet joint irritation
- Significant levator scapulae spasm
- No nerve involvement
We performed:
- Gentle cervical joint mobilisation
- Soft tissue release
- Guided active movement exercises
- Postural advice for her workstation
Within the first session, rotation improved by about 50%.
By her second visit 4 days later, she had near full movement.
One week later, she was back at Pilates pain-free.
This is typical when treatment is early and targeted.
How Long Does Wry Neck Last?
Without treatment:
- Mild cases: 3–7 days
- Moderate cases: 1–2 weeks
With physiotherapy:
- Often significantly reduced
- Faster return to full movement
- Lower chance of recurrence
The key is calming irritation early and restoring normal movement quickly.
Can Wry Neck Become Chronic?
Occasionally, yes — especially if:
- It’s left untreated
- Poor posture persists
- There’s repeated strain
- Underlying cervical stiffness exists
Recurrent episodes usually indicate an underlying mobility or control issue.
That’s where a tailored strengthening program matters.
Exercises for Wry Neck (Once Pain Settles)
These are general examples — individual assessment is best.
1. Gentle Rotation
Turn head slowly toward comfortable range.
10 reps, 3–4 times daily.
2. Chin Tucks
Gently retract chin (like making a double chin).
Hold 5 seconds, repeat 10 times.
3. Scapular Setting
Draw shoulder blades gently back and down.
These help restore control and reduce recurrence risk.

Prevention Tips
To reduce future episodes:
- Optimise pillow height (neutral alignment)
- Avoid stomach sleeping
- Improve desk ergonomics
- Take movement breaks every 30–45 mins
- Strengthen deep neck flexors
- Manage stress load
Small changes make a big difference.
Red Flags (Rare but Important)
Seek urgent medical review if you experience:
- Fever
- Severe headache
- Trauma
- Neurological symptoms
- Unexplained weight loss
- History of cancer
These are uncommon but important to rule out.
Why Early Wry Neck Treatment Matters
The longer muscle spasm persists, the more the nervous system sensitises.
Early physiotherapy:
- Reduces pain faster
- Restores movement sooner
- Prevents compensation patterns
- Lowers recurrence risk
Don’t wait it out unnecessarily.
Frequently Asked Questions (FAQs)
What is the fastest way to fix a wry neck?
Gentle movement, heat, and physiotherapy treatment provide the fastest improvement. Hands-on mobilisation combined with guided exercises usually speeds recovery significantly.
Should I massage a wry neck?
Light massage may help, but aggressive pressure can worsen irritation. It’s best combined with joint mobilisation and movement therapy.
Is wry neck serious?
In most cases, no. It’s usually a temporary mechanical issue. However, if symptoms are severe or accompanied by neurological signs, seek assessment.
Can I exercise with a wry neck?
Avoid intense workouts initially. Gentle movement is beneficial, but heavy lifting or high-impact activity should wait until pain settles.
How many physio sessions do I need?
Many patients improve within 1–3 sessions depending on severity.
References
- https://www.healthdirect.gov.au/torticollis
- https://www.nhs.uk/conditions/torticollis/
- https://www.physio-pedia.com/Torticollis
- https://xphysio.com.au/blog/
If you’ve woken up stuck and sore — don’t just wait and hope.
Early, targeted wry neck treatment makes a huge difference.
Give us a call today on 9806 3077, or book online, just CLICK HERE:
https://x-physio.au4.cliniko.com/bookings#service
Snapping hip syndrome is a common cause of clicking, flicking or popping around the hip — especially in runners, dancers and gym-goers. While it’s often painless at first, it can become irritating and stubborn. The good news? With the right physiotherapy approach, you can settle it down and stop the click for good.
That Annoying Click in the Hip…
You’re walking up stairs.
You swing your leg out of the car.
You go to stand up after sitting.
Click.
If that sound (or feeling) keeps happening around the front or side of your hip, you might be dealing with snapping hip syndrome.
For some people, it’s just a harmless noise. For others, it becomes painful, inflamed and frustrating — especially when it starts limiting training or daily movement.
Let’s break down what’s actually happening, why it won’t go away on its own, and how physiotherapy can fix it properly.

What Is Snapping Hip Syndrome?
Snapping hip syndrome (sometimes called coxa saltans) is when a tendon flicks over a bony structure in the hip, creating a snapping or clicking sensation.
There are three main types:
1️⃣ External Snapping Hip
The most common type.
The iliotibial band (ITB) or gluteus maximus tendon snaps over the outside of the hip bone (greater trochanter).
You’ll usually feel:
- A snap on the outside of the hip
- Clicking when walking or running
- Tenderness on the side of the hip
This often overlaps with ITB irritation or lateral hip pain.
2️⃣ Internal Snapping Hip
This happens when the iliopsoas tendon flicks over structures at the front of the hip.
You’ll notice:
- A deep click in the front of the hip
- Snapping when lifting the knee
- Clicking getting out of a car
- Tight hip flexors
This is common in runners, dancers and people who sit a lot.
3️⃣ Intra-Articular Snapping
Less common, but more serious.
This involves something inside the joint — like a labral tear or cartilage issue.
These patients often describe:
- Catching or locking
- Deep joint pain
- Reduced hip range
- Sharp pain with twisting
This type requires careful assessment and sometimes imaging.
Why Does Snapping Hip Syndrome Happen?
Snapping hip syndrome usually develops because of:
- Muscle tightness (especially hip flexors or ITB)
- Weak glutes
- Poor pelvic control
- Overtraining
- Sudden training load increases
- Biomechanical overload
- Long hours sitting
In active Australians, it’s often a mix of tight hip flexors + weak glutes + increased training volume.
The tendon starts to flick repeatedly over bone — and over time that repeated friction causes irritation and inflammation.
That’s when the painless click becomes painful snapping.
If the hip is not snapping but is sore on the outside, READ THIS BLOG
Why It Won’t Just “Go Away”
Here’s the trap.
Many people think:
“It’s just a click. I’ll stretch it.”
But stretching alone rarely fixes snapping hip syndrome.
Why?
Because the underlying problem isn’t just tightness. It’s usually:
- Load imbalance
- Weak lateral hip stabilisers
- Poor movement control
- Pelvic positioning issues
Unless you address those, the tendon keeps snapping.
And if it continues long enough, you can develop:
- Trochanteric bursitis
- Hip flexor tendinopathy
- Gluteal tendinopathy
- Ongoing hip pain with sport
That’s why early physio treatment makes such a big difference.

What We Saw Recently in Clinic (Real Patient Example)
A 32-year-old runner came to see us from a nearby Northern Beaches suburb to our clinic in Frenchs Forest NSW.
She’d had a clicking hip for about 8 months.
At first it was painless. Then it started aching after long runs.
Eventually, she felt sharp snapping every time she lifted her knee.
She had:
- Tight hip flexors
- Weak glute medius
- Reduced single-leg control
- Poor pelvic stability on running assessment
Her MRI was clear — no labral tear. That was good news.
We treated her snapping hip syndrome with:
- Targeted hip flexor release
- Progressive glute strengthening
- Pelvic stability retraining
- Running load modification
- Gradual return-to-run programming
Within 4 weeks:
- Clicking reduced significantly
- Pain resolved
- Running tolerance improved
By 8 weeks:
- No snapping during daily movement
- Returned to full training
The key wasn’t stretching alone. It was correcting the underlying load and control problem.
How Physiotherapy Fixes Snapping Hip Syndrome
Here’s how we approach snapping hip syndrome properly.
1️⃣ Accurate Diagnosis
First, we determine:
- External vs internal vs intra-articular
- Is it painful or just audible?
- Is there tendon irritation?
- Do we need imaging?
A proper assessment prevents misdiagnosis.
2️⃣ Reduce Irritation
Early stage management may include:
- Activity modification
- Load reduction
- Soft tissue release
- Dry needling (if appropriate)
- Taping strategies
The goal: calm the tissue down.
3️⃣ Restore Strength
This is where most people fall short.
We focus heavily on:
- Glute medius
- Glute max
- Deep hip rotators
- Core stability
- Single-leg strength
Strength reduces the flicking force over the bone.
4️⃣ Improve Movement Control
We retrain:
- Single-leg squats
- Running gait
- Pelvic positioning
- Hip hinge mechanics
Movement retraining is often the missing piece.
5️⃣ Return to Sport Plan
For runners and athletes:
- Controlled load progression
- Monitoring symptoms
- Specific hip capacity work
This prevents recurrence.

Can You Exercise Through It?
If snapping hip syndrome is painless, you can often continue training with modifications.
If it’s painful:
- Avoid repeated snapping motions
- Reduce hills or speed work
- Avoid deep hip flexion temporarily
Painful snapping should not be ignored — especially if worsening.
How Long Does It Take to Fix?
Typical timelines:
- Mild cases: 3–6 weeks
- Moderate cases: 6–10 weeks
- Long-standing cases: 8–12+ weeks
The longer it’s been present, the longer it usually takes to correct.
When Should You Be Concerned?
Seek assessment if you notice:
- Locking or catching
- Sharp groin pain
- Sudden onset after trauma
- Persistent swelling
- Pain that doesn’t settle
These may indicate intra-articular involvement.
Self-Management Tips (That Actually Help)
If you suspect snapping hip syndrome:
✔ Strengthen glutes (not just stretch hip flexors)
✔ Avoid aggressive stretching if painful
✔ Reduce load temporarily
✔ Work on single-leg stability
✔ Don’t ignore progressive symptoms
But if it’s been there more than a few weeks — get it assessed.
Why Early Treatment Matters
When treated early, snapping hip syndrome responds very well.
Left untreated, it can turn into:
- Chronic lateral hip pain
- Tendinopathy
- Ongoing running issues
- Compensatory knee or back pain
Fix the cause, not just the click.
The Bottom Line
Snapping hip syndrome is common, annoying, and very fixable.
The clicking hip that “won’t go away” usually sticks around because the underlying strength and control issues haven’t been addressed.
With targeted physiotherapy, proper loading and progressive strength work, most people return to full activity without surgery.
If your hip keeps clicking — and especially if it’s starting to hurt — don’t wait.
FAQs About Snapping Hip Syndrome
What is snapping hip syndrome?
Snapping hip syndrome is a condition where a tendon flicks over a bony structure in the hip, causing a clicking or snapping sensation. It can be painless or painful and is common in runners and active individuals.
Is snapping hip syndrome serious?
It is usually not serious, especially if painless. However, if it becomes painful or is associated with locking or catching, it should be assessed by a physiotherapist or doctor.
Can snapping hip syndrome go away on its own?
Mild painless snapping may settle with load reduction. Painful snapping hip syndrome typically requires physiotherapy to correct muscle imbalances and movement control issues.
What exercises help snapping hip syndrome?
Glute strengthening, pelvic stability exercises, and controlled single-leg training are most effective. Stretching alone is rarely enough.
Do I need surgery for snapping hip syndrome?
Surgery is rarely required. Most cases respond well to physiotherapy and structured rehabilitation.
References
- https://www.physio-pedia.com/Snapping_Hip_Syndrome
- https://orthoinfo.aaos.org/en/diseases–conditions/snapping-hip/
- https://www.sportsinjuryclinic.net/sport-injuries/hip-groin-pain/snapping-hip
If you’re dealing with snapping hip syndrome and it’s not settling, our physios in Frenchs Forest can help identify the cause and build a clear plan to get you back to full strength.
Give us a call today on 9806 3077, or book online, just CLICK HERE: https://x-physio.au4.cliniko.com/bookings#service
A bone bruise is deeper than a muscle strain but not quite a fracture — which is exactly why it hangs around. The bone’s internal structure gets damaged and heals slowly. In this guide we’ll explain why pain lingers, what speeds recovery up, and how physio gets you moving sooner. If your injury isn’t settling… keep reading.
What is a Bone Bruise?
A bone bruise (also called a bone contusion) is damage to the inside of the bone.
Think of bone like a honeycomb — not solid concrete. When force hits it (fall, tackle, twist, awkward landing), tiny internal trabeculae collapse and bleed.
You haven’t broken the bone — but you’ve injured the structure.
That’s why it hurts far more than a sprain but looks normal on X-ray.
Bone bruises commonly occur in:
- Knee (most common — especially after sport)
- Heel after landing
- Hip after a fall
- Wrist after catching yourself
- Ankle after rolling it
- Shoulder after impact
Why Does a Bone Bruise Hurt for So Long?
This is the big frustration.
People expect soft tissue healing timelines:
- Muscle: 2–4 weeks
- Ligament: 4–8 weeks
But bone bruises often last 2–6 months.
Here’s why.
1. Bones Have Poor Blood Flow
Muscle heals quickly because it’s rich in blood supply.
Bone marrow? Not so much.
Healing cells physically take longer to arrive.
2. Every Step Compresses the Injury
Unlike a muscle tear where rest helps — you load bones every time you stand, walk, or climb stairs.
So the injury gets micro-irritated daily.
3. Swelling is Trapped Inside Bone
Soft tissue swelling can disperse.
Bone swelling is trapped under rigid cortex → pressure → deep aching pain.
That classic complaint:
“It feels bruised inside, especially at night.”
Exactly right.
4. MRI Changes Persist After Symptoms Improve
A key point — pain and healing don’t progress together.
Even once you feel better, bone remodelling continues for months.
Return too fast → flare up.
This is where physiotherapy becomes critical.
Symptoms of a Bone Bruise
Typical features include:
- Deep ache rather than sharp pain
- Pain with weight-bearing
- Worse after activity, stiff the next day
- Night throbbing
- Localised tenderness over bone
- Swelling without major instability
- Slow improvement plateau
The giveaway sign:
You were improving… then it just stopped.
Classic bone bruise behaviour.
To find out more info about a bone fracture, CLICK HERE
Why Rest Alone Doesn’t Fix It
Many people are told:
“Just rest and let it heal.”
The problem?
Total rest weakens the surrounding muscles → more load goes through the bone → recovery slows.
Bone actually heals best with controlled progressive loading.
Not zero load.
Not full sport.
But smart loading.
That’s physiotherapy.

How Physiotherapy Speeds Bone Bruise Recovery
At our clinic in Frenchs Forest, we manage bone bruises weekly — especially knees and heels.
Physio treatment works in 4 stages.
Stage 1 — Settle Irritation (Week 0–2)
Goal: Reduce internal bone pressure
We use:
- Load modification (not full rest)
- Crutch or taping advice
- Range of motion drills
- Muscle activation without compression
- Pool walking or cycling
- Pain-guided activity limits
Important:
You should still move — just not aggravate.
Stage 2 — Restore Movement (Week 2–6)
Now we improve joint mechanics so force spreads better.
Common problems:
- Stiff ankle → overload knee bone bruise
- Weak glutes → overload hip
- Poor quad control → overload patella
Treatment includes:
- Joint mobilisation
- Strength activation patterns
- Gait retraining
- Controlled weight-bearing progressions
Pain often drops dramatically here.
Stage 3 — Load the Bone Properly (Week 4–10)
This is the most important stage — and the one most people skip.
Bone remodels in response to progressive compression.
We introduce:
- Isometric loading
- Slow resistance strength
- Step-down progressions
- Controlled impact preparation
This stimulates healing instead of delaying it.
Stage 4 — Return to Impact (Week 8–16+)
Gradual return:
- Jog → run intervals
- Landing mechanics
- Deceleration training
- Sport-specific drills
Skipping this stage = relapse.

Real Patient Example
A 34-year-old runner came to us from Belrose with persistent knee pain after slipping on wet tiles 8 weeks earlier.
They’d been told:
“Probably just bruised — give it time.”
But time didn’t help.
Findings
- MRI: medial femoral condyle bone bruise
- Quad inhibition
- Avoidance gait
- Pain climbing stairs
- Unable to run
Treatment Plan
Weeks 1–2
Unload + restore quad activation
Weeks 3–6
Strength + controlled knee loading
Weeks 6–10
Running re-introduction program
Weeks 10–12
Return to park run
Outcome
- Running 5km pain-free
- No swelling
- Confidence restored
The biggest change?
They stopped resting completely and started graded loading.
Exercises That Help Bone Bruise Recovery
(Always guided — wrong load irritates bone)
Early Phase
- Static quad holds
- Glute bridges
- Heel slides
- Pool walking
Mid Phase
- Sit-to-stands
- Step-ups
- Resistance band walking
- Leg press (partial range)
Late Phase
- Split squats
- Single leg deadlifts
- Hopping drills
- Jog progressions
What Makes Bone Bruises Worse?
Avoid these mistakes:
❌ Complete rest for weeks
❌ Running “through discomfort”
❌ Stretching aggressively over bone
❌ Returning once pain reduces (too early)
❌ Ignoring strength deficits
How Long Does a Bone Bruise Take to Heal?
Typical timelines:
| Severity | Healing Time |
|---|---|
| Mild | 4–8 weeks |
| Moderate | 2–4 months |
| Severe | 4–9 months |
Key rule:
Pain settles before bone finishes healing.
We progress based on load tolerance — not MRI images.
Do You Need a Scan?
You may need MRI if:
- Pain lasts >4 weeks after impact
- Deep localised tenderness
- Night ache persists
- Swelling unexplained
- X-ray normal but pain severe
X-rays don’t show bone bruises.
Preventing Recurrence
Bone bruises often come back because the real cause wasn’t fixed.
We address:
- Landing mechanics
- Muscle imbalance
- Joint stiffness
- Running load errors
- Foot control
Once corrected → recurrence risk drops massively.
When to See a Physio
Book an assessment if:
- Pain lingers beyond 2–3 weeks
- You plateau in recovery
- Running keeps flaring symptoms
- Night pain persists
- Swelling returns after activity
Early treatment shortens recovery by months.
FAQs About Bone Bruises
How is a bone bruise different from a fracture?
A fracture breaks the bone cortex. A bone bruise damages the internal structure but keeps the outer shell intact.
Can you walk on a bone bruise?
Usually yes — but load must be controlled. Too much walking delays healing.
Should I ice a bone bruise?
Ice helps pain early but won’t speed healing significantly after the first week.
Why does it hurt more at night?
Bone pressure increases when circulation changes and muscles relax.
Can I run with a bone bruise?
Only during staged rehab. Running too early commonly resets recovery.
Do bone bruises show on X-ray?
No. They require MRI.
Does physio actually speed healing?
Yes — by optimising load, strength, and mechanics so bone remodelling occurs faster.
References
- https://www.ncbi.nlm.nih.gov/books/NBK532251/
- https://orthoinfo.aaos.org/en/diseases–conditions/bone-bruise/
- https://www.physio-pedia.com/Bone_Bruise
- https://bjsm.bmj.com/
- https://www.sportsmed.org/
Give us a call today on 9806 3077, or book online, just CLICK HERE
Shin pain after running or sport is usually either shin splints vs stress fracture — but they’re treated very differently. One needs load management and strengthening, the other often needs strict protection. In this blog we’ll show you how physio accurately diagnoses the difference and gets you back to training safely — faster.
If you’ve ever tried to “run through” shin pain, you already know the result… it just gets worse.
One of the most common mistakes we see in clinic is people guessing what their shin pain is. They Google, ice it, rest for a few days, then go back — only to flare it again. Sometimes for months.
Here’s the problem:
shin splints vs stress fracture are easy to confuse — but treating them the same can delay recovery by weeks… or even cause a full fracture.
Let’s break it down clearly.

First — What Actually Hurts In Your Shin?
Your shin bone is the tibia. Around it sit muscles, fascia and bone tissue that all react differently to load.
When running or jumping, the tibia bends slightly with every step. Normally, your body repairs that micro-damage overnight.
But if training load increases faster than your body adapts → tissue overload occurs.
That overload becomes either:
| Condition | Tissue Problem |
|---|---|
| Shin Splints | Irritated muscle & bone lining |
| Stress Fracture | Small crack inside bone |
They start from the same cause — training load error — but end very differently.
What Are Shin Splints vs Stress Fracture? (Medial Tibial Stress Syndrome)
Shin splints vs Stress Fracture is very different. Shin splints is an irritation of the bone lining (periosteum) and muscle attachment along the inside of the shin.
Typical Symptoms
- Dull ache along inner shin
- Pain warms up then settles during exercise
- Worse the next morning
- Tender along a wide area (5–10cm strip)
- Both legs often affected
Most runners describe it as:
“tight, sore, annoying — but I can still run”
That’s why people ignore it… and that’s why it progresses.
What’s Happening Physically
Your calf and deep tibial muscles pull repeatedly on the bone.
Instead of the bone breaking — the attachment tissue becomes irritated.
Think of it as shin overload warning stage.

What Is A Stress Fracture?
A stress fracture is bone fatigue failure — a small crack caused by repetitive loading exceeding bone repair. Shin Splints vs Stress fracture are often mistaken for one another.
Typical Symptoms
- Sharp, localised pain
- Pain increases during activity
- Pain doesn’t warm up
- Hurts hopping
- Often one exact fingertip spot
- Can ache at rest or night
Patients often say:
“It feels like someone is poking the bone”
This is not a warning stage anymore — it’s structural damage.
The Biggest Diagnostic Clue (You Can Try Now)
Hop Test
If hopping is painful → suspect stress fracture
If hopping is uncomfortable but tolerable → more likely shin splints vs stress fracture
But this is NOT enough alone — because missing a stress fracture is risky.
This is exactly where physiotherapy matters.
Why People Misdiagnose Themselves
Most runners think:
“If I can still run, it’s just shin splints”
Unfortunately… that’s wrong.
We regularly see runners continue training on early stress fractures for 4–6 weeks because the pain wasn’t severe initially.
By the time they come in — recovery takes 12 weeks instead of 4.
How Physiotherapy Diagnoses Shin Splints vs Stress Fracture
At XPhysio in Frenchs Forest, we don’t rely on guesswork.
We combine clinical testing + loading history + physical response patterns.
Step 1 — Load History Analysis
We map:
- Weekly distance changes
- Surface change (road → track)
- Shoe changes
- Hill work
- Speed sessions
- Sport pre-season spikes
Stress fractures nearly always follow a sudden spike.
Step 2 — Palpation Mapping
We physically map pain location:
| Finding | Suggests |
|---|---|
| Broad tenderness | Shin splints |
| Fingertip pain | Stress fracture |
Step 3 — Functional Testing
We test:
- Single leg hop
- Calf endurance
- Tibial torsion stress
- Landing mechanics
Stress fractures fail impact tests early.
Step 4 — Medical Imaging (If Needed)
If fracture suspected → GP referral for imaging.
Important note:
Early X-rays are often negative — so we guide correct scan timing.

Treatment Is Completely Different
This is why correct diagnosis matters.
Shin Splints vs stress fracture Treatment
Goal = reduce irritation + improve load capacity
- Activity modification (not full rest)
- Calf strength rebuilding
- Tibial loading progression
- Running retraining
- Foot strike & cadence changes
- Gradual return to running
Recovery: 2–6 weeks
You usually keep training in some capacity.
Stress Fracture Treatment
Goal = protect bone healing
- Impact unloading
- Cross training only
- Staged bone loading program
- Strength rebuild
- Controlled return to impact
Recovery: 6–12+ weeks
Running through it delays healing dramatically.
Real Patient Example
A 29-year-old runner came to us from Dee Why after 8 weeks of persistent shin pain. We had to figure out if it was shin splints vs stress fracture.
They’d been told it was shin splints and kept running 3–4 times per week.
During assessment:
- Fingertip pain over tibia
- Pain hopping
- Increasing night ache
We suspected stress fracture and arranged imaging — confirmed early tibial stress fracture.
Instead of needing 3 months off, we:
- Immediately unloaded impact
- Maintained cardio via cycling
- Introduced staged bone loading
- Gradually reintroduced running at week 5
They completed a 10km event pain-free 10 weeks later.
If they kept running another month → likely full fracture.
Why These Injuries Keep Coming Back
The real issue is rarely just the shin.
Common root causes:
- Weak calf endurance
- Poor shock absorption
- Sudden training spikes
- Low cadence running
- Hip control deficits
- Inadequate recovery
If you only rest — it returns.
How Physiotherapy Prevents Recurrence
Your rehab shouldn’t end when pain stops.
We build:
- Load tolerance
- Impact capacity
- Running efficiency
- Training planning skills
Most runners relapse because they never improved tissue capacity — only waited for pain to settle.
To learn more about this injury, CLICK HERE for our other blog on this topic.

The Return To Running Plan (Simplified)
Phase 1 — Calm Tissue
Bike / swim / gym only
Phase 2 — Load The Bone
Walking impact drills
Phase 3 — Reintroduce Running
Walk-run intervals
Phase 4 — Build Distance
Volume before speed
Phase 5 — Performance
Speed & hills
Skipping phases = relapse.
When To Seek Physio Immediately
Book ASAP if:
- Pain worsening week to week
- Pain in one exact spot
- Pain hopping
- Pain at rest
- Pain lasting >10 days
Early diagnosis shortens recovery massively.
FAQs
How do I know if I have shin splints or a stress fracture?
Shin splints usually feel like a broad ache that warms up with activity. Stress fractures feel sharp, localised and worsen during impact or hopping.
Can I run with shin splints?
Often yes — but load must be modified and rehab started early to prevent progression into a stress fracture.
Can shin splints turn into a stress fracture?
Yes. They’re part of the same overload spectrum. Ignoring shin splints is the most common cause of tibial stress fractures.
Do stress fractures always need a boot?
Not always. Early detection often avoids immobilisation and allows controlled loading rehab.
How long does recovery take?
Shin splints: 2–6 weeks
Stress fracture: 6–12+ weeks depending on severity
References
- https://www.sportsmedaustralia.com.au
- https://www.ais.gov.au/health-wellbeing/injury
- https://www.mayoclinic.org
- https://www.nhs.uk/conditions/stress-fractures/
- https://bjsm.bmj.com
Give us a call today on 9806 3077, or book online, just CLICK HERE with the hyperlink: https://x-physio.au4.cliniko.com/bookings#service
Golfers elbow vs Tennis elbow both cause annoying elbow pain — but they’re actually different injuries needing slightly different rehab. The good news? Physiotherapy works extremely well for both. In this guide you’ll learn how to tell them apart, what really fixes them, and how to stop them coming back. If your elbow’s been nagging — keep reading.
First — What’s the Difference?
Despite the sporting names, most people who get these injuries don’t even play golf or tennis.
They’re overuse tendon injuries caused by repetitive gripping, lifting, typing, tools, gym, or parenting.
| Condition | Location of Pain | Tendon Involved | Common In |
|---|---|---|---|
| Tennis Elbow (Lateral Epicondylitis) | Outside of elbow | Wrist extensors | Office workers, gym, racquet sports, tradies |
| Golfers Elbow (Medial Epicondylitis) | Inside of elbow | Wrist flexors | Manual labour, lifting, gripping, climbers |
So when people search “golfers elbow vs tennis elbow”, the key difference is simple:
👉 Outside pain = Tennis elbow
👉 Inside pain = Golfers elbow
But the treatment approach is similar — because both are tendon overload injuries (tendinopathy).

Why These Injuries Happen (The Real Cause)
It’s not inflammation anymore — research shows these are load tolerance problems.
Your tendon becomes weaker than the demand placed on it.
This happens when:
- You suddenly increase activity (gym, golf, DIY projects)
- Long hours gripping (mouse, tools, steering wheel)
- Poor technique
- Weak forearm or shoulder muscles
- Returning to sport too fast
- Poor recovery
The tendon starts degenerating rather than healing.
That’s why rest alone doesn’t fix it.

Symptoms: How to Tell Which One You Have
Tennis Elbow Symptoms
- Pain outside elbow
- Pain lifting kettle or coffee cup
- Weak grip strength
- Pain shaking hands
- Clicking mouse hurts
- Pain with wrist extension
Golfers Elbow Symptoms
- Pain inside elbow
- Pain gripping or squeezing
- Pain lifting weights palm-up
- Forearm tightness
- Tender to touch inside elbow
- Sometimes tingling in ring/little finger
- To learn more about Golfers Elbow – CLICK HERE and read out blog on it
Why It Doesn’t Heal By Itself
Many patients tell us:
“I rested it for months and it came straight back”
Because tendons don’t need rest.
They need progressive loading.
Without the right load:
- Tendon fibres become disorganised
- Pain sensitivity increases
- Strength decreases
- It keeps recurring
Physiotherapy fixes this by rebuilding tendon capacity.
Physiotherapy Assessment (What We Look For)
At XPhysio Frenchs Forest, we don’t just poke the elbow.
We assess the whole chain:
- Shoulder strength
- Grip strength
- Wrist mobility
- Neck contribution
- Technique (sport/work)
- Load capacity vs demand
Because elbow pain is usually the symptom — not the cause.
Physiotherapy Treatment for Tennis Elbow
1. Pain Reduction Phase
Goal: Calm the tendon without resting it
We use:
- Isometric loading exercises
- Activity modification
- Manual therapy
- Taping support
- Education (this matters most)
You can still use the arm — just in a smarter way.
2. Tendon Strength Phase
This is the most important stage.
We progressively load the tendon:
- Eccentric wrist extension
- Slow heavy resistance training
- Grip strengthening
- Forearm endurance
This actually stimulates tendon healing.
3. Return to Function Phase
Now we retrain real life tasks:
- Lifting mechanics
- Sport technique
- Work tolerance
- Power and speed
Most people skip this — and relapse.

Physiotherapy Treatment for Golfers Elbow Vs Tennis Elbow
Treatment is similar but targets different muscles.
Phase 1 — Calm Pain
- Isometric wrist flexion holds
- Reduce aggressive gripping
- Nerve irritation management (if present)
Phase 2 — Load the Tendon
- Eccentric wrist flexion
- Pronation strengthening
- Grip endurance training
- Shoulder stability work
Phase 3 — Functional Strength
- Pulling exercises
- Carrying tolerance
- Sport-specific drills
Golfer’s elbow often takes slightly longer due to poorer blood supply.
Important: Why Massage & Dry Needling Alone Won’t Fix It
They help pain short-term — but they don’t rebuild tendon strength.
Without loading:
Pain relief = temporary
With loading:
Tissue capacity increases = long term fix
Physiotherapy focuses on the long game.
Real Patient Example (Frenchs Forest Clinic)
We recently saw a 42-year-old dad from Belrose NSW who drove over to our Frenchs Forest clinic.
He developed severe inside elbow pain after:
- Starting gym pull-ups
- Weekend yard work
- Carrying kids
He’d rested it for 4 months — no improvement.
Findings:
- Weak shoulder stability
- Grip endurance poor
- Medial tendon overload (golfer’s elbow)
Treatment plan:
- Isometric holds (week 1)
- Progressive loading (weeks 2–6)
- Gym return plan (weeks 6–10)
Result:
✔ Pain reduced within 2 weeks
✔ Back to gym in 6 weeks
✔ Full pull-ups pain-free in 10 weeks
He said:
“I thought I’d need injections — turns out I just needed the right rehab.”
Do You Need Scans or Injections?
Usually no.
Research shows:
- Ultrasound findings don’t match pain well
- Cortisone helps short term but worse long term
- Exercise rehab outperforms passive treatment
Scans are only needed if:
- Severe trauma
- Locking
- Numbness spreading
- No improvement after rehab
How Long Does Recovery Take?
| Severity | Typical Recovery |
|---|---|
| Mild | 4–6 weeks |
| Moderate | 6–12 weeks |
| Chronic | 3–6 months |
If you’ve had pain >3 months — it’s a tendon conditioning issue.
Prevention Tips (Massively Important)
For Desk Workers
- Raise keyboard height
- Relax mouse grip
- Micro-breaks every 30 minutes
- Strengthen forearms weekly
For Gym
- Don’t over-grip everything
- Progress loads gradually
- Train shoulders not just arms
For Parents
- Carry kids close to body
- Alternate arms
- Avoid prolonged one-hand holding
The Big Takeaway
Both injuries are not inflammatory problems.
They’re:
Load management + strength capacity problems
The fix is progressive rehab — not rest, braces, or injections alone.
FAQs
1. Which is worse — golfers elbow Vs tennis elbow?
Neither is worse, but golfer’s elbow often takes longer to settle due to poorer tendon blood supply.
2. Should I stop gym if I have elbow pain?
No — you should modify it. Complete rest delays healing.
3. Do braces help?
They can reduce pain short term but don’t fix the tendon.
4. Can physio cure chronic elbow pain?
Yes — even long-term cases improve with progressive loading rehab.
5. How do I know if it’s nerve pain instead?
Tingling or numbness into fingers suggests nerve involvement — physio can assess this.
6. Will cortisone injections fix it?
They reduce pain short term but increase recurrence rates long term.
7. Is stretching helpful?
Only mildly. Strengthening matters far more.
8. When should I see a physio?
If pain lasts longer than 2–3 weeks or keeps coming back.
References
- https://www.physio-pedia.com/Lateral_Epicondylitis
- https://www.physio-pedia.com/Medial_Epicondylitis
- https://bjsm.bmj.com/content/50/19/1187
- https://www.jospt.org/doi/10.2519/jospt.2017.7337
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3445129/
Give us a call today on 9806 3077, or book online, just CLICK HERE
https://x-physio.au4.cliniko.com/bookings#service
Thoracic Outlet Syndrome (TOS) is a sneaky cause of shoulder, arm and nerve pain that’s often misdiagnosed or overlooked. The good news? Thoracic outlet syndrome physiotherapy can significantly reduce symptoms by addressing posture, muscle imbalance and nerve compression — without injections or surgery. Let’s break it down.
Why This Shoulder–Arm Pain Might Not Be “Just a Shoulder Problem”
If you’ve got pain, pins and needles, heaviness or weakness running from your neck into your shoulder, arm or hand — and scans keep coming back “normal” — Thoracic Outlet Syndrome could be the missing piece.
TOS happens when nerves or blood vessels are compressed as they pass from the neck to the arm through a narrow space called the thoracic outlet. This compression can irritate sensitive structures, leading to pain that feels confusing, frustrating and persistent.
Many people end up treating the shoulder, elbow or wrist in isolation — without fixing the real cause.
That’s where physiotherapy comes in.

What Is Thoracic Outlet Syndrome?
Thoracic Outlet Syndrome refers to a group of conditions caused by compression of structures passing between the neck and shoulder, including:
- The brachial plexus nerves
- The subclavian artery
- The subclavian vein
This compression usually occurs between the:
- Collarbone (clavicle)
- First rib
- Surrounding muscles (scalenes, pec minor)
When space becomes restricted, symptoms show up fast — especially with poor posture, repetitive work, or overhead activity.

Types of Thoracic Outlet Syndrome
1. Neurogenic TOS (Most Common)
Accounts for around 90% of cases.
Symptoms include:
- Pins and needles in the arm or hand
- Neck and shoulder pain
- Weak grip strength
- Arm fatigue with overhead tasks
2. Venous TOS
Less common but more serious.
Symptoms include:
- Arm swelling
- Heaviness
- Bluish colour changes
3. Arterial TOS
Rare, but significant.
Symptoms include:
- Cold sensitivity
- Arm pain with activity
- Reduced pulse
👉 Physiotherapy is most effective for neurogenic TOS, which is what we see most often in clinic.

Common Causes of Thoracic Outlet Syndrome
TOS doesn’t usually come from one single event. It’s often a slow build-up from daily habits.
Common contributors include:
- Slouched or forward head posture
- Desk work and laptop use
- Repetitive overhead activity
- Heavy backpacks or tool belts
- Poor shoulder blade control
- Previous neck or shoulder injury
- Tight chest or neck muscles
Sound familiar? You’re not alone.

How Thoracic Outlet Syndrome Is Diagnosed
There’s no single scan that “proves” TOS. Diagnosis is mainly clinical, which is where experienced physiotherapy assessment matters.
At our Frenchs Forest clinic, assessment includes:
- Detailed symptom history
- Postural analysis
- Neck, shoulder and thoracic spine movement testing
- Neural tension tests
- Strength and motor control screening
- Functional aggravating positions
This allows us to identify where compression is happening and why.
If your symptoms are different, here is another related blog to read.
How Physiotherapy Helps Thoracic Outlet Syndrome
The goal of thoracic outlet syndrome physiotherapy is simple:
👉 Create more space for nerves and blood vessels by restoring normal movement and posture.
But how we do that is very individual.
1. Postural Re-education (The Game-Changer)
Poor posture is one of the biggest drivers of TOS.
Physiotherapy focuses on:
- Reducing forward head posture
- Improving thoracic spine extension
- Restoring shoulder blade positioning
- Teaching sustainable desk and work posture
Small changes here = big symptom relief.

2. Manual Therapy to Reduce Compression
Hands-on treatment can help reduce tension in structures that narrow the thoracic outlet.
This may include:
- Soft tissue release to scalenes and pec minor
- Thoracic spine mobilisation
- Rib mobility techniques
- Gentle neural glides
This isn’t about cracking — it’s about restoring movement.
3. Strengthening What’s Weak (Not Just Stretching)
Stretching alone isn’t enough.
We target:
- Deep neck flexors
- Lower trapezius
- Serratus anterior
- Rotator cuff stabilisers
These muscles keep your shoulder girdle in the right position during daily tasks.
4. Nerve Mobility (Without Irritation)
When nerves are irritated, they hate being yanked.
Physio-guided nerve mobility exercises:
- Improve nerve tolerance
- Reduce symptoms without flare-ups
- Restore confidence in movement
Done correctly, this is a huge win for people with nerve symptoms.
5. Education & Load Management
We also help you:
- Modify aggravating activities
- Adjust gym or work routines
- Pace recovery safely
- Understand flare-ups (so they don’t freak you out)
Knowledge reduces fear — and fear worsens pain.
A Real Patient Story from Our Frenchs Forest Clinic
Recently, we treated a patient who travelled to our Frenchs Forest NSW clinic from Dee Why, after months of unresolved shoulder and arm pain.
They had:
- Pins and needles into the hand
- Shoulder fatigue when driving
- Neck tightness
- Normal MRI results
They’d tried massage and rest, but symptoms kept returning.
After assessment, we identified neurogenic Thoracic Outlet Syndrome, driven by poor thoracic posture, tight pec minor muscles and weak scapular stabilisers.
Their Treatment Plan Included:
- Manual therapy to neck, ribs and chest
- Thoracic spine mobility work
- Postural correction strategies
- Progressive strengthening
- Nerve mobility exercises
The Result:
Within 6 weeks, their arm symptoms reduced significantly. By 10 weeks, they were driving, working and exercising without flare-ups — and finally understood why the pain was happening.
That’s the power of targeted physiotherapy.
How Long Does Recovery Take?
This varies, but most people see improvement within:
- 3–6 weeks: reduced symptoms and flare-ups
- 6–12 weeks: improved strength, posture and confidence
- 12+ weeks: long-term resolution and prevention
Consistency beats intensity every time.

Can Thoracic Outlet Syndrome Come Back?
Yes — if the underlying drivers aren’t addressed.
That’s why physiotherapy focuses on:
- Long-term posture
- Strength habits
- Movement awareness
- Sustainable exercise routines
Our goal isn’t short-term relief. It’s lasting change.
When to Seek Help
You should consider physiotherapy if you have:
- Ongoing shoulder and arm pain
- Pins and needles without clear cause
- Symptoms worse with posture or overhead work
- Normal scans but ongoing pain
- Failed rest or massage alone
Early treatment = faster recovery.
FAQs – Thoracic Outlet Syndrome Physiotherapy
Is physiotherapy effective for thoracic outlet syndrome?
Yes. Physiotherapy is one of the most effective treatments for neurogenic thoracic outlet syndrome, helping reduce nerve compression, improve posture and restore normal movement without surgery.
How many physio sessions do I need for TOS?
Most people need between 6–12 sessions, depending on symptom severity, posture habits and how long symptoms have been present.
Can thoracic outlet syndrome heal without surgery?
In many cases, yes. Most neurogenic TOS cases respond very well to physiotherapy and exercise-based treatment.
What makes thoracic outlet syndrome worse?
Poor posture, prolonged desk work, overhead activity, stress and weak shoulder stabilisers commonly worsen symptoms.
Do I need imaging for thoracic outlet syndrome?
Imaging is often normal in TOS. Diagnosis is usually based on clinical assessment rather than scans.
References
- https://www.physio-pedia.com/Thoracic_Outlet_Syndrome
- https://www.ncbi.nlm.nih.gov/books/NBK557450/
- https://www.healthdirect.gov.au/thoracic-outlet-syndrome
- https://www.xphysio.com.au/blog/neck-pain-causes-treatment
- https://www.xphysio.com.au/blog/shoulder-pain-physio
Ready to Fix This Properly?
Give us a call today on 9806 3077, or book online, just CLICK HERE
Jumper’s knee (patellar tendinopathy) is a stubborn tendon condition caused by poor load tolerance, not inflammation. The most effective jumper’s knee physiotherapy treatment uses progressive strengthening, smart load management, and movement retraining to reduce pain and get you back to sport — without relying on rest alone.
If Your Knee Pain Keeps Coming Back, This Is Why
You rest it.
It feels better.
You train again.
And the pain comes straight back.
If that sounds familiar, you’re not broken — you’re just treating jumper’s knee the wrong way.
Jumper’s knee (also known as patellar tendinopathy) is one of the most misunderstood knee conditions we see in the clinic. And unfortunately, outdated advice like “just rest it” or “stretch more” keeps people stuck in pain for months… sometimes years.
The good news?
When treated properly, outcomes are excellent.
This blog walks you through:
- What jumper’s knee really is
- Why rest and anti-inflammatories usually fail
- What actually works in jumper’s knee physiotherapy
- How long recovery really takes
- And how we help patients return to sport pain-free
👉 If knee pain is stopping you from training, jumping, running or squatting — keep reading.

What Is Jumper’s Knee (Patellar Tendinopathy)?
Jumper’s knee is a load-related tendon condition affecting the patellar tendon — the strong tendon connecting your kneecap (patella) to your shin bone (tibia).
It’s most common in sports that involve:
- Jumping
- Sprinting
- Sudden changes of direction
- Repeated knee loading
We frequently see jumper’s knee in:
- Basketball
- Volleyball
- Netball
- AFL & soccer
- CrossFit & gym-based training
- Runners (especially hill or speed work)
Despite the name, you don’t have to be a professional athlete. We see plenty of recreational athletes and active adults with patellar tendon pain.
Jumper’s Knee vs Patellar Tendonitis (Why Words Matter)
You’ll often hear the term patellar tendonitis, but this is outdated.
Here’s the key difference:
- Tendonitis = inflammation (short-term)
- Tendinopathy = tendon degeneration + poor load tolerance (long-term)
Most people with jumper’s knee have patellar tendinopathy, not inflammation.
Why this matters:
- ❌ Anti-inflammatories don’t fix the tendon
- ❌ Complete rest weakens it further
- ✅ Progressive loading helps it adapt and heal
This is why modern jumper’s knee physiotherapy focuses on strengthening — not resting forever.
If your pain is more brouadly found around the knee cap, read our blog on Knee Cap Related Pain

Common Symptoms of Jumper’s Knee
Jumper’s knee often starts quietly and worsens over time.
Typical symptoms include:
- Pain just below the kneecap
- Stiffness at the start of training
- Pain during jumping, squatting or running
- Ache after sport or gym sessions
- Reduced power and confidence in the knee
Early on, pain may “warm up” with activity. Later, it can linger, limit performance, and even affect everyday tasks like stairs or getting out of a chair.
Why Rest Alone Doesn’t Work (And Often Makes It Worse)
Short-term load reduction can help settle pain — but complete rest is rarely the answer.
Tendons are load-responsive tissues. They need the right amount of stress to regain strength and capacity.
Think of it like this:
- Too much load → pain flare-ups
- Too little load → weaker tendon
- The right load → adaptation and recovery
Without a structured plan, most people either:
- Push too hard too soon, or
- Rest too much and lose tendon capacity
This is where physiotherapy makes the difference.

Jumper’s Knee Physiotherapy: What Actually Works
1. Thorough Assessment (Not Guesswork)
Effective treatment starts with understanding why your tendon is overloaded.
Your physiotherapist will assess:
- Training volume and recent load spikes
- Jumping and landing mechanics
- Hip, knee and ankle strength
- Quadriceps and calf capacity
- Mobility restrictions
- Recovery habits
This ensures treatment targets the cause, not just the pain.
2. Pain-Modulating Isometric Exercises (Early Phase)
Isometric loading is often used early to:
- Reduce pain
- Maintain strength
- Allow modified training to continue
Common examples include:
- Spanish squats
- Wall sits
- Isometric leg press holds
Pain is carefully monitored and kept within safe limits. This helps calm symptoms without shutting everything down.
3. Progressive Strength Training (The Foundation)
This is the cornerstone of jumper’s knee physiotherapy.
Key principles:
- Slow, controlled loading
- Progressive resistance
- Tendon-specific stress
- Patience (weeks, not days)
Common exercises include:
- Decline squats
- Heavy slow squats
- Split squats
- Step-downs
- Leg press
- Calf strengthening
Strength programs are progressed gradually to rebuild tendon capacity safely.

4. Fixing the Bigger Picture
The tendon is rarely the only issue.
Your physio will also address:
- Poor hip and glute strength
- Limited ankle mobility
- Knee valgus (collapse)
- Poor landing mechanics
- Sudden training load increases
We don’t just treat the tendon — we fix what’s overloading it.
5. Return-to-Sport & Plyometric Training
Once strength improves and pain is under control, jumping and sport-specific drills are reintroduced.
This may include:
- Hopping progressions
- Acceleration and deceleration drills
- Change-of-direction work
- Sport-specific jump patterns
Return to sport is planned, not rushed.
Real Patient Example (Local to Frenchs Forest NSW)
We recently treated a 29-year-old recreational netballer who travelled to our clinic from a surrounding suburb near Frenchs Forest, NSW.
She had over 5 months of patellar tendon pain that worsened with jumping and squatting. Previous advice had been rest, icing, and stretching — none of which worked long-term.
After 12 weeks of structured jumper’s knee physiotherapy focusing on progressive tendon loading, hip strengthening, and controlled return to jumping, she returned to full games pain-free and reported improved confidence and performance on court.
How Long Does Jumper’s Knee Take to Heal?
Recovery time depends on:
- How long symptoms have been present
- Tendon load tolerance
- Consistency with rehab
Typical timelines:
- Mild cases: 6–8 weeks
- Moderate cases: 8–12 weeks
- Long-standing cases: 3–6 months
The key predictor of success? Doing the rehab properly.
Can You Still Train With Jumper’s Knee?
In most cases — yes.
Your physiotherapist will guide:
- What you can continue
- What needs temporary modification
- How to progress safely
Staying active (with the right loads) usually leads to better outcomes than stopping completely.
Why Physiotherapy Is the Best Treatment for Jumper’s Knee
Jumper’s knee physiotherapy provides:
- Evidence-based treatment
- Individualised loading programs
- Movement retraining
- Safer, faster return to sport
- Long-term solutions, not quick fixes
If your knee pain keeps coming back, it’s usually because the tendon hasn’t been rebuilt properly — yet.
Ready to Fix Your Jumper’s Knee?
If knee pain is stopping you from training, jumping or playing sport, don’t just rest and hope.
Proper physiotherapy works.
👉 Give us a call today on 9806 3077, or book online, just CLICK HERE
Frequently Asked Questions (FAQs)
Is jumper’s knee permanent?
No. With proper physiotherapy and progressive loading, most people make a full recovery.
Should I stop all sport with jumper’s knee?
Not always. Many people can continue modified training under physio guidance.
Are scans necessary for jumper’s knee?
Imaging isn’t always required. Diagnosis is usually clinical.
Do knee straps or braces help?
They may reduce symptoms short-term but don’t fix the underlying problem.
Is surgery required for patellar tendinopathy?
Surgery is rarely needed and only considered after failed conservative treatment.
References
-
Cook JL, Purdam CR. Is tendon pathology a continuum? British Journal of Sports Medicine
https://bjsm.bmj.com/content/43/6/409 -
Malliaras P, Barton CJ, Reeves ND, Langberg H. Achilles and patellar tendinopathy loading programmes. Sports Medicine
https://link.springer.com/article/10.1007/s40279-013-0019-z -
Physiopedia – Patellar Tendinopathy
https://www.physio-pedia.com/Patellar_Tendinopathy -
Sports Medicine Australia – Tendon Injuries
https://sma.org.au/resources-advice/injury-fact-sheets/tendon-injuries/ -
Australian Institute of Sport – Tendon Load Management
https://www.ais.gov.au/position_statements/best_practice_content/tendon_load_management
Tendon pain can stop you training, working, or even sleeping comfortably. But is it tendonitis or tendinopathy? While they sound similar, they’re actually different conditions that need different treatment approaches. In this blog, we’ll break down the key differences, common causes, and how tendonitis physiotherapy vs tendinopathy rehab can get you back to pain-free movement faster.
If you’ve been resting for weeks with no improvement — keep reading. The right physio plan can change everything.
Why Tendon Pain Is So Common
Tendons are the tough, rope-like tissues that connect muscle to bone. They handle enormous loads every day — running, lifting, typing, throwing, or even standing for long periods.
When tendons are overloaded or under-prepared for the work we demand of them, pain can develop. This is especially common in:
- Runners
- Tradies
- Desk workers with repetitive strain
- Parents lifting kids
- Weekend warriors returning to sport too quickly
Historically, any tendon pain was labelled “tendonitis.” But modern research shows most long-lasting tendon pain isn’t inflammation at all — it’s tendinopathy. And that distinction matters.

Tendonitis vs Tendinopathy: What’s the Actual Difference?
What is Tendonitis?
Tendonitis refers to acute inflammation of a tendon.
It usually happens:
- After a sudden spike in activity
- Following direct trauma
- In the early stage of overload
Classic tendonitis signs include:
- Sudden onset pain
- Swelling or warmth
- Pain with movement
- Tenderness to touch
This inflammatory phase is usually short-lived — lasting days to a couple of weeks.
What is Tendinopathy?
Tendinopathy refers to degenerative tendon change, not inflammation.
With repeated overload and inadequate recovery, the tendon structure starts to weaken. Collagen fibres become disorganised, and the tendon thickens but loses strength.
Typical features include:
- Pain that develops gradually
- Stiffness in the morning
- Pain at the start of activity that eases as you warm up
- Pain returning after exercise
- Long-term persistence (months)
This is why rest and anti-inflammatory medication often fail — because there’s little inflammation to treat.
Why Getting the Diagnosis Right Matters
If you treat tendinopathy like tendonitis — meaning rest, ice, and avoiding load — the tendon actually becomes weaker over time.
If you overload an inflamed acute tendon — you can worsen irritation.
That’s why a proper physiotherapy assessment is essential. We look at:
- Your pain history
- Activity levels
- Strength and movement patterns
- Load tolerance of the tendon
- Contributing biomechanical factors
From there, we tailor treatment to match the tendon’s stage of healing.
Common Tendon Problems We See
At our clinic near Frenchs Forest NSW, we commonly treat:
- Achilles tendinopathy
- Patellar tendinopathy (jumper’s knee)
- Rotator cuff tendinopathy
- Tennis and golfer’s elbow
- Gluteal tendinopathy
- Plantar fascia tendon pain
Each tendon behaves differently — so cookie-cutter rehab doesn’t work.
What Causes Tendonitis and Tendinopathy?
While the conditions differ, risk factors often overlap:
- Sudden increase in training or workload
- Poor strength or conditioning
- Repetitive movements
- Poor technique or biomechanics
- Inadequate recovery
- Age-related tendon changes
- Previous injury history
The good news? These are all modifiable with the right physiotherapy program.

Tendonitis Physiotherapy vs Tendinopathy Rehab: What Physio Does Best
Early Tendonitis Treatment
If your tendon is in the acute inflammatory stage, physiotherapy focuses on:
- Load reduction guidance (not total rest)
- Activity modification
- Gentle mobility exercises
- Soft tissue techniques
- Taping or bracing if required
- Gradual re-loading plan
The goal is to settle pain while keeping the tendon healthy enough to recover properly.
Tendinopathy Rehabilitation
For chronic tendon pain, exercise is medicine — but it must be the right exercise at the right load.
Physiotherapy for tendinopathy typically includes:
- Progressive strength loading
- Isometric pain-reducing exercises
- Slow resistance training
- Plyometric or sport-specific loading later
- Gait or technique correction
- Hip and core strengthening
- Return-to-sport planning
This stimulates tendon remodelling — helping fibres realign and regain strength.

Why Rest Alone Doesn’t Fix Tendinopathy
One of the biggest myths is “just rest until it settles.”
Yes, rest might reduce symptoms temporarily. But without loading, tendons:
- Lose stiffness
- Lose strength
- Become more sensitive to load
- Are more likely to flare again
Physio-guided loading teaches your tendon to tolerate stress again — safely and progressively.
A Real Patient Example from Our Clinic
Recently, we saw Sarah, a 38-year-old runner from Beacon Hill, just minutes from Frenchs Forest NSW. She’d been struggling with Achilles pain for over six months. She’d tried resting, changing shoes, and even stopped running — but the pain returned every time she resumed training.
After assessment, we diagnosed mid-portion Achilles tendinopathy. Her rehab plan included:
- Isometric calf loading for pain control
- Progressive slow calf raises
- Hip and glute strength work
- Running load modification
- Gradual return-to-run plan
Within four weeks, Sarah was running short distances pain-free. At three months, she returned to her usual running routine — stronger than before.
That’s the power of evidence-based tendon rehab.
How Long Does Tendon Rehab Take?
This depends on:
- How long you’ve had pain
- The tendon involved
- Your current strength levels
- Your consistency with exercises
General timeframes:
- Acute tendonitis: 2–6 weeks
- Tendinopathy: 8–16 weeks (sometimes longer)
The key is steady progress, not rushing.
Can Physio Help Prevent Tendon Injuries?
Absolutely. Prevention programs focus on:
- Strength and conditioning
- Load management education
- Movement pattern correction
- Warm-up routines
- Recovery strategies
Prevention is always easier than rehab.
When Should You See a Physio?
Book in if:
- Tendon pain lasts longer than 2 weeks
- Pain returns every time you resume activity
- Morning stiffness is increasing
- You’re unsure how much load is safe
- Rest hasn’t worked
Early guidance prevents long-term frustration.
Why Choose Physiotherapy for Tendon Pain?
At our Frenchs Forest clinic, we offer:
- Thorough assessment
- Individualised rehab plans
- Evidence-based loading programs
- Hands-on treatment when required
- Clear guidance on activity modification
- Ongoing progression to full recovery
No generic exercise sheets — just tailored care.
Final Thoughts
Tendonitis physiotherapy vs tendinopathy rehab are not the same — and treating them correctly makes all the difference. Whether your tendon pain is new or has been lingering for months, there’s a proven pathway forward.
Don’t wait for it to “just settle.”
FAQs
What is the main difference between tendonitis and tendinopathy?
Tendonitis is short-term inflammation of a tendon, usually after sudden overload. Tendinopathy is long-term degeneration of the tendon structure caused by repeated strain. They need different treatment approaches.
Should I rest or exercise with tendon pain?
Short-term rest helps acute tendonitis. But tendinopathy requires progressive loading exercises to rebuild tendon strength. A physiotherapist can guide the correct balance.
How long does tendinopathy take to heal?
Most tendinopathy programs take 8–16 weeks of consistent rehab. Long-standing cases may take longer, but steady improvement is expected with proper loading.
Can anti-inflammatory medication fix tendinopathy?
Anti-inflammatories may reduce pain temporarily, but tendinopathy isn’t primarily inflammatory. Rehab exercises remain the main treatment.
When should I see a physiotherapist for tendon pain?
If pain lasts more than two weeks, keeps returning with activity, or limits daily life, it’s time for a physio assessment.
References (with websites)
Here are useful, authoritative sites to learn more:
- Better Health Channel – Tendinopathy & tendon pain
https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/tendonitis - Healthdirect – Tendinopathy info (Australia)
https://www.healthdirect.gov.au/tendinopathy - Healthdirect – Tendinitis info (Australia)
https://www.healthdirect.gov.au/tendinitis - Physiocheck – Achilles tendinopathy overview
https://www.physiocheck.com.au/condition/68/achilles-tendinopathy - Physica – Achilles tendinopathy & continuum model
https://www.physica.com.au/achilles-tendonopathy/ - Peak Physio – Tendinopathy research references
https://www.peak-physio.com.au/education/tendinopathy-overview/ - Blog XPhysio
- https://xphysio.com.au/blog/
Give us a call today on 9806 3077, or book online — just CLICK HERE:
https://x-physio.au4.cliniko.com/bookings#service
A hip flexor strain can cause sharp groin or hip pain, stiffness and difficulty walking, running or standing upright. Hip flexor strain physiotherapy helps reduce pain, restore mobility and rebuild strength — while addressing the underlying causes so the injury doesn’t keep coming back. Keep reading for expert physio tips and real recovery stories.
Got a sore hip that just won’t loosen up?
You’re not alone.
Hip flexor strains are one of those injuries that sneak up on you — especially if you’re a runner, sit most of the day, or are getting a little stiffer with age. One day you’re fine, the next you’re struggling to lift your leg, stand up straight, or get through your usual walk or jog without pain.
The good news?
With the right hip flexor strain physiotherapy, most people recover well — without scans, injections or long-term issues.
Let’s break down what’s really going on, how physio helps, and what recovery actually looks like in the real world.

What is a hip flexor strain?
Your hip flexors are a group of muscles at the front of your hip that help lift your knee and bend your hip. The main ones include:
- Iliopsoas (iliacus + psoas major)
- Rectus femoris (part of the quadriceps)
- Sartorius
A hip flexor strain occurs when one or more of these muscles is overstretched or overloaded, leading to small muscle tears and inflammation.
Common signs and symptoms
Hip flexor strains don’t always feel dramatic at first. Common symptoms include:
- Pain at the front of the hip or deep in the groin
- Pain when lifting the knee or walking uphill
- Tightness or pulling when standing up straight
- Reduced stride length when walking or running
- Weakness when climbing stairs
- Pain after sitting for long periods
In more severe cases, you may notice bruising, swelling or a sharp pain during activity.

Who is most at risk?
Hip flexor strains are particularly common in:
🏃 Runners
- Sudden increases in mileage or speed
- Sprinting or hill training
- Poor hip strength or overstriding
🪑 People who sit a lot
- Office workers
- Drivers
- Students
Long periods of sitting shorten the hip flexors, making them vulnerable when you suddenly ask them to work.
👵 Seniors
- Reduced hip strength
- Stiffer joints
- Changes in walking mechanics
Age-related muscle weakness and balance changes increase strain on the hip flexors during everyday movements.

What actually causes a hip flexor strain?
While it often feels like it “came out of nowhere”, there’s usually more going on under the surface.
Common contributors include:
- Tight hip flexors from prolonged sitting
- Weak glutes and core muscles
- Poor running or walking mechanics
- Reduced hip joint mobility
- Sudden spikes in activity
- Inadequate warm-up or recovery
This is why rest alone rarely fixes the problem long-term.
Why rest and stretching alone often isn’t enough
Many people try to self-manage a hip flexor strain by:
- Resting completely
- Stretching aggressively
- Using heat or massage
While these can help symptoms temporarily, they don’t address why the strain happened in the first place.
Without proper rehabilitation:
- Pain often returns when activity resumes
- Mobility remains limited
- Compensations develop in the lower back or knee
- The injury becomes chronic
This is where hip flexor strain physiotherapy makes a big difference.

How physiotherapy helps a hip flexor strain
Physiotherapy isn’t just about easing pain — it’s about restoring confident movement and preventing recurrence.
1. Accurate diagnosis
Not all front-of-hip pain is a hip flexor strain.
Your physiotherapist will rule out:
- Hip joint arthritis
- Labral issues
- Stress reactions
- Lumbar spine referral
- Sports hernia-type injuries
Getting the diagnosis right is critical for recovery.
2. Pain relief and early management
In the early phase, physio helps calm symptoms using:
- Hands-on soft tissue techniques
- Gentle joint mobilisation
- Load modification advice
- Activity guidance (what to avoid vs what to keep doing)
This reduces pain without completely shutting you down.
3. Restoring hip mobility
Stiff hips place extra strain on the hip flexors.
Physiotherapy focuses on improving:
- Hip extension range
- Pelvic control
- Lumbar–hip coordination
This helps you move more freely and efficiently again.
4. Strengthening the right muscles
One of the biggest mistakes is only stretching the hip flexors.
Your rehab will also target:
- Glutes (especially glute max and med)
- Deep core muscles
- Hip stabilisers
- Controlled hip flexor loading (progressively)
This allows the muscle to heal stronger, not just looser.

5. Movement retraining
Whether you’re running, walking or standing up from a chair, your physio will look at how you move.
This may include:
- Gait retraining
- Running drills
- Posture and desk advice
- Gradual return-to-activity planning
A real patient story from our clinic
Recently, we saw Mark, a 47-year-old recreational runner who travelled to our clinic from Belrose, just a few minutes from Frenchs Forest NSW.
Mark developed a nagging front-of-hip pain that worsened during his morning runs and made sitting at work uncomfortable. Rest helped temporarily, but every attempt to return to running brought the pain straight back.
What we found
- Tight iliopsoas and rectus femoris
- Weak glutes and poor hip extension during running
- Reduced pelvic control when fatigued
His physiotherapy program included
- Manual therapy to reduce hip flexor tone
- Progressive hip and glute strengthening
- Running retraining to reduce overstriding
- Gradual return-to-run plan
The outcome
Within 6 weeks, Mark:
- Returned to pain-free running
- Could sit comfortably all day
- Improved his stride efficiency
- Reported feeling “stronger than before the injury”
Most importantly, he avoided repeated flare-ups.
How long does recovery take?
Recovery depends on severity and consistency with rehab:
- Mild strains: 2–4 weeks
- Moderate strains: 4–8 weeks
- Chronic or recurrent strains: 8–12+ weeks
Early physiotherapy almost always shortens recovery time.
Can you keep exercising with a hip flexor strain?
In most cases — yes, but with guidance.
Your physio will help you:
- Modify training loads
- Maintain fitness safely
- Avoid movements that delay healing
Complete rest is rarely necessary and often slows recovery.
V

Why early physio matters
Delaying treatment increases the risk of:
- Chronic hip pain
- Compensation into the lower back
- Reduced walking or running tolerance
- Repeated strains
Early hip flexor strain physiotherapy means faster recovery and better long-term results.
When should you see a physio?
Book in if you:
- Have hip pain lasting more than 7–10 days
- Feel pain when lifting your leg or walking
- Keep re-injuring the same area
- Sit a lot and feel tight or sore through the hips
- Want to return to running or exercise safely
Hip flexor pain doesn’t have to slow you down or become “one of those things you live with”.
With the right physiotherapy plan, you can move freely again — and stay that way.
FAQs – Hip Flexor Strain Physiotherapy
What is the fastest way to heal a hip flexor strain?
Early physiotherapy, load management, targeted strengthening and gradual return to activity are the most effective ways to heal a hip flexor strain quickly and safely.
Should I stretch a hip flexor strain?
Gentle stretching may help, but aggressive stretching too early can delay healing. A physiotherapist will guide the right timing and intensity.
Can a hip flexor strain cause lower back pain?
Yes. Tight or weak hip flexors can alter pelvic position and increase load on the lower back.
Is walking good for a hip flexor strain?
Usually yes, provided it doesn’t increase pain. Walking is often encouraged with modifications early on.
How do I know if my hip pain is a strain or something else?
Hip pain can come from the joint, spine or surrounding structures. A physiotherapist can assess and diagnose the cause accurately.
References
- Sports Medicine Australia – Hip Flexor Injuries
- https://sma.org.au/resources/injury-fact-sheets/hip-flexor-strain/
- Physiopedia – Hip Flexor Strain
- https://www.physio-pedia.com/Hip_Flexor_Strain
- Better Health Victoria – Muscle Strains
- https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/muscle-strain
- Related blog: Why Sitting All Day Wrecks Your Hips (And What Physio Can Do)
- https://www.healthline.com/health/tight-hips
- Related blog: Running Injuries – When to See a Physio
- https://www.sportsphysio.org.au/blog/common-running-injuries-and-how-physio-can-help/
- Related Blog: Hip Labral Tears
- https://xphysio.com.au/hip-labral-tear-physiotherapy-guide/
Ready to move without hip pain?
Give us a call today on 9806 3077, or book online, just CLICK HERE:
👉 https://x-physio.au4.cliniko.com/bookings#service
