Thoracic Outlet Syndrome (TOS) is a sneaky cause of shoulder, arm and nerve pain that’s often misdiagnosed or overlooked. The good news? Thoracic outlet syndrome physiotherapy can significantly reduce symptoms by addressing posture, muscle imbalance and nerve compression — without injections or surgery. Let’s break it down.
Why This Shoulder–Arm Pain Might Not Be “Just a Shoulder Problem”
If you’ve got pain, pins and needles, heaviness or weakness running from your neck into your shoulder, arm or hand — and scans keep coming back “normal” — Thoracic Outlet Syndrome could be the missing piece.
TOS happens when nerves or blood vessels are compressed as they pass from the neck to the arm through a narrow space called the thoracic outlet. This compression can irritate sensitive structures, leading to pain that feels confusing, frustrating and persistent.
Many people end up treating the shoulder, elbow or wrist in isolation — without fixing the real cause.
That’s where physiotherapy comes in.

What Is Thoracic Outlet Syndrome?
Thoracic Outlet Syndrome refers to a group of conditions caused by compression of structures passing between the neck and shoulder, including:
- The brachial plexus nerves
- The subclavian artery
- The subclavian vein
This compression usually occurs between the:
- Collarbone (clavicle)
- First rib
- Surrounding muscles (scalenes, pec minor)
When space becomes restricted, symptoms show up fast — especially with poor posture, repetitive work, or overhead activity.

Types of Thoracic Outlet Syndrome
1. Neurogenic TOS (Most Common)
Accounts for around 90% of cases.
Symptoms include:
- Pins and needles in the arm or hand
- Neck and shoulder pain
- Weak grip strength
- Arm fatigue with overhead tasks
2. Venous TOS
Less common but more serious.
Symptoms include:
- Arm swelling
- Heaviness
- Bluish colour changes
3. Arterial TOS
Rare, but significant.
Symptoms include:
- Cold sensitivity
- Arm pain with activity
- Reduced pulse
👉 Physiotherapy is most effective for neurogenic TOS, which is what we see most often in clinic.

Common Causes of Thoracic Outlet Syndrome
TOS doesn’t usually come from one single event. It’s often a slow build-up from daily habits.
Common contributors include:
- Slouched or forward head posture
- Desk work and laptop use
- Repetitive overhead activity
- Heavy backpacks or tool belts
- Poor shoulder blade control
- Previous neck or shoulder injury
- Tight chest or neck muscles
Sound familiar? You’re not alone.

How Thoracic Outlet Syndrome Is Diagnosed
There’s no single scan that “proves” TOS. Diagnosis is mainly clinical, which is where experienced physiotherapy assessment matters.
At our Frenchs Forest clinic, assessment includes:
- Detailed symptom history
- Postural analysis
- Neck, shoulder and thoracic spine movement testing
- Neural tension tests
- Strength and motor control screening
- Functional aggravating positions
This allows us to identify where compression is happening and why.
If your symptoms are different, here is another related blog to read.
How Physiotherapy Helps Thoracic Outlet Syndrome
The goal of thoracic outlet syndrome physiotherapy is simple:
👉 Create more space for nerves and blood vessels by restoring normal movement and posture.
But how we do that is very individual.
1. Postural Re-education (The Game-Changer)
Poor posture is one of the biggest drivers of TOS.
Physiotherapy focuses on:
- Reducing forward head posture
- Improving thoracic spine extension
- Restoring shoulder blade positioning
- Teaching sustainable desk and work posture
Small changes here = big symptom relief.

2. Manual Therapy to Reduce Compression
Hands-on treatment can help reduce tension in structures that narrow the thoracic outlet.
This may include:
- Soft tissue release to scalenes and pec minor
- Thoracic spine mobilisation
- Rib mobility techniques
- Gentle neural glides
This isn’t about cracking — it’s about restoring movement.
3. Strengthening What’s Weak (Not Just Stretching)
Stretching alone isn’t enough.
We target:
- Deep neck flexors
- Lower trapezius
- Serratus anterior
- Rotator cuff stabilisers
These muscles keep your shoulder girdle in the right position during daily tasks.
4. Nerve Mobility (Without Irritation)
When nerves are irritated, they hate being yanked.
Physio-guided nerve mobility exercises:
- Improve nerve tolerance
- Reduce symptoms without flare-ups
- Restore confidence in movement
Done correctly, this is a huge win for people with nerve symptoms.
5. Education & Load Management
We also help you:
- Modify aggravating activities
- Adjust gym or work routines
- Pace recovery safely
- Understand flare-ups (so they don’t freak you out)
Knowledge reduces fear — and fear worsens pain.
A Real Patient Story from Our Frenchs Forest Clinic
Recently, we treated a patient who travelled to our Frenchs Forest NSW clinic from Dee Why, after months of unresolved shoulder and arm pain.
They had:
- Pins and needles into the hand
- Shoulder fatigue when driving
- Neck tightness
- Normal MRI results
They’d tried massage and rest, but symptoms kept returning.
After assessment, we identified neurogenic Thoracic Outlet Syndrome, driven by poor thoracic posture, tight pec minor muscles and weak scapular stabilisers.
Their Treatment Plan Included:
- Manual therapy to neck, ribs and chest
- Thoracic spine mobility work
- Postural correction strategies
- Progressive strengthening
- Nerve mobility exercises
The Result:
Within 6 weeks, their arm symptoms reduced significantly. By 10 weeks, they were driving, working and exercising without flare-ups — and finally understood why the pain was happening.
That’s the power of targeted physiotherapy.
How Long Does Recovery Take?
This varies, but most people see improvement within:
- 3–6 weeks: reduced symptoms and flare-ups
- 6–12 weeks: improved strength, posture and confidence
- 12+ weeks: long-term resolution and prevention
Consistency beats intensity every time.

Can Thoracic Outlet Syndrome Come Back?
Yes — if the underlying drivers aren’t addressed.
That’s why physiotherapy focuses on:
- Long-term posture
- Strength habits
- Movement awareness
- Sustainable exercise routines
Our goal isn’t short-term relief. It’s lasting change.
When to Seek Help
You should consider physiotherapy if you have:
- Ongoing shoulder and arm pain
- Pins and needles without clear cause
- Symptoms worse with posture or overhead work
- Normal scans but ongoing pain
- Failed rest or massage alone
Early treatment = faster recovery.
FAQs – Thoracic Outlet Syndrome Physiotherapy
Is physiotherapy effective for thoracic outlet syndrome?
Yes. Physiotherapy is one of the most effective treatments for neurogenic thoracic outlet syndrome, helping reduce nerve compression, improve posture and restore normal movement without surgery.
How many physio sessions do I need for TOS?
Most people need between 6–12 sessions, depending on symptom severity, posture habits and how long symptoms have been present.
Can thoracic outlet syndrome heal without surgery?
In many cases, yes. Most neurogenic TOS cases respond very well to physiotherapy and exercise-based treatment.
What makes thoracic outlet syndrome worse?
Poor posture, prolonged desk work, overhead activity, stress and weak shoulder stabilisers commonly worsen symptoms.
Do I need imaging for thoracic outlet syndrome?
Imaging is often normal in TOS. Diagnosis is usually based on clinical assessment rather than scans.
References
- https://www.physio-pedia.com/Thoracic_Outlet_Syndrome
- https://www.ncbi.nlm.nih.gov/books/NBK557450/
- https://www.healthdirect.gov.au/thoracic-outlet-syndrome
- https://www.xphysio.com.au/blog/neck-pain-causes-treatment
- https://www.xphysio.com.au/blog/shoulder-pain-physio
Ready to Fix This Properly?
Give us a call today on 9806 3077, or book online, just CLICK HERE
Jumper’s knee (patellar tendinopathy) is a stubborn tendon condition caused by poor load tolerance, not inflammation. The most effective jumper’s knee physiotherapy treatment uses progressive strengthening, smart load management, and movement retraining to reduce pain and get you back to sport — without relying on rest alone.
If Your Knee Pain Keeps Coming Back, This Is Why
You rest it.
It feels better.
You train again.
And the pain comes straight back.
If that sounds familiar, you’re not broken — you’re just treating jumper’s knee the wrong way.
Jumper’s knee (also known as patellar tendinopathy) is one of the most misunderstood knee conditions we see in the clinic. And unfortunately, outdated advice like “just rest it” or “stretch more” keeps people stuck in pain for months… sometimes years.
The good news?
When treated properly, outcomes are excellent.
This blog walks you through:
- What jumper’s knee really is
- Why rest and anti-inflammatories usually fail
- What actually works in jumper’s knee physiotherapy
- How long recovery really takes
- And how we help patients return to sport pain-free
👉 If knee pain is stopping you from training, jumping, running or squatting — keep reading.

What Is Jumper’s Knee (Patellar Tendinopathy)?
Jumper’s knee is a load-related tendon condition affecting the patellar tendon — the strong tendon connecting your kneecap (patella) to your shin bone (tibia).
It’s most common in sports that involve:
- Jumping
- Sprinting
- Sudden changes of direction
- Repeated knee loading
We frequently see jumper’s knee in:
- Basketball
- Volleyball
- Netball
- AFL & soccer
- CrossFit & gym-based training
- Runners (especially hill or speed work)
Despite the name, you don’t have to be a professional athlete. We see plenty of recreational athletes and active adults with patellar tendon pain.
Jumper’s Knee vs Patellar Tendonitis (Why Words Matter)
You’ll often hear the term patellar tendonitis, but this is outdated.
Here’s the key difference:
- Tendonitis = inflammation (short-term)
- Tendinopathy = tendon degeneration + poor load tolerance (long-term)
Most people with jumper’s knee have patellar tendinopathy, not inflammation.
Why this matters:
- ❌ Anti-inflammatories don’t fix the tendon
- ❌ Complete rest weakens it further
- ✅ Progressive loading helps it adapt and heal
This is why modern jumper’s knee physiotherapy focuses on strengthening — not resting forever.
If your pain is more brouadly found around the knee cap, read our blog on Knee Cap Related Pain

Common Symptoms of Jumper’s Knee
Jumper’s knee often starts quietly and worsens over time.
Typical symptoms include:
- Pain just below the kneecap
- Stiffness at the start of training
- Pain during jumping, squatting or running
- Ache after sport or gym sessions
- Reduced power and confidence in the knee
Early on, pain may “warm up” with activity. Later, it can linger, limit performance, and even affect everyday tasks like stairs or getting out of a chair.
Why Rest Alone Doesn’t Work (And Often Makes It Worse)
Short-term load reduction can help settle pain — but complete rest is rarely the answer.
Tendons are load-responsive tissues. They need the right amount of stress to regain strength and capacity.
Think of it like this:
- Too much load → pain flare-ups
- Too little load → weaker tendon
- The right load → adaptation and recovery
Without a structured plan, most people either:
- Push too hard too soon, or
- Rest too much and lose tendon capacity
This is where physiotherapy makes the difference.

Jumper’s Knee Physiotherapy: What Actually Works
1. Thorough Assessment (Not Guesswork)
Effective treatment starts with understanding why your tendon is overloaded.
Your physiotherapist will assess:
- Training volume and recent load spikes
- Jumping and landing mechanics
- Hip, knee and ankle strength
- Quadriceps and calf capacity
- Mobility restrictions
- Recovery habits
This ensures treatment targets the cause, not just the pain.
2. Pain-Modulating Isometric Exercises (Early Phase)
Isometric loading is often used early to:
- Reduce pain
- Maintain strength
- Allow modified training to continue
Common examples include:
- Spanish squats
- Wall sits
- Isometric leg press holds
Pain is carefully monitored and kept within safe limits. This helps calm symptoms without shutting everything down.
3. Progressive Strength Training (The Foundation)
This is the cornerstone of jumper’s knee physiotherapy.
Key principles:
- Slow, controlled loading
- Progressive resistance
- Tendon-specific stress
- Patience (weeks, not days)
Common exercises include:
- Decline squats
- Heavy slow squats
- Split squats
- Step-downs
- Leg press
- Calf strengthening
Strength programs are progressed gradually to rebuild tendon capacity safely.

4. Fixing the Bigger Picture
The tendon is rarely the only issue.
Your physio will also address:
- Poor hip and glute strength
- Limited ankle mobility
- Knee valgus (collapse)
- Poor landing mechanics
- Sudden training load increases
We don’t just treat the tendon — we fix what’s overloading it.
5. Return-to-Sport & Plyometric Training
Once strength improves and pain is under control, jumping and sport-specific drills are reintroduced.
This may include:
- Hopping progressions
- Acceleration and deceleration drills
- Change-of-direction work
- Sport-specific jump patterns
Return to sport is planned, not rushed.
Real Patient Example (Local to Frenchs Forest NSW)
We recently treated a 29-year-old recreational netballer who travelled to our clinic from a surrounding suburb near Frenchs Forest, NSW.
She had over 5 months of patellar tendon pain that worsened with jumping and squatting. Previous advice had been rest, icing, and stretching — none of which worked long-term.
After 12 weeks of structured jumper’s knee physiotherapy focusing on progressive tendon loading, hip strengthening, and controlled return to jumping, she returned to full games pain-free and reported improved confidence and performance on court.
How Long Does Jumper’s Knee Take to Heal?
Recovery time depends on:
- How long symptoms have been present
- Tendon load tolerance
- Consistency with rehab
Typical timelines:
- Mild cases: 6–8 weeks
- Moderate cases: 8–12 weeks
- Long-standing cases: 3–6 months
The key predictor of success? Doing the rehab properly.
Can You Still Train With Jumper’s Knee?
In most cases — yes.
Your physiotherapist will guide:
- What you can continue
- What needs temporary modification
- How to progress safely
Staying active (with the right loads) usually leads to better outcomes than stopping completely.
Why Physiotherapy Is the Best Treatment for Jumper’s Knee
Jumper’s knee physiotherapy provides:
- Evidence-based treatment
- Individualised loading programs
- Movement retraining
- Safer, faster return to sport
- Long-term solutions, not quick fixes
If your knee pain keeps coming back, it’s usually because the tendon hasn’t been rebuilt properly — yet.
Ready to Fix Your Jumper’s Knee?
If knee pain is stopping you from training, jumping or playing sport, don’t just rest and hope.
Proper physiotherapy works.
👉 Give us a call today on 9806 3077, or book online, just CLICK HERE
Frequently Asked Questions (FAQs)
Is jumper’s knee permanent?
No. With proper physiotherapy and progressive loading, most people make a full recovery.
Should I stop all sport with jumper’s knee?
Not always. Many people can continue modified training under physio guidance.
Are scans necessary for jumper’s knee?
Imaging isn’t always required. Diagnosis is usually clinical.
Do knee straps or braces help?
They may reduce symptoms short-term but don’t fix the underlying problem.
Is surgery required for patellar tendinopathy?
Surgery is rarely needed and only considered after failed conservative treatment.
References
-
Cook JL, Purdam CR. Is tendon pathology a continuum? British Journal of Sports Medicine
https://bjsm.bmj.com/content/43/6/409 -
Malliaras P, Barton CJ, Reeves ND, Langberg H. Achilles and patellar tendinopathy loading programmes. Sports Medicine
https://link.springer.com/article/10.1007/s40279-013-0019-z -
Physiopedia – Patellar Tendinopathy
https://www.physio-pedia.com/Patellar_Tendinopathy -
Sports Medicine Australia – Tendon Injuries
https://sma.org.au/resources-advice/injury-fact-sheets/tendon-injuries/ -
Australian Institute of Sport – Tendon Load Management
https://www.ais.gov.au/position_statements/best_practice_content/tendon_load_management
Tendon pain can stop you training, working, or even sleeping comfortably. But is it tendonitis or tendinopathy? While they sound similar, they’re actually different conditions that need different treatment approaches. In this blog, we’ll break down the key differences, common causes, and how tendonitis physiotherapy vs tendinopathy rehab can get you back to pain-free movement faster.
If you’ve been resting for weeks with no improvement — keep reading. The right physio plan can change everything.
Why Tendon Pain Is So Common
Tendons are the tough, rope-like tissues that connect muscle to bone. They handle enormous loads every day — running, lifting, typing, throwing, or even standing for long periods.
When tendons are overloaded or under-prepared for the work we demand of them, pain can develop. This is especially common in:
- Runners
- Tradies
- Desk workers with repetitive strain
- Parents lifting kids
- Weekend warriors returning to sport too quickly
Historically, any tendon pain was labelled “tendonitis.” But modern research shows most long-lasting tendon pain isn’t inflammation at all — it’s tendinopathy. And that distinction matters.

Tendonitis vs Tendinopathy: What’s the Actual Difference?
What is Tendonitis?
Tendonitis refers to acute inflammation of a tendon.
It usually happens:
- After a sudden spike in activity
- Following direct trauma
- In the early stage of overload
Classic tendonitis signs include:
- Sudden onset pain
- Swelling or warmth
- Pain with movement
- Tenderness to touch
This inflammatory phase is usually short-lived — lasting days to a couple of weeks.
What is Tendinopathy?
Tendinopathy refers to degenerative tendon change, not inflammation.
With repeated overload and inadequate recovery, the tendon structure starts to weaken. Collagen fibres become disorganised, and the tendon thickens but loses strength.
Typical features include:
- Pain that develops gradually
- Stiffness in the morning
- Pain at the start of activity that eases as you warm up
- Pain returning after exercise
- Long-term persistence (months)
This is why rest and anti-inflammatory medication often fail — because there’s little inflammation to treat.
Why Getting the Diagnosis Right Matters
If you treat tendinopathy like tendonitis — meaning rest, ice, and avoiding load — the tendon actually becomes weaker over time.
If you overload an inflamed acute tendon — you can worsen irritation.
That’s why a proper physiotherapy assessment is essential. We look at:
- Your pain history
- Activity levels
- Strength and movement patterns
- Load tolerance of the tendon
- Contributing biomechanical factors
From there, we tailor treatment to match the tendon’s stage of healing.
Common Tendon Problems We See
At our clinic near Frenchs Forest NSW, we commonly treat:
- Achilles tendinopathy
- Patellar tendinopathy (jumper’s knee)
- Rotator cuff tendinopathy
- Tennis and golfer’s elbow
- Gluteal tendinopathy
- Plantar fascia tendon pain
Each tendon behaves differently — so cookie-cutter rehab doesn’t work.
What Causes Tendonitis and Tendinopathy?
While the conditions differ, risk factors often overlap:
- Sudden increase in training or workload
- Poor strength or conditioning
- Repetitive movements
- Poor technique or biomechanics
- Inadequate recovery
- Age-related tendon changes
- Previous injury history
The good news? These are all modifiable with the right physiotherapy program.

Tendonitis Physiotherapy vs Tendinopathy Rehab: What Physio Does Best
Early Tendonitis Treatment
If your tendon is in the acute inflammatory stage, physiotherapy focuses on:
- Load reduction guidance (not total rest)
- Activity modification
- Gentle mobility exercises
- Soft tissue techniques
- Taping or bracing if required
- Gradual re-loading plan
The goal is to settle pain while keeping the tendon healthy enough to recover properly.
Tendinopathy Rehabilitation
For chronic tendon pain, exercise is medicine — but it must be the right exercise at the right load.
Physiotherapy for tendinopathy typically includes:
- Progressive strength loading
- Isometric pain-reducing exercises
- Slow resistance training
- Plyometric or sport-specific loading later
- Gait or technique correction
- Hip and core strengthening
- Return-to-sport planning
This stimulates tendon remodelling — helping fibres realign and regain strength.

Why Rest Alone Doesn’t Fix Tendinopathy
One of the biggest myths is “just rest until it settles.”
Yes, rest might reduce symptoms temporarily. But without loading, tendons:
- Lose stiffness
- Lose strength
- Become more sensitive to load
- Are more likely to flare again
Physio-guided loading teaches your tendon to tolerate stress again — safely and progressively.
A Real Patient Example from Our Clinic
Recently, we saw Sarah, a 38-year-old runner from Beacon Hill, just minutes from Frenchs Forest NSW. She’d been struggling with Achilles pain for over six months. She’d tried resting, changing shoes, and even stopped running — but the pain returned every time she resumed training.
After assessment, we diagnosed mid-portion Achilles tendinopathy. Her rehab plan included:
- Isometric calf loading for pain control
- Progressive slow calf raises
- Hip and glute strength work
- Running load modification
- Gradual return-to-run plan
Within four weeks, Sarah was running short distances pain-free. At three months, she returned to her usual running routine — stronger than before.
That’s the power of evidence-based tendon rehab.
How Long Does Tendon Rehab Take?
This depends on:
- How long you’ve had pain
- The tendon involved
- Your current strength levels
- Your consistency with exercises
General timeframes:
- Acute tendonitis: 2–6 weeks
- Tendinopathy: 8–16 weeks (sometimes longer)
The key is steady progress, not rushing.
Can Physio Help Prevent Tendon Injuries?
Absolutely. Prevention programs focus on:
- Strength and conditioning
- Load management education
- Movement pattern correction
- Warm-up routines
- Recovery strategies
Prevention is always easier than rehab.
When Should You See a Physio?
Book in if:
- Tendon pain lasts longer than 2 weeks
- Pain returns every time you resume activity
- Morning stiffness is increasing
- You’re unsure how much load is safe
- Rest hasn’t worked
Early guidance prevents long-term frustration.
Why Choose Physiotherapy for Tendon Pain?
At our Frenchs Forest clinic, we offer:
- Thorough assessment
- Individualised rehab plans
- Evidence-based loading programs
- Hands-on treatment when required
- Clear guidance on activity modification
- Ongoing progression to full recovery
No generic exercise sheets — just tailored care.
Final Thoughts
Tendonitis physiotherapy vs tendinopathy rehab are not the same — and treating them correctly makes all the difference. Whether your tendon pain is new or has been lingering for months, there’s a proven pathway forward.
Don’t wait for it to “just settle.”
FAQs
What is the main difference between tendonitis and tendinopathy?
Tendonitis is short-term inflammation of a tendon, usually after sudden overload. Tendinopathy is long-term degeneration of the tendon structure caused by repeated strain. They need different treatment approaches.
Should I rest or exercise with tendon pain?
Short-term rest helps acute tendonitis. But tendinopathy requires progressive loading exercises to rebuild tendon strength. A physiotherapist can guide the correct balance.
How long does tendinopathy take to heal?
Most tendinopathy programs take 8–16 weeks of consistent rehab. Long-standing cases may take longer, but steady improvement is expected with proper loading.
Can anti-inflammatory medication fix tendinopathy?
Anti-inflammatories may reduce pain temporarily, but tendinopathy isn’t primarily inflammatory. Rehab exercises remain the main treatment.
When should I see a physiotherapist for tendon pain?
If pain lasts more than two weeks, keeps returning with activity, or limits daily life, it’s time for a physio assessment.
References (with websites)
Here are useful, authoritative sites to learn more:
- Better Health Channel – Tendinopathy & tendon pain
https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/tendonitis - Healthdirect – Tendinopathy info (Australia)
https://www.healthdirect.gov.au/tendinopathy - Healthdirect – Tendinitis info (Australia)
https://www.healthdirect.gov.au/tendinitis - Physiocheck – Achilles tendinopathy overview
https://www.physiocheck.com.au/condition/68/achilles-tendinopathy - Physica – Achilles tendinopathy & continuum model
https://www.physica.com.au/achilles-tendonopathy/ - Peak Physio – Tendinopathy research references
https://www.peak-physio.com.au/education/tendinopathy-overview/ - Blog XPhysio
- https://xphysio.com.au/blog/
Give us a call today on 9806 3077, or book online — just CLICK HERE:
https://x-physio.au4.cliniko.com/bookings#service
A hip flexor strain can cause sharp groin or hip pain, stiffness and difficulty walking, running or standing upright. Hip flexor strain physiotherapy helps reduce pain, restore mobility and rebuild strength — while addressing the underlying causes so the injury doesn’t keep coming back. Keep reading for expert physio tips and real recovery stories.
Got a sore hip that just won’t loosen up?
You’re not alone.
Hip flexor strains are one of those injuries that sneak up on you — especially if you’re a runner, sit most of the day, or are getting a little stiffer with age. One day you’re fine, the next you’re struggling to lift your leg, stand up straight, or get through your usual walk or jog without pain.
The good news?
With the right hip flexor strain physiotherapy, most people recover well — without scans, injections or long-term issues.
Let’s break down what’s really going on, how physio helps, and what recovery actually looks like in the real world.

What is a hip flexor strain?
Your hip flexors are a group of muscles at the front of your hip that help lift your knee and bend your hip. The main ones include:
- Iliopsoas (iliacus + psoas major)
- Rectus femoris (part of the quadriceps)
- Sartorius
A hip flexor strain occurs when one or more of these muscles is overstretched or overloaded, leading to small muscle tears and inflammation.
Common signs and symptoms
Hip flexor strains don’t always feel dramatic at first. Common symptoms include:
- Pain at the front of the hip or deep in the groin
- Pain when lifting the knee or walking uphill
- Tightness or pulling when standing up straight
- Reduced stride length when walking or running
- Weakness when climbing stairs
- Pain after sitting for long periods
In more severe cases, you may notice bruising, swelling or a sharp pain during activity.

Who is most at risk?
Hip flexor strains are particularly common in:
🏃 Runners
- Sudden increases in mileage or speed
- Sprinting or hill training
- Poor hip strength or overstriding
🪑 People who sit a lot
- Office workers
- Drivers
- Students
Long periods of sitting shorten the hip flexors, making them vulnerable when you suddenly ask them to work.
👵 Seniors
- Reduced hip strength
- Stiffer joints
- Changes in walking mechanics
Age-related muscle weakness and balance changes increase strain on the hip flexors during everyday movements.

What actually causes a hip flexor strain?
While it often feels like it “came out of nowhere”, there’s usually more going on under the surface.
Common contributors include:
- Tight hip flexors from prolonged sitting
- Weak glutes and core muscles
- Poor running or walking mechanics
- Reduced hip joint mobility
- Sudden spikes in activity
- Inadequate warm-up or recovery
This is why rest alone rarely fixes the problem long-term.
Why rest and stretching alone often isn’t enough
Many people try to self-manage a hip flexor strain by:
- Resting completely
- Stretching aggressively
- Using heat or massage
While these can help symptoms temporarily, they don’t address why the strain happened in the first place.
Without proper rehabilitation:
- Pain often returns when activity resumes
- Mobility remains limited
- Compensations develop in the lower back or knee
- The injury becomes chronic
This is where hip flexor strain physiotherapy makes a big difference.

How physiotherapy helps a hip flexor strain
Physiotherapy isn’t just about easing pain — it’s about restoring confident movement and preventing recurrence.
1. Accurate diagnosis
Not all front-of-hip pain is a hip flexor strain.
Your physiotherapist will rule out:
- Hip joint arthritis
- Labral issues
- Stress reactions
- Lumbar spine referral
- Sports hernia-type injuries
Getting the diagnosis right is critical for recovery.
2. Pain relief and early management
In the early phase, physio helps calm symptoms using:
- Hands-on soft tissue techniques
- Gentle joint mobilisation
- Load modification advice
- Activity guidance (what to avoid vs what to keep doing)
This reduces pain without completely shutting you down.
3. Restoring hip mobility
Stiff hips place extra strain on the hip flexors.
Physiotherapy focuses on improving:
- Hip extension range
- Pelvic control
- Lumbar–hip coordination
This helps you move more freely and efficiently again.
4. Strengthening the right muscles
One of the biggest mistakes is only stretching the hip flexors.
Your rehab will also target:
- Glutes (especially glute max and med)
- Deep core muscles
- Hip stabilisers
- Controlled hip flexor loading (progressively)
This allows the muscle to heal stronger, not just looser.

5. Movement retraining
Whether you’re running, walking or standing up from a chair, your physio will look at how you move.
This may include:
- Gait retraining
- Running drills
- Posture and desk advice
- Gradual return-to-activity planning
A real patient story from our clinic
Recently, we saw Mark, a 47-year-old recreational runner who travelled to our clinic from Belrose, just a few minutes from Frenchs Forest NSW.
Mark developed a nagging front-of-hip pain that worsened during his morning runs and made sitting at work uncomfortable. Rest helped temporarily, but every attempt to return to running brought the pain straight back.
What we found
- Tight iliopsoas and rectus femoris
- Weak glutes and poor hip extension during running
- Reduced pelvic control when fatigued
His physiotherapy program included
- Manual therapy to reduce hip flexor tone
- Progressive hip and glute strengthening
- Running retraining to reduce overstriding
- Gradual return-to-run plan
The outcome
Within 6 weeks, Mark:
- Returned to pain-free running
- Could sit comfortably all day
- Improved his stride efficiency
- Reported feeling “stronger than before the injury”
Most importantly, he avoided repeated flare-ups.
How long does recovery take?
Recovery depends on severity and consistency with rehab:
- Mild strains: 2–4 weeks
- Moderate strains: 4–8 weeks
- Chronic or recurrent strains: 8–12+ weeks
Early physiotherapy almost always shortens recovery time.
Can you keep exercising with a hip flexor strain?
In most cases — yes, but with guidance.
Your physio will help you:
- Modify training loads
- Maintain fitness safely
- Avoid movements that delay healing
Complete rest is rarely necessary and often slows recovery.
V

Why early physio matters
Delaying treatment increases the risk of:
- Chronic hip pain
- Compensation into the lower back
- Reduced walking or running tolerance
- Repeated strains
Early hip flexor strain physiotherapy means faster recovery and better long-term results.
When should you see a physio?
Book in if you:
- Have hip pain lasting more than 7–10 days
- Feel pain when lifting your leg or walking
- Keep re-injuring the same area
- Sit a lot and feel tight or sore through the hips
- Want to return to running or exercise safely
Hip flexor pain doesn’t have to slow you down or become “one of those things you live with”.
With the right physiotherapy plan, you can move freely again — and stay that way.
FAQs – Hip Flexor Strain Physiotherapy
What is the fastest way to heal a hip flexor strain?
Early physiotherapy, load management, targeted strengthening and gradual return to activity are the most effective ways to heal a hip flexor strain quickly and safely.
Should I stretch a hip flexor strain?
Gentle stretching may help, but aggressive stretching too early can delay healing. A physiotherapist will guide the right timing and intensity.
Can a hip flexor strain cause lower back pain?
Yes. Tight or weak hip flexors can alter pelvic position and increase load on the lower back.
Is walking good for a hip flexor strain?
Usually yes, provided it doesn’t increase pain. Walking is often encouraged with modifications early on.
How do I know if my hip pain is a strain or something else?
Hip pain can come from the joint, spine or surrounding structures. A physiotherapist can assess and diagnose the cause accurately.
References
- Sports Medicine Australia – Hip Flexor Injuries
- https://sma.org.au/resources/injury-fact-sheets/hip-flexor-strain/
- Physiopedia – Hip Flexor Strain
- https://www.physio-pedia.com/Hip_Flexor_Strain
- Better Health Victoria – Muscle Strains
- https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/muscle-strain
- Related blog: Why Sitting All Day Wrecks Your Hips (And What Physio Can Do)
- https://www.healthline.com/health/tight-hips
- Related blog: Running Injuries – When to See a Physio
- https://www.sportsphysio.org.au/blog/common-running-injuries-and-how-physio-can-help/
- Related Blog: Hip Labral Tears
- https://xphysio.com.au/hip-labral-tear-physiotherapy-guide/
Ready to move without hip pain?
Give us a call today on 9806 3077, or book online, just CLICK HERE:
👉 https://x-physio.au4.cliniko.com/bookings#service
SI joint pain can be sneaky — it often feels like lower back, hip or even groin pain, and many people don’t realise where it’s really coming from. The good news? Physiotherapy can accurately diagnose the problem and provide targeted treatment to relieve pain and restore movement. Keep reading to learn what causes SI joint pain, how it’s diagnosed, and what actually works to fix it — or book in now and start feeling better sooner.
What is the SI Joint?
The sacroiliac (SI) joints sit at the base of your spine, where the sacrum meets the pelvis. You have one on each side. These joints don’t move a lot, but they play a huge role in transferring force between your upper body and legs — especially when walking, running, bending and lifting.
When the SI joint becomes irritated, stiff, or unstable, it can produce significant pain. Because of its location, SI joint pain is frequently mistaken for:
- Lower back pain
- Hip joint pain
- Sciatica
- Gluteal muscle strain
- Disc-related back pain
This is why an accurate assessment matters — and why physiotherapy is so effective.

Common Causes of SI Joint Pain
SI joint pain rarely appears out of nowhere. It usually develops due to one or more contributing factors.
1. Joint irritation or inflammation
Repetitive loading, prolonged sitting, poor posture or sudden increases in activity can irritate the joint surfaces.
2. Muscle imbalances
Weak glute muscles, poor core control, or tight hip flexors can overload the SI joint over time.
3. Pregnancy and post-partum changes
Hormonal changes increase ligament laxity, which can make the SI joint less stable.
4. Trauma or falls
A direct impact to the pelvis or awkward twisting injury can trigger SI joint dysfunction.
5. Asymmetrical movement patterns
Leg length differences, scoliosis or habitual uneven weight-bearing can place extra stress through one SI joint.
6. Degenerative changes
Age-related joint wear can reduce shock absorption and irritate surrounding structures.
Understanding the root cause is essential — treating SI joint pain is not just about “loosening the back.”

Symptoms of SI Joint Pain
People with SI joint pain often report:
- Deep ache on one side of the lower back or buttock
- Pain when getting out of a chair or car
- Discomfort when walking uphill or climbing stairs
- Pain turning in bed
- Stiffness after sitting too long
- Occasional referral into the groin or upper thigh
Unlike disc-related pain, SI joint pain rarely causes pins and needles or numbness below the knee.

Why Self-Diagnosis Often Fails
Because SI joint pain mimics other conditions, many people:
- Stretch the wrong muscles
- Rest too long
- Blame their mattress
- Or assume it’s “just getting older”
Unfortunately, generic stretching or random strengthening can sometimes make symptoms worse.
A physiotherapy assessment uses specific clinical tests to confirm whether the SI joint is actually the source of pain — and rule out other structures.
How Physiotherapists Diagnose SI Joint Pain
At X-Physio in Frenchs Forest, assessment typically includes:
- Detailed history of symptoms and triggers
- Postural and movement analysis
- Hip, lumbar spine and pelvic mobility testing
- Muscle strength testing
- Special SI joint provocation tests
- Walking and functional movement assessment
This allows us to:
✔ Confirm whether the SI joint is the pain generator
✔ Identify contributing muscle imbalances
✔ Detect movement habits keeping the problem going
✔ Build a plan based on your lifestyle and goals
No guesswork. No generic programs.

How Physiotherapy Treats SI Joint Pain
1. Pain relief and joint calming
Early treatment focuses on settling irritation through:
- Gentle joint mobilisation
- Soft tissue release for tight glutes, hip flexors and lower back
- Activity modification guidance
- Taping or bracing where appropriate
This helps reduce pain so you can move more comfortably again.
2. Restoring normal movement
Once pain settles, we address:
- Hip stiffness
- Lumbar spine mobility
- Pelvic control during walking and bending
Improving how your body moves reduces strain through the SI joint long-term.
3. Strengthening key support muscles
SI joints rely heavily on muscular support. We target:
- Glute strength
- Deep core control
- Hip stabilisers
- Lower limb alignment
You’ll receive a tailored home exercise program with clear guidance — not a generic printout.
4. Fixing contributing habits
We also look at:
- Sitting posture
- Lifting technique
- Sleeping positions
- Workstation setup
- Training errors for runners and gym-goers
Small changes here make a big difference.
5. Gradual return to full activity
Whether your goal is:
- Getting back to sport
- Playing with your kids
- Sitting comfortably at work
- Or walking without pain
Your rehab plan progresses step-by-step until you’re confident and pain-free again.

A Real Patient Example
Recently, we saw a patient who came to our clinic from Dee Why, a surrounding suburb near Frenchs Forest NSW. They’d been struggling with persistent one-sided lower back and buttock pain for over four months. Sitting at work and getting out of the car were especially painful. They’d tried massage and general stretching with only short-term relief.
Our assessment confirmed SI joint irritation combined with weak glute muscles and poor pelvic control during walking.
Treatment included:
- Gentle SI joint mobilisation
- Targeted glute and core strengthening
- Hip mobility work
- Advice on desk sitting and car posture
Within two weeks, their pain had significantly reduced. By week six, they were back to full gym training and long coastal walks without flare-ups.
Most importantly — they understood how to prevent it returning.
Why Choose Physiotherapy for SI Joint Pain?
Medication may reduce pain temporarily. Rest may help briefly. But without fixing the underlying movement and strength issues, SI joint pain often returns.
Physiotherapy offers:
✔ Accurate diagnosis
✔ Targeted treatment
✔ Long-term prevention
✔ Reduced reliance on medication
✔ Faster return to normal life
How Long Does Recovery Take?
Every case differs, but most people notice:
- Early pain reduction in 1–2 weeks
- Improved movement by 3–4 weeks
- Full functional recovery in 6–8 weeks
Chronic or long-standing cases may take longer — but still improve with the right plan.
Can SI Joint Pain Be Prevented?
Yes. Key strategies include:
- Maintaining good glute and core strength
- Avoiding prolonged slouched sitting
- Gradually increasing training loads
- Keeping hips mobile
- Seeking early treatment when pain first appears
Prevention is far easier than treating a long-standing problem.

FAQs: SI Joint Pain and Physiotherapy
What is the fastest way to relieve SI joint pain?
The fastest relief comes from accurate diagnosis followed by manual therapy to calm the joint, combined with specific strengthening exercises to stabilise the pelvis. Rest alone usually doesn’t fix the underlying cause.
Can SI joint pain go away on its own?
Mild irritation sometimes settles, but if contributing movement or strength issues remain, pain often returns. Physiotherapy helps resolve both symptoms and root causes.
Is walking good or bad for SI joint pain?
Gentle walking is usually helpful, but long distances or hills may aggravate symptoms early on. A physiotherapist will guide safe activity levels.
How do I know if my pain is SI joint or disc-related?
SI joint pain is typically one-sided, deep in the buttock and worsens with position changes. Disc pain often produces leg symptoms like pins and needles. A physio assessment confirms the source.
Do I need scans for SI joint pain?
Imaging is rarely needed. Clinical assessment is usually enough to diagnose SI joint dysfunction accurately.
Can exercise make SI joint pain worse?
Incorrect or unsupervised exercises can aggravate symptoms. Targeted physiotherapy exercises are designed to stabilise — not overload — the joint.
References & Further Reading
- https://xphysio.com.au/blog/
- https://xphysio.com.au/blog/tension-headache-physio
- https://xphysio.com.au/blog/groin-strain-recovery-time
- https://www.physio-pedia.com/Sacroiliac_Joint
- https://www.spine-health.com/conditions/sacroiliac-joint-dysfunction
- https://www.sportsmedicine.com.au/si-joint-pain
Ready to Get Relief?
If SI joint pain is limiting your work, training or daily life, don’t wait for it to become chronic. The sooner you address it, the faster you’ll recover.
Give us a call today on 9806 3077, or book online — just CLICK HERE:
https://x-physio.au4.cliniko.com/bookings#service
Golfers elbow can turn simple tasks like gripping a coffee cup or lifting weights into a painful chore. The good news? The right golfers elbow treatment with targeted physiotherapy exercises can reduce pain fast and restore strength. In this guide, you’ll learn exactly what works — and how we help patients get better quickly. Ready to fix it? Let’s go.
What Is Golfers Elbow?
Despite the name, you don’t have to play golf to get golfers elbow. Medically known as medial epicondylalgia, golfers elbow is an overuse injury affecting the tendons on the inside of your elbow. These tendons connect your forearm muscles to the bony bump on the inside of the elbow and are responsible for gripping, wrist flexion, and forearm rotation.
When these tendons are overloaded repeatedly — through work, sport, or daily activities — tiny micro-tears develop. Over time, the tendon becomes painful, weak, and sensitive to load.
Common activities that trigger golfers elbow include:
- Golf, tennis, and racquet sports
- Weight training (especially gripping and pulling)
- Manual labour and tool use
- Repetitive typing or mouse work
- DIY or gardening
If left untreated, symptoms can linger for months — which is why early physiotherapy treatment is key.

Symptoms of Golfers Elbow Treatment
Typical symptoms include:
- Pain or tenderness on the inside of the elbow
- Weak grip strength
- Pain when lifting, gripping, or twisting objects
- Stiffness in the elbow or forearm
- Symptoms worsening with activity
Many people ignore early signs, hoping it will “just settle.” Unfortunately, tendon injuries rarely improve without the right loading program.
Why Physiotherapy Is the Best Golfers Elbow Treatment
The old advice for golfers elbow treatmentwas rest, anti-inflammatories, and waiting it out. We now know that progressive tendon loading is the most effective long-term solution.
At X Physio in Frenchs Forest, our golfers elbow treatment focuses on:
- Reducing pain and irritation
- Restoring tendon strength
- Improving grip and forearm capacity
- Correcting contributing movement patterns
- Returning you safely to sport or work
Physiotherapy doesn’t just mask symptoms — it addresses the cause. Physiotherapists are the best allied health professionals for Golfers Elbow Treatment.

Common Causes We See in Clinic
Every case is slightly different, but the most common contributing factors include:
- Sudden increase in activity or training load
- Poor lifting or sporting technique
- Weak forearm and shoulder muscles
- Prolonged gripping postures (desk work, tools)
- Lack of recovery time
Identifying the real driver of your pain is crucial — which is why assessment matters before Golfers Elbow Treatment.

A Real Patient Example from Our Clinic
Recently, we saw James (name changed for privacy), a 42-year-old electrician from Forestville, a surrounding suburb of Frenchs Forest. He had been dealing with inner elbow pain for nearly four months. Every time he used tools at work or lifted weights at the gym, the pain flared up. Rest helped temporarily, but symptoms always returned.
After assessment, we found:
- Reduced grip strength
- High tendon sensitivity
- Poor load tolerance in wrist flexor muscles
- Shoulder weakness contributing to overload at the elbow
James began a structured golfers elbow physiotherapy program:
- Pain-modulating isometric exercises
- Progressive wrist and grip strengthening
- Shoulder and scapular strengthening
- Manual therapy for symptom relief
- Load management guidance for work tasks
Within 3 weeks, his daily pain reduced significantly. By 6 weeks, he returned to full work duties and gym training with minimal discomfort — and now continues maintenance exercises to prevent recurrence.
This is a typical outcome when treatment is started early and progressed correctly.
Golfers Elbow Treatment That Reduce Pain Fast
Below are the key exercise stages we commonly prescribe. Always get individual assessment before starting, as load levels matter.
1. Isometric Wrist Flexor Holds (Early Pain Relief)
These help calm tendon pain without irritating it.
How to do it:
- Rest your forearm on a table, palm facing up
- Hold a light dumbbell or resistance band
- Gently lift your wrist slightly
- Hold for 30–45 seconds
- Repeat 4–5 times
This often reduces pain immediately by calming the nervous system response around the tendon.
2. Slow Wrist Flexion Strengthening
Once pain settles, we build true tendon capacity.
- Forearm supported, palm up
- Hold a light dumbbell
- Slowly lift the wrist up for 3 seconds
- Lower back down for 3 seconds
- 3 sets of 12–15 reps
Progress weight gradually over weeks.

3. Forearm Pronation & Supination
- Elbow at 90 degrees
- Hold a hammer or dumbbell vertically
- Rotate palm up → palm down slowly
- 3 sets of 10–12 reps
This strengthens rotational control — essential for gripping and tool use.
4. Grip Strength Training
- Use a soft stress ball or grip trainer
- Squeeze and hold for 5 seconds
- Repeat 15–20 reps
Improves functional load tolerance.
5. Shoulder & Scapular Strengthening
Weak shoulders shift excessive load to the elbow. Common exercises include:
- Resistance band rows
- External rotation strengthening
- Scapular control drills
A strong shoulder reduces recurrence risk.

How Long Does Recovery Take?
With proper golfers elbow treatment:
- Mild cases: 2–4 weeks
- Moderate cases: 6–8 weeks
- Long-standing cases: 8–12 weeks
Consistency with exercises is the biggest predictor of success for Golfers Elbow Treatment.
Should You Rest Completely?
Total rest is rarely helpful. Tendons need appropriate loading to heal. We guide you on:
- Which activities to temporarily reduce
- How to modify work or sport
- How to progress safely
This prevents flare-ups while still promoting healing.
Other Treatment Options We May Use
Alongside exercise therapy, physiotherapy may include:
- Hands-on soft tissue techniques
- Taping or bracing advice
- Ergonomic or sporting technique assessment
- Education on load management
In persistent cases, we may liaise with your GP regarding imaging or further options — but most people improve without injections or surgery.

Why Choose X Physio in Frenchs Forest?
- One-on-one personalised treatment
- Evidence-based tendon rehabilitation
- Clear progression plans
- Easy online booking
- Convenient for Frenchs Forest and surrounding suburbs
We don’t just treat pain — we build long-term resilience.
Frequently Asked Questions
Is golfers elbow the same as tennis elbow?
No. Tennis elbow affects the outside of the elbow. Golfers elbow affects the inside. Both involve tendon overload but require slightly different rehab exercises.
Can golfers elbow heal on its own?
Sometimes mild cases settle, but most persistent cases need structured loading exercises. Without treatment, symptoms often return when activity increases again.
Are anti-inflammatory tablets helpful?
They may reduce short-term pain but don’t fix tendon weakness. Physiotherapy addresses the underlying cause.
Can I keep training while recovering?
Yes — with modifications. We guide you on safe load levels so you stay active without delaying healing.
Do I need a scan for golfers elbow?
Not usually. Diagnosis is clinical. Imaging is only needed if progress stalls or symptoms are unusual.
References & Helpful Resources
- References & Helpful Resources
- Better Health Channel – Tendon Injuries
https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/tendonitis - Sports Medicine Australia – Overuse Injuries
https://sma.org.au/resources-advice/injury-fact-sheets/overuse-injuries/ - Physiopedia – Medial Epicondylalgia (Golfers Elbow)
https://www.physio-pedia.com/Medial_Epicondylalgia - Healthdirect Australia – Tennis & Golfer’s Elbow
https://www.healthdirect.gov.au/tennis-elbow-and-golfers-elbow - X Physio Blog – Tennis Elbow Treatment Guide
https://xphysio.com.au/blog/tennis-elbow-treatment - X Physio Blog – Shoulder Strength & Injury Prevention
https://xphysio.com.au/blog/shoulder-strength-exercises - X Physio Blog – How Tendons Heal With Exercise
https://xphysio.com.au/blog/tendon-rehabilitation-exercises
If inner elbow pain is limiting your work, training, or daily life, don’t wait for it to worsen. The right golfers elbow treatment can get you better faster.
Give us a call today on 9806 3077, or book online, just CLICK HERE:
https://x-physio.au4.cliniko.com/bookings#service
Tension headaches are often neck problems disguised as head pain. Tight neck muscles, poor posture, stress, and desk work can irritate nerves and tissues that refer pain into the head. The good news? With the right tension headache physio, most people experience fast relief and long-term change. Let’s dive into why it happens—and how physio fixes it.
The Real Reason Neck Muscles Cause Headaches
Most people assume headaches come from dehydration, stress, or eye strain. While those can contribute, one of the biggest drivers of tension headaches is actually the muscles and joints in your neck.
When the muscles around the neck, shoulders, and base of the skull tighten up, they place pressure on surrounding nerves and blood vessels. This “muscle guarding” often builds slowly over time due to:
- Working at a desk
- Looking down at your phone
- Driving long distances
- Stress bracing through the shoulders
- Grinding your teeth
- Poor sleep positions
Those tensioned muscles attach into the skull and refer pain upward. That’s why tension headaches often feel like:
- A band of pressure around the head
- Pain behind the eyes
- Heavy or tight feeling at the back of the head
- Pain that worsens as the day goes on
- Aching into the temples
It’s not “just a headache”—it’s usually your body waving a big flag saying, “Sort this neck out!”

The Science Behind Tension Headaches
There’s a strong link between neck dysfunction and headaches. Studies have shown that the upper cervical spine (C1–C3) has direct nerve connections to the head and face. When these joints get stiff and the surrounding muscles tighten, they irritate the nerves that also supply the head.
That’s why tension headache physio are classed as a type of cervicogenic headache in many cases.
Common muscle culprits include:
- Upper trapezius
- Levator scapulae
- Sternocleidomastoid (front neck muscle)
- Suboccipital muscles at the base of skull
When these muscles get overloaded, they trigger pain patterns that wrap around the skull. Physio helps by restoring movement, reducing tension, and retraining your posture so it doesn’t keep happening.

Why Simply Taking Painkillers Doesn’t Fix It
Panadol and Nurofen might help temporarily, but they don’t solve the root cause. The muscle tension and joint restriction remains. That’s why so many people experience:
- Headaches returning daily or weekly
- Needing stronger medication
- Relying on “just pushing through”
Physio treats the source, not just the symptoms.

How Tension Headache Physio Helps
A tension headache physio assessment looks far beyond just your head pain. We assess:
- Neck mobility
- Muscle tightness
- Shoulder blade control
- Posture
- Breathing patterns
- Lifestyle triggers
Then we create a tailored plan.
Tension Headache Physio may include:
✔️ Hands-on soft tissue release
✔️ Mobilisation of the cervical spine
✔️ Dry needling (if suitable)
✔️ Posture correction
✔️ Strengthening weak muscles
✔️ Relaxation and breathing strategies
✔️ Ergonomic education

Real Patient Example – Relief Closer Than You Think
Recently we treated a patient from Brookvale, just a short drive from our Frenchs Forest clinic. She had been suffering with daily tension headaches for months. By midday she’d feel tightness creep up from her neck into her temples and behind her eyes. She needed a Tension Headache Physio.
She had tried:
- Massage
- Painkillers
- New pillows
- More coffee (of course…)
Nothing gave more than temporary relief.
During her physio assessment, we found:
- Very tight suboccipital muscles
- Forward head posture
- Limited upper neck movement
- Overactive shoulder muscles trying to “help” support the head
We worked through a structured treatment plan involving cervical joint mobilisation, targeted release, posture retraining, and simple home exercises.
Within two weeks, her headaches reduced from daily to only occasional. Within six weeks, she reported weeks with zero headaches, improved concentration, better sleep, and no longer relying on medication.
She said her only regret was not coming sooner.
Are Your Headaches Actually Coming From Your Neck?
Here are signs your headache is likely neck-related:
- Pain starts in the neck and travels to your head
- Headache worsens with sitting or working at a computer
- Movement makes it worse
- You feel neck tightness or stiffness
- Pain is on one side more than the other
- You get relief when someone massages your neck
If that sounds like you, physio is extremely likely to help.
Common Triggers You May Not Realise
Even “little habits” add up:
- Sitting with your head forward
- Clenching your jaw
- Sleeping on too many pillows
- Slouching
- Not moving enough during the day
- Stress tension
The good news? These are fixable.
Can Exercises Help Tension Headaches?
Absolutely. Targeted exercises help retrain your muscles to support your neck properly. But not just any exercises. The internet is full of generic stretches that may not address what your body needs.
Physio-guided exercises ensure you strengthen the right muscles without flaring things up.
Lifestyle Tips To Reduce Tension Headaches
💡 Move every 30–60 minutes
💡 Keep screens at eye level
💡 Relax your shoulders (if they’re up near your ears right now… drop them)
💡 Stay hydrated
💡 Stretch gently instead of cracking your neck
💡 Sleep well and support your neck properly
Small changes = huge impact.

Why Choose Us For Tension Headache Physio in Frenchs Forest NSW?
We see tension headache patients every single week. Our approach is:
- Thorough
- Individualised
- Evidence-based
- Focused on long-term solutions
We don’t just treat the pain — we treat the reason it keeps happening.
If you’re tired of tension headaches controlling your day, affecting your mood, productivity, sleep, and enjoyment of life, it may be time to fix it properly.
👉 Book an appointment and let’s get your head clearer, your neck happier, and your life back on track.
FAQs – Tension Headache Physio
What is a tension headache?
A tension headache is a headache caused by tight muscles and restricted joints in the neck and shoulders, leading to referred pain into the head.
Can physio really help headaches?
Yes. If your headaches are coming from your neck, physiotherapy is one of the most effective treatments.
How many sessions will I need?
Most people notice improvement within 2–3 sessions, with long-term change often achieved within 4–8 sessions depending on severity.
What if I’ve had headaches for years?
It’s still worth getting assessed. Chronic headaches often have multiple contributing factors and physio can significantly reduce frequency and intensity.
Do I need a referral?
No referral needed unless you’re claiming under a specific program like EPC.
Do you treat kids and teens?
Yes, particularly students dealing with posture-related headaches.
References
https://www.headacheaustralia.org.au/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4996711/
https://www.physioaustralia.org.au/
https://xphysio.com.au/headaches-that-can-be-treated-by-a-physiotherapist/
https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD001878.pub3/full
Ready to finally do something about your headaches?
Give us a call today on 9806 3077, or book online, just CLICK HERE: https://x-physio.au4.cliniko.com/bookings#service
Groin Strain Recovery Time can be quite lengthy. Have you pulled your groin and wondering how long it’ll take to heal? Groin strains can be painful, frustrating and slow you down — especially if you love sport, running or gym training. The good news? With the right physiotherapy, you can recover faster, reduce re-injury risk and get back to moving confidently again. Let’s explain how.
What Exactly Is a Groin Strain?
A groin strain happens when the inner thigh muscles — usually the adductor group — are overstretched or torn. These muscles help stabilise your hip, pull the leg inward and support quick changes of direction. That’s why they’re so important for footballers, runners, gym-goers, hockey players, sprinters and weekend warriors.
Groin strains often happen with:
- Sudden sprinting
- Quick twisting or pivoting
- Lunging or kicking
- Slipping or overstretching
- Heavy gym work without proper warm-up
Many people try to “walk it off” — but if not treated properly, Groin Strain Recovery Time’s can go on for weeks or even months.

Groin Strain Recovery Time – What’s Normal?
Recovery time depends on the severity of the injury, how early you treat it, and whether you rehab it properly.
Grade 1 Groin Strain
Mild overstretching with small muscle fibre damage. You may feel discomfort but can still walk fairly normally.
Grade 1 Groin Strain Recovery Time 1–3 weeks
Grade 2 Groin Strain
Partial tear, moderate pain, weakness, reduced movement and difficulty walking fast, running or changing direction.
Grade 2 Groin Strain Recovery Time: 3–6 weeks
Grade 3 Groin Strain
Significant or complete muscle tear. Severe pain, major swelling/bruising and difficulty weight bearing.
Grade 3 Groin Strain Recovery Time: 8–12+ weeks (sometimes requires specialist input)
These are general timelines — but physiotherapy can significantly speed up recovery, reduce pain faster and make sure the groin heals strong, not weak.

Why Do Some Groin Strain Recovery Times blow out?
Many Groin Strain Recovery Time’s drag on longer than they should for a few key reasons:
- People rest too long — and lose strength
- They return to sport too early
- They don’t rebuild muscle control properly
- Scar tissue forms without proper movement
- They never address weakness or flexibility issues
So instead of healing strong, the groin stays vulnerable — leading to repeated strains.
This is exactly where physiotherapy makes a massive difference.
How Physiotherapy Speeds Up Groin Strain Recovery Time
At X-Physio, we don’t just “treat the pain”. We identify why the injury happened, help it heal properly and make you stronger than before.
When you come in, we assess:
- Which muscles are injured
- Whether it’s a strain or something else (hernia, hip pathology, nerve pain or tendon issues can mimic groin pain)
- Your strength and movement
- Walking and running mechanics
- Sport or activity demands
Then we tailor treatment to your exact situation.
Phase 1 – Settling Pain and Protecting the Injury
Early management is all about calming things down without completely resting the muscle.
Treatment may include:
- Gentle hands-on therapy
- Soft tissue release
- Swelling management
- Education on what to avoid
- Light guided movement
- Safe pain-free walking drills
We also make sure you understand what NOT to do early on — like stretching aggressively or pushing through pain — both of which can delay recovery.

Phase 2 – Restoring Strength and Flexibility
Once pain settles, we start rebuilding strength safely.
Physiotherapy focuses on:
- Adductor muscle strengthening
- Hip and core stability
- Gradual mobility work
- Load progression
- Balance and control
This is the stage most people skip — and it’s exactly why many groin strains return.
Phase 3 – Building Power, Speed and Confidence
If you play sport, run or train at the gym, your groin needs to handle more than just day-to-day activity.
So we progress to:
- Running mechanics
- Change of direction training
- Sport-specific drills
- Power and agility
- Plyometric training when appropriate
This ensures you don’t just recover — you return stronger and more resilient than before.
Real Patient Success Story – From a Surrounding Suburb Near Frenchs Forest NSW
Recently we saw a patient who came to our Frenchs Forest NSW clinic from a nearby surrounding suburb after pulling their groin playing weekend football. They tried resting for two weeks, but every time they returned to running, the pain came back.
During assessment, we found:
- A Grade 2 groin strain
- Weak hip stabilisers
- Tightness through the adductors
- Poor control during quick direction changes
We started with hands-on treatment and guided early exercises. Within two weeks, their pain had significantly reduced. By week four they were running comfortably, and by week eight they were back playing full matches — stronger, confident and pain-free.
Now they’re back enjoying the game without constantly worrying their groin will go again.
How Long Should You Rest a Groin Strain?
Complete rest is rarely the answer.
Too much rest leads to:
- Weakness
- Tightness
- Delayed healing
- Higher risk of re-injury
A better approach is relative rest + guided rehab.
Your physio will help you stay active safely, while still allowing the injury to heal properly.

When Should You See a Physio?
Book an appointment if:
- Groin pain doesn’t improve after a few days
- Walking hurts
- Running or sport is painful
- You keep re-injuring it
- There is bruising, swelling or sharp pain
- Pain lingers beyond 2–3 weeks
- You’re unsure what you’ve actually injured
Early physio = faster recovery and less chance of re-injury.
Can I Speed Up Groin Strain Recovery Time at Home?
Yes — but it needs to be done correctly.
Helpful tips include:
- Avoid pushing through pain
- Don’t stretch aggressively early on
- Keep moving gently
- Strengthen progressively
- Follow guided rehab rather than guessing
And if you’re unsure, get it checked. A proper diagnosis saves time, frustration and ongoing pain.
Can Groin Strains Become Chronic?
Unfortunately, yes — especially if ignored or poorly managed.
Chronic Groin Strain Recovery Time issues can lead to:
- Ongoing pain
- Weakness
- Loss of speed and power
- Reduced performance
- Long-term tendon changes
Many athletes and active adults struggle for months simply because they never rehabilitated the injury properly.
The earlier you treat a groin strain, the faster the Groin Strain Recovery Time.
Frequently Asked Questions (FAQs)
How long does it take for a groin strain to heal?
Anywhere from 1–12+ weeks depending on severity. Physiotherapy helps speed recovery and ensures it heals strong.
Do I need a scan for a groin strain?
Most groin strains can be diagnosed clinically. Scans are only needed in severe or unclear cases.
Can I exercise with a groin strain?
Yes — but activity should be modified. Guided strengthening helps recovery without aggravating the injury.
Why does my groin strain keep coming back?
Usually because it never fully healed, strength wasn’t restored properly, or biomechanics weren’t addressed.
Can physiotherapy help groin strains heal faster?
Absolutely. Physio reduces pain, restores movement, rebuilds strength and prevents re-injury.
References & Further Reading
https://xphysio.com.au/blog
https://www.physio-pedia.com/Groin_Strain
https://orthoinfo.aaos.org/en/diseases–conditions/muscle-strain
https://www.sportsmedtoday.com/groin-strain-va-81.htm
Ready to Recover Faster?
If you’re dealing with groin pain, don’t just wait and hope it gets better. The right physiotherapy can help you heal faster, move confidently and get back to doing what you love.
Give us a call today on 9806 3077, or book online, just CLICK HERE.
If your ankle keeps rolling, gives way without warning, or still feels weak long after a sprain, you’re probably dealing with ankle instability. It’s incredibly common in walkers, runners and athletes — but the good news is, physiotherapy can fix it properly. In this blog, we’ll explain why it happens, what helps, and how to strengthen it for good.
What Is Ankle Instability?
Ankle instability is when your ankle feels loose, wobbly, weak or unreliable — especially when walking on uneven ground, changing direction quickly or playing sport. Many people describe it as feeling like the ankle might “roll again at any moment”.
This usually develops after one or more ankle sprains that never fully healed. Instead of regaining strength, mobility and stability, the ankle remains vulnerable, and each roll weakens it further.
Ankle instability can be:
- Mechanical instability – where the ankle ligaments are stretched or torn
- Functional instability – where balance, control and muscle reaction time are impaired
Most people actually have a combination of both.

Why Does the Ankle Keep Rolling?
The most common cause is a previous ankle sprain that didn’t rehab properly. After a sprain, the supportive ligaments are stretched, and the important stabilising muscles switch off. Without retraining these muscles and restoring control, the ankle stays weak.
But there are other contributors too:
✔ Weak Ankle and Foot Muscles
Muscles around the ankle (especially peroneals) are responsible for reacting quickly to sudden changes in position. If they’re weak or slow, the ankle gives way.
✔ Poor Balance and Proprioception
After injury, your body loses its awareness of ankle position. Without specific rehab, your reaction time slows — and you roll again.
✔ Ligament Laxity
Repeated sprains stretch the ligaments so much that they lose their ability to support the joint.
✔ Reduced Mobility
Ironically, some people also develop stiffness in other ankle structures, which forces movement through the unstable area.
✔ Poor Footwear or Surface Demands
Unsupportive shoes, uneven surfaces, trails, sand running or court sports all increase risk.
Common Symptoms of Ankle Instability
You may be dealing with ankle instability if you have:
- Repeated ankle sprains
- A “giving way” feeling
- Ongoing weakness
- Swelling after simple activities
- Pain on the outside of the ankle
- Trouble on uneven ground
- Poor confidence in the ankle
- Hesitation when sprinting, jumping or changing direction
Left untreated, ankle instability can lead to more serious issues like chronic pain, tendon strain, cartilage damage and early joint arthritis.
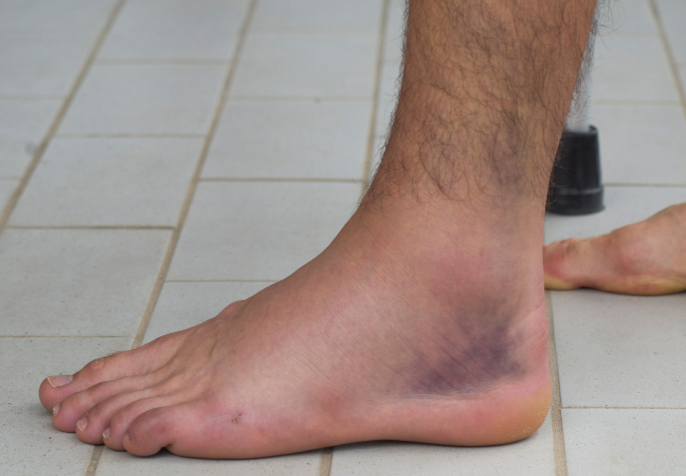
Why Rest Isn’t Enough
Most people sprain an ankle, limp for a few days, throw on an ankle brace, then go straight back to normal activity.
Unfortunately, that’s the perfect recipe for chronic ankle instability.
Rest may reduce pain, but it doesn’t:
- Strengthen weak muscles
- Restore ligament support
- Improve balance
- Retrain reflexes
- Build ankle confidence
Without proper rehabilitation, every sprain increases the chance of another — resulting in a cycle of repeated injury.
This is exactly where physiotherapy makes the biggest difference.
How Physiotherapy Fixes Ankle Instability
Physiotherapy doesn’t just treat the pain — it restores stability, mobility, strength and confidence so you can get back to walking, sport and daily life safely.
At X-Physio, treatment starts with a thorough assessment to understand:
- Which ligaments are affected
- How unstable the ankle actually is
- Strength deficits
- Balance and control
- Mobility restrictions
- Sport or activity demands
Then we design a treatment plan tailored specifically to you.

Hands-On Treatment — Reducing Pain and Improving Movement
Early on, the goal is to settle discomfort and restore normal movement. Treatment may include:
- Soft tissue release
- Joint mobilisation to improve ankle mechanics
- Swelling management
- Strapping or bracing short-term if required
- Gentle guided exercises
This phase also helps you start walking more confidently again.
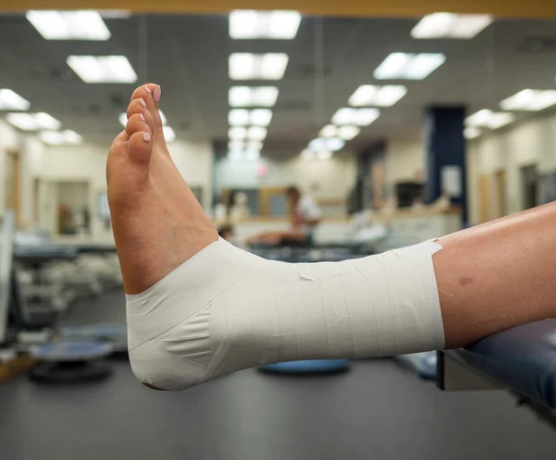
Strengthening — The Real Fix
Long-term results come from strength and control. That’s where physio really shines.
We target:
🔹 Peroneal and Lower Leg Strength
These muscles prevent rolling by stabilising the ankle.
🔹 Foot Intrinsic Strength
Small stabilising muscles in the foot are crucial for control.
🔹 Balance and Proprioception Training
Exercises retrain the ankle to react quickly again.
🔹 Functional Strength
We progress you from basic exercise to walking, stairs, running, hopping and sport-specific drills.
This builds real stability so your ankle stops rolling — not just temporarily feeling better.
Real Patient Example – From a Surrounding Suburb near Frenchs Forest NSW
Recently, we saw a patient who came to our Frenchs Forest NSW clinic from a nearby surrounding suburb after rolling their ankle multiple times over the past year. They loved bushwalking and weekend running but had lost confidence because the ankle kept giving way — sometimes even on flat ground.
They had previously tried rest, ice and ankle braces, but symptoms always returned.
During assessment, we identified:
- Significant ankle instability
- Weak peroneal muscles
- Poor single-leg balance
- Limited ankle mobility
- Hesitation and fear of movement
We started with mobility work and gentle strengthening, then progressed into structured stability exercises, balance retraining and graded return to running drills.
Within four weeks, they were walking confidently without the feeling of giving way. By eight weeks, they returned to trail running with strong ankle stability, better balance and far more confidence than before.
This story is extremely common — and physiotherapy makes an enormous difference.
How Long Does It Take to Fix Ankle Instability?
Recovery time depends on:
- Severity of ligament damage
- Number of previous sprains
- Activity level
- Consistency with rehab
Most people feel steadier within 2–4 weeks, with strong long-term stability often achieved within 8–12 weeks of structured physiotherapy.
Do I Need an MRI or X-Ray?
Not always. Most ankle instability can be diagnosed clinically during physiotherapy assessment. Imaging is only recommended if:
- There is severe swelling or bruising
- Pain persists longer than expected
- There is suspicion of fracture or significant tearing
- You’re not responding to treatment
Your physio will guide you if imaging is necessary.
Can Braces or Tape Help?
Yes — temporarily.
Bracing or taping can:
- Support the ankle
- Reduce rolling risk
- Build confidence early on
But they should never replace strengthening. The goal is to restore natural ankle stability so you don’t rely on external support long-term.
When Should You See a Physio?
Book an appointment if:
- Your ankle keeps rolling
- You’ve sprained your ankle more than once
- You lack confidence on uneven ground
- You’re avoiding activity because of your ankle
- You experience swelling or pain regularly
- You want to return to sport safely
The earlier you address ankle instability, the easier it is to fix — and the less damage occurs long-term.
Frequently Asked Questions (FAQs)
Why does my ankle keep rolling?
Usually because previous sprains never fully rehabilitated, leaving the ankle weak and unstable.
Can ankle instability heal on its own?
Rarely. Without strengthening, balance training and stability work, most unstable ankles continue to give way.
Is ankle instability serious?
It can become serious if ignored, leading to repeated sprains, chronic pain, tendon damage and early arthritis.
Can physiotherapy fix ankle instability?
Yes — with mobility work, strengthening, balance retraining and graded return to activity, physiotherapy is highly effective.
Do I need surgery?
Very few people need surgery. Most ankle instability improves significantly with structured physiotherapy.
References & Further Reading
https://xphysio.com.au/blog
https://www.physio-pedia.com/Chronic_Ankle_Instability
https://orthoinfo.aaos.org/en/diseases–conditions/chronic-lateral-ankle-instability
https://www.sportsmedtoday.com/ankle-sprain-va-22.htm
Ready to Stop Your Ankle Rolling?
If you’re tired of weak, wobbly ankles stopping you from walking, running or enjoying sport, physiotherapy can get you back feeling strong, confident and stable again.
Give us a call today on 9806 3077, or book online, just CLICK HERE.
