Let’s have a chat about carpal tunnel syndrome (CTS), a condition that can cause a fair bit of discomfort in your hand and wrist. Understanding what it is, why it happens, and how we can manage it through physiotherapy can make a world of difference.
What Is Carpal Tunnel Syndrome?
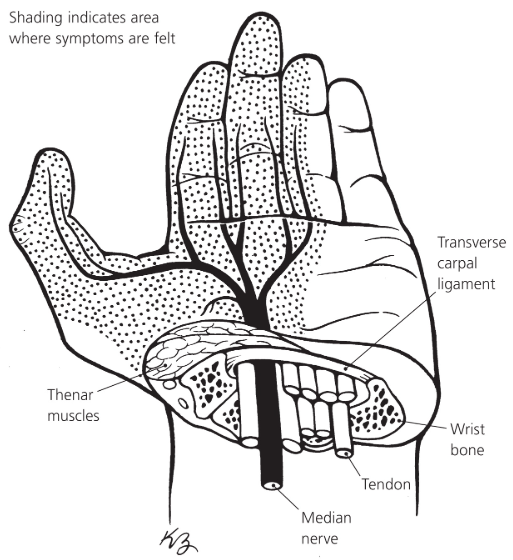
Imagine a narrow passageway on the palm side of your wrist—about the size of a twenty-cent coin. This is the carpal tunnel, and it houses the median nerve along with tendons that help bend your fingers. When this tunnel becomes cramped or the contents swell, it puts pressure on the median nerve, leading to symptoms like pain, numbness, and weakness in your hand.
Why Does It Happen?
Several factors can contribute to CTS:
- Repetitive Movements: Activities that involve repetitive wrist movements, such as typing or machine work, can increase the risk.
- Wrist Positioning: Keeping your wrist in a bent position for extended periods, like when writing or using a computer mouse, may contribute.
- Health Conditions: Conditions like diabetes, thyroid issues, or arthritis can play a role.
- Pregnancy: Hormonal changes and fluid retention during pregnancy can lead to swelling in the carpal tunnel.
- Anatomy: Some folks naturally have a smaller carpal tunnel, making them more susceptible.
What Are the Symptoms?
CTS often starts with a gradual onset of symptoms, including:
- Numbness or Tingling: Especially in the thumb, index, middle, and ring fingers.
- Pain: In the wrist, palm, or forearm.
- Weakness: You might find yourself dropping objects or having trouble with tasks that require fine motor skills.
- Night-Time Discomfort: Symptoms can be worse at night, sometimes waking you from sleep.
How Can Physiotherapy Help?
Physiotherapy offers a range of treatments to alleviate the symptoms of CTS and improve hand function:
- Education: Understanding the condition and how to manage it is crucial. Your physio can provide guidance on modifying activities to reduce strain on your wrist.
- Splinting: Wearing a wrist splint, especially at night, can keep your wrist in a neutral position, reducing pressure on the median nerve.
- Exercises: Specific exercises can help improve flexibility and strength in the wrist and hand. Here are some exercises that might be beneficial:
Median Nerve Gliding Exercises
These exercises help the median nerve move more freely through the carpal tunnel, reducing pressure and improving symptoms.
Wrist Flexor Stretch
This stretch targets the muscles on the underside of your forearm, helping to relieve tension that may contribute to CTS symptoms.

Wrist Extensor Stretch
Stretching the muscles on the top side of your forearm can also be beneficial in managing CTS discomfort.

Tendon Gliding Exercises
These exercises promote the smooth movement of tendons through the carpal tunnel, reducing stiffness and improving function.
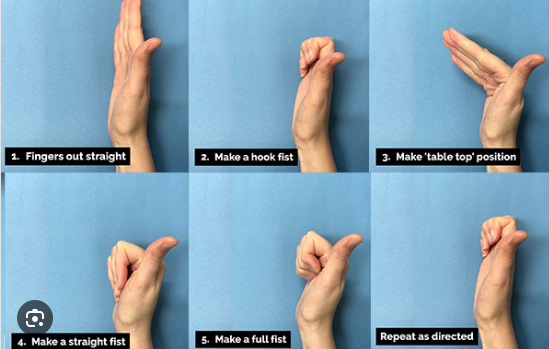
Grip Strengthening Exercises
Strengthening the muscles of the hand can improve overall function and help alleviate symptoms of CTS.

- Manual Therapy: Techniques like gentle mobilization of the wrist joints and soft tissue massage can reduce pain and improve mobility.
- Ergonomic Advice: Your physio can assess your work or home setup and suggest modifications to reduce strain on your wrist.
What Can You Do at Home?
In addition to physiotherapy, there are steps you can take to manage CTS:
- Activity Modification: Take regular breaks from repetitive tasks and avoid positions that overextend your wrist.
- Stretching: Incorporate gentle wrist and hand stretches into your daily routine.
- Ice Therapy: Applying ice to the wrist can help reduce inflammation and alleviate pain.
- Maintain a Healthy Lifestyle: Managing underlying health conditions and maintaining a healthy weight can reduce your risk.
When Should You Consider Surgery?
If symptoms persist despite conservative treatments, or if there’s significant nerve compression, surgical options may be considered. Surgery involves releasing the ligament that’s pressing on the median nerve to create more space in the carpal tunnel. However, many people find relief through physiotherapy and other non-surgical interventions.
Final Thoughts
Carpal tunnel syndrome can be a real nuisance, but with the right approach, you can manage the symptoms effectively. Physiotherapy offers a range of treatments tailored to your needs, aiming to reduce pain, improve function, and enhance your quality of life. If you’re experiencing symptoms of CTS, it’s a good idea to consult with a healthcare professional or physiotherapist to develop a treatment plan that’s right for you.
Remember, early intervention can prevent symptoms from worsening, so don’t hesitate to seek help if you’re experiencing discomfort in your hand or wrist.
Sources
1) Hingehealth
Physical Therapy for Carpal Tunnel: Tips & Best Exercises
Learn how physical therapy for carpal tunnel syndrome can help you manage symptoms and prevent future pain flares through targeted exercises.
2) Choose PT
Physical Therapy Guide to Carpal Tunnel Syndrome – Choose PT
Carpal tunnel syndrome is a common condition that causes pain, numbness, and weakness in the wrist and hand. CTS can affect the use of the entire arm.
3) Physiopedia
Carpal Tunnel Syndrome – Physiopedia
Carpal tunnel syndrome (CTS) is an entrapment neuropathy caused by compression of the median nerve as it travels through the wrist’s carpal tunnel.
4) ASSH
What is Carpal Tunnel Syndrome? | The Hand Society
5) Australian Sports Physiotherapy
Carpal Tunnel Syndrome Physio – Australian Sports Physiotherapy
Most carpal tunnel syndrome patients benefit from physiotherapy, particularly those with mild to moderate symptoms.
Carpal Tunnel Syndrome – Exercise Thought
Carpal Tunnel Syndrome (CTS) is a condition of the hand where the median nerve becomes compressed
When most of us think of physiotherapists, we often picture them helping people with sports injuries, sore backs, or post-surgery rehabilitation. But did you know that physiotherapists can also help treat headaches? Yep, you heard that right. If headaches are making your life miserable, seeing a physio might be a game-changer. Let’s dive into the types of headaches they can treat and how they work their magic to help you feel like yourself again.
Understanding Headaches: A Quick Overview
Before we get into the nitty-gritty, it’s worth knowing that not all headaches are the same. Different types have different causes, and that’s why the treatment varies. While some require medical intervention or medication, others can stem from physical issues that a physio can address. Things like poor posture, muscle tension, or even stress can trigger them that are within a physio’s expertise to manage.
Now, let’s look at the types of headaches physiotherapy can help with.
1. Tension Headaches
Tension headaches are incredibly common, and chances are you’ve experienced one at some point. They feel like a tight band squeezing around your head or a dull, aching pressure. Often, they will result from stress, poor posture, or prolonged time in one position (hello, desk workers!).
How can a physio help?
- Postural Corrections: Your physio w ill assess your posture and help you make adjustments to reduce strain on your neck and shoulders.
- Massage Therapy: Tense muscles, particularly in the neck, shoulders, and upper back, are often the culprits. Massage can work wonders to release that built-up tension.
- Exercise Programs: Simple exercises can strengthen your muscles, improve flexibility, and prevent future headaches.
2. Cervicogenic Headaches
Cervicogenic headaches are a mouthful to say, but they’re fairly straightforward in how they occur. They will often start in the neck but are felt in the head, and typically only on one side. They’re typically caused by joint or muscle issues in the neck, poor posture, or even an injury like whiplash.

How can a physio help?
- Manual Therapy: Techniques like joint mobilisation or manipulation can help restore proper movement and reduce pain.
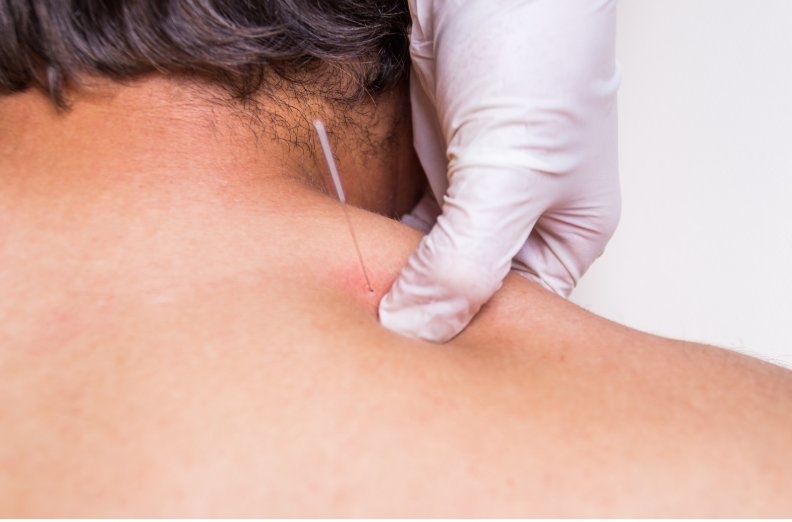
- Dry Needling: This technique involves inserting thin needles into trigger points in your muscles to relieve pain and tension.
- Neck Strengthening Exercises: Weak neck muscles can contribute to cervicogenic headaches, so your physio may give you targeted exercises to build strength.
3. Migraines
Migraines are a bit more complex. They’re often accompanied by nausea, sensitivity to light or sound, and a throbbing pain that can last for hours or even days. While migraines are usually managed with medication, physiotherapy can play a supportive role, especially if physical triggers are contributing to them.
How can a physio help?
- Identifying Triggers: Your physio can help you identify physical triggers like tension or poor posture that may be setting off your migraines.
- Relaxation Techniques: Stress and tension can exacerbate migraines, so learning how to relax your muscles can be incredibly helpful.
- Improving Sleep Posture: How you sleep matters. Your physio might recommend changes to your sleep setup to reduce strain on your neck.
4. Cluster Headaches
Cluster headaches are less common but incredibly intense. They’re often described as a piercing or burning pain around one eye and typically occur in clusters (hence the name) over weeks or months. While physios can’t treat the root cause of the cluster type, they can help manage some of the secondary symptoms.
How can a physio help?
- Pain Management Strategies: Techniques like gentle massage and relaxation exercises can help reduce overall tension and discomfort.
- Improving Overall Wellbeing: Your physio might focus on general health and stress management to support your body during these episodes.
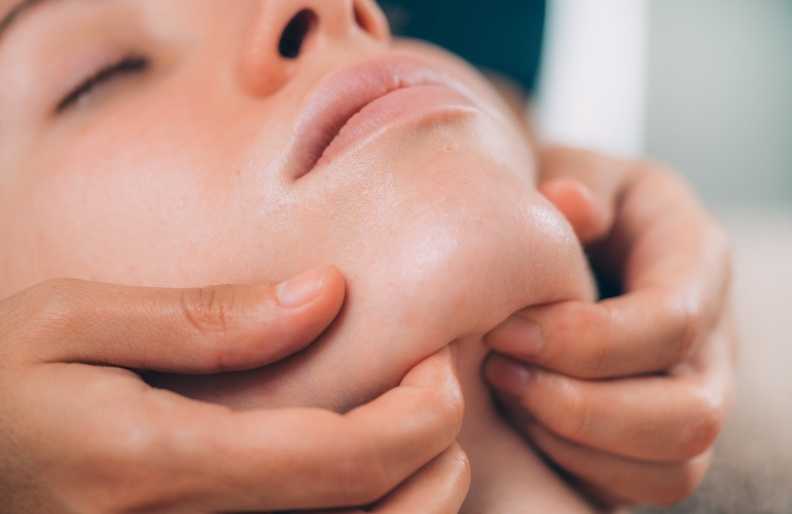
5. TMJ-Related Headaches
Your temporomandibular joint (TMJ) connects your jaw to your skull, and issues with this joint can lead to headaches. TMJ-related pain is often felt in the jaw with clicking or popping sounds, and even difficulty opening or closing your mouth.
How can a physio help?
- Jaw Exercises: Specific exercises can improve the function of your TMJ and reduce pain.
- Massage and Stretching: Releasing tension in the jaw and surrounding muscles can work wonders.
- Postural Adjustments: Since your jaw and neck are closely linked, improving your posture can alleviate symptoms.
6. Headaches Following a Concussion
If you’ve had a concussion, headaches can linger long after the initial injury. These are often due to neck issues, muscle tension, or even changes in how you move as your body compensates for the injury.
How can a physio help?
- Neck Rehabilitation: Addressing any stiffness or weakness in your neck can help reduce the pain.
- Balance and Coordination Exercises: If your concussion has affected your balance, your physio can guide you through exercises to restore it.
- Education: Your physio can teach you strategies to pace yourself during recovery and avoid activities that might aggravate your symptoms.
How to Know If Your Headache Is Physio-Treatable
Not every headache will benefit from physiotherapy. If it is sudden, severe, or accompanied by symptoms like vision changes, confusion, or weakness, you should seek medical attention immediately. But if it seems tied to physical tension, mental stress, posture, or previous injuries, a physio might be just what you need.
Signs your physio might be able to help:
- You notice stiffness or discomfort in your neck, shoulders, or jaw.
- Your pain comes on after sitting for long periods.
- You’ve had a recent injury or accident.
- Stress or tension seems to make things worse.
What to Expect During a Physio Appointment
If you’ve never been to a physio for headaches before, you might be wondering what’s involved. Here’s a quick rundown:
- Assessment: Your physio will ask about your pain history, lifestyle, and any other symptoms you’re experiencing. They’ll also assess your posture, muscle tension, and joint movement.
- Treatment Plan: Based on their findings, your physio will create a tailored treatment plan. This might include manual therapy, strengthening exercises, or advice on ergonomics.
- Hands-On Treatment: Techniques like massage, mobilisation, or dry needling may be used to address tension and pain.
- Home Exercises: Your physio will likely give you some exercises to do at home to support your recovery and prevent future pain.

Tips for Preventing Headaches
Prevention is always better than cure, right? Here are some tips to keep headaches at bay:
- Move Regularly: If you sit for long periods, take breaks to stretch and move around.
- Check Your Posture: Make sure your desk setup is ergonomic and that you’re not slouching.
- Manage Stress: Find ways to relax, whether it’s through yoga, meditation, or a walk in the park.
- Sleep Well: A good night’s sleep can do wonders for headache prevention. Pay attention to your pillow and sleeping position.
Wrapping It Up
Headaches can be a real pain—literally—but they don’t have to take over your life. Physiotherapy offers a range of treatments that can help alleviate the pain and prevent it from coming back. Whether it’s tension headaches, cervicogenic headaches, or even migraines, a physio can help you tackle the root cause and get back to feeling your best.
So, if headaches are getting you down, why not book an appointment with a physiotherapist at XPhysio today? You’ve got nothing to lose—except the headache, of course!
Knee swelling, often referred to as “water on the knee,” can be a literal pain to deal with. It’s a condition where excess fluid builds up in or around your knee joint, making it swollen, stiff, and sometimes quite painful. As a physio, I’ve seen my fair share of swollen knees walk (or hobble) through the clinic doors. Let’s dive into what knee swelling is, why it happens, and how physiotherapy can help you get back on your feet.
What Exactly Is Knee Swelling?
Knee swelling occurs when there’s an abnormal accumulation of fluid in the knee joint. This can happen inside the joint capsule (intra-articular) or outside it (extra-articular). The fluid can be synovial fluid—the slippery stuff that lubricates your joint—or, in more severe cases, blood or pus. Swelling is your body’s way of saying, “Something’s not right here,” and it’s often accompanied by stiffness, pain, and a reduced range of motion.

Common Causes of Knee Swelling
1. Injury
Acute injuries like a torn ligament, meniscus tear, or a fracture can cause knee swelling. A direct blow or twist of the knee often triggers an inflammatory response, leading to fluid accumulation.
2. Arthritis
Conditions like osteoarthritis, rheumatoid arthritis, or gout can lead to chronic knee swelling. In osteoarthritis, for instance, the cartilage wears down over time, irritating the joint and causing swelling.
3. Infection
A septic joint, although less common, is a serious cause of knee swelling. This requires urgent medical attention to prevent long-term damage.
4. Overuse or Repetitive Strain
Sometimes, doing too much too soon—whether it’s running, squatting, or even gardening—can irritate the knee joint and lead to fluid build-up.
5. Systemic Conditions
Autoimmune diseases, like lupus, or metabolic conditions, like gout or pseudogout, can also contribute to knee swelling.
Symptoms to Watch For
How do you know if you’re dealing with knee swelling? Here are some tell-tale signs:
- Swelling around or within the knee joint
- When comparing one knee to the other, they don’t look symmetrical
- A feeling of heaviness or tightness
- Pain, especially when bearing weight
- Stiffness and difficulty bending or straightening the knee
- Reduced range of motion
- Warmth or redness (this could signal infection or inflammation)
If the swelling comes on suddenly after an injury or is accompanied by fever, chills, or severe pain, don’t muck around—see a doctor straight away.
How Physiotherapy Can Help
Physiotherapy is a game-changer when it comes to managing knee swelling. Here’s how it works:
1. Reducing Swelling and Pain
First things first: we focus on reducing the swelling and easing your pain. This often involves:
- P.E.A.C.E Protocol: Protect, Elevate, Avoid Anti Inflammatory Medication, Compress, and Education regarding your injury are the best steps initially when you notice swelling.
- Gentle Range of Motion Exercises: Keeping the joint moving—without overdoing it—prevents stiffness and promotes fluid drainage.
2. Identifying the Underlying Cause
A thorough assessment helps us figure out what’s causing your knee swelling. Is it an injury? Arthritis? Something else? Understanding the root cause is crucial for tailoring your treatment plan.
3. Restoring Range of Motion
Once the swelling is under control, we work on getting your knee moving properly again. Techniques might include:
- Manual Therapy: Hands-on techniques to mobilise the joint and surrounding tissues.
- Stretching Exercises: Targeting the muscles around your knee, like your quads, hamstrings, and calves.
4. Strengthening Muscles
A small amount of knee swelling causes the quadriceps muscle to deactivate, making it very hard to contract this muscle. Over time, the muscle can shrink causing imbalances. Weak muscles can put extra stress on your knee joint, so strengthening the surrounding muscles—especially your quads, hamstrings, and glutes—is a must. We’ll start with gentle exercises and progress as your knee improves.
5. Improving Biomechanics
Poor movement patterns can exacerbate knee issues. We’ll assess your gait, posture, and functional movements (like squats or lunges) to identify any problems. Small tweaks can make a big difference.
6. Preventing Recurrence
Finally, we’ll arm you with strategies to prevent future knee swelling. This might involve a mix of strengthening, stretching, and activity modification. If you’re an athlete, we’ll tailor your rehab to get you back to your sport safely.
Treatment Techniques in the Physio Toolkit
1. Taping or Bracing
K-taping or using a brace can provide support, reduce swelling, and improve proprioception (your sense of joint position).

2. Hydrotherapy
Exercising in water is a fantastic way to reduce joint stress while improving strength and range of motion.

3. Dry Needling
These techniques can help relieve pain and promote healing by targeting trigger points or stimulating your body’s natural healing processes.
4. Education and Lifestyle Advice
We’ll guide you on activity modification, weight management (if necessary), and other lifestyle factors that can impact knee health.
When to Seek Further Help
While physio can do wonders, there are times when you might need additional medical input. If your knee swelling is caused by an infection, significant injury, or an underlying medical condition, you may need medications, a corticosteroid injection, or even surgery.
Managing Knee Swelling at Home
While physio is essential, there are things you can do at home to complement your treatment:
Stay Active: Gentle, low-impact activities like walking or cycling can keep your knee moving.
Use Ice for Pain Relief: Apply ice for 15-20 minutes every couple of hours during the acute phase.
Elevate Your Leg: Prop your leg up on a pillow to reduce swelling.
Maintain a Healthy Weight: Carrying less weight reduces stress on your knee joints.
Don’t Overdo It: Listen to your body and avoid activities that worsen your symptoms. This can often be a delayed response, so pay attention for at least 24 hours after activity.
Real-Life Case Study
Let’s take the example of Sarah, a 42-year-old recreational netball player who came to see me with a swollen knee. After a thorough assessment, we identified that she’d strained her medial collateral ligament (MCL) during a game.
We started with P.E.A.C.E protocol and some gentle range of motion exercises. Once the swelling subsided, we worked on strengthening her quads and glutes and improving her movement patterns. Sarah was back on the court within eight weeks, armed with a proper warm-up routine and some K-taping for extra support.
Final Thoughts
Knee swelling can be a frustrating setback, but with the right approach, it doesn’t have to sideline you for long. Physiotherapy offers a holistic, hands-on approach to managing the condition, addressing not just the symptoms but also the underlying causes. Whether it’s a niggling injury, arthritis, or something else, a good physio will guide you through the recovery process and help you get back to doing what you love.
If your knee’s been playing up and you’re not sure where to start, don’t hesitate to book in with one of our physiotherapist’s at XPhysio today. After all, it’s better to tackle the problem head-on than to let it linger—your knees will thank you for it!
Elbow injuries might not be the first type of injury that comes to mind, but this joint works hard for you every day. From lifting groceries to typing away at your desk, your elbows are constantly in action. But what happens when things go wrong? Let’s dive into the world of common elbow injuries, explore why they happen, and talk about how physiotherapy can help you get back on track.
Why is the Elbow So Susceptible to Injury?
The elbow is a complex joint. It’s a hinge joint (like your knee) but with a twist—literally. The elbow allows for both bending and rotating your forearm. This range of motion is thanks to the coordination of three bones: the humerus (upper arm bone), the ulna, and the radius (forearm bones), along with a network of muscles, tendons, and ligaments.
Because of its complexity and regular use, the elbow injuries can be common. Overuse, poor technique during sports, or even something as simple as a slip and fall can lead to trouble. The good news? Physiotherapy can often work wonders in helping you recover.

Common Elbow Injuries
Let’s take a look at some of the most frequent elbow problems people face:
1. Tennis Elbow (Lateral Epicondylitis)
Don’t be fooled by the name—you don’t need to pick up a racquet to get tennis elbow. This condition is caused by repetitive stress on the tendons that attach to the lateral (outer) part of your elbow. Typing, gardening, or even holding a paintbrush can lead to this painful overuse injury. I would say this is the most common elbow injury to present in our clinic.
Symptoms:
- Pain or burning on the outside of the elbow
- Weak grip strength
- Pain that worsens with repetitive movements
How Physiotherapy Helps:
A physio will assess the cause of your pain and tailor a treatment plan. Common approaches include:
- Manual therapy: Techniques to improve blood flow and reduce tension in the affected area.
- Stretching and strengthening exercises: To ease strain on the tendons and improve their resilience.
- Ergonomic advice: Modifications to your work or daily activities to prevent further load.
2. Golfer’s Elbow (Medial Epicondylitis)
Similar to tennis elbow, golfer’s elbow affects the tendons—but this time on the inner side of your elbow. You don’t have to be a golfer to experience it; any repetitive wrist or finger motion can put you at risk. As the tendon does not have a great blood supply, this elbow injury can take weeks, if not months to resolve.
Symptoms:
- Pain and tenderness on the inside of the elbow
- Weakness in the wrist or hand
- Stiffness or discomfort when gripping objects
How Physiotherapy Helps:
Your physio might use:
- Dry needling: To relieve pain and improve circulation.
- Gradual loading exercises: To strengthen the tendons and improve flexibility.
- Activity modifications: Guidance on how to reduce strain during repetitive tasks.
3. Elbow Sprains and Ligament Injuries
Ligaments hold the elbow joint together and keep it stable. A sprain occurs when these ligaments are overstretched or torn, often due to trauma like a fall or a sudden twisting motion.
Symptoms:
- Swelling and bruising around the elbow
- Pain when moving the joint
- A feeling of instability in the elbow
How Physiotherapy Helps:
Treatment will depend on the severity of the sprain but might include:
- Immobilisation: Using a brace or sling to allow healing.
- Controlled exercises: To restore range of motion and strength gradually.
- Proprioception training: To help your elbow regain its sense of position and stability.
4. Fractures
Elbow fractures are most commonly caused by falls or direct impact. They can affect any of the three bones in the joint and often require immobilisation or even surgery to heal properly. It is important that a correct diagnosis is made for this elbow injury.
Symptoms:
- Severe pain and swelling
- Difficulty or inability to move the elbow
- Obvious deformity (in some cases)
How Physiotherapy Helps:
Once the fracture has been treated and stabilised, physio plays a crucial role in recovery:
- Restoration of movement: Exercises to regain flexibility and reduce stiffness.
- Strength rebuilding: Gradual progression to strengthen the muscles around the joint.
- Scar tissue management: Techniques to minimise stiffness from surgery or immobilisation.
5. Bursitis
The elbow has a small, fluid-filled sac called a bursa that cushions the joint. Bursitis occurs when this sac becomes inflamed, often due to prolonged pressure (like leaning on your elbows for too long) or repetitive motion.This elbow injury tends to cause pain at the back of your elbow.
Symptoms:
- Swelling at the back of the elbow
- Pain when touching or moving the elbow
- Warmth or redness around the joint (if infected)
How Physiotherapy Helps:
A physio might recommend:
- Ice and compression therapy: To reduce inflammation.
- Gentle exercises: To maintain joint mobility without aggravating the bursa.
- Postural advice: Tips to avoid pressure or repetitive actions that irritate the area.
6. Ulnar Nerve Entrapment (Cubital Tunnel Syndrome)
The ulnar nerve runs through a narrow tunnel on the inside of your elbow. When compressed or irritated, it can cause numbness, tingling, or weakness in your hand and fingers.This elbow injury can be caused by a range of factors and often requires a scan to further investigate the cause.
Symptoms:
- Tingling or numbness in the ring and little fingers
- Weak grip strength
- Pain or aching on the inside of the elbow
How Physiotherapy Helps:
Treatment might include:
- Nerve gliding exercises: To help the ulnar nerve move more freely.
- Splinting: To keep the elbow in a position that reduces pressure on the nerve.
- Postural adjustments: Advice on avoiding prolonged elbow flexion or other aggravating positions.
How to Prevent Elbow Injuries
Prevention is always better than cure! Here are some practical tips to prevent an elbow injury:
- Warm up properly: Before any physical activity, ensure your muscles and tendons are ready to go.
- Use correct technique: Whether you’re lifting weights or typing, proper form can reduce strain on your joints.
- Take breaks: Avoid repetitive motions for long periods; stretch and rest regularly.
- Strengthen your forearms: Stronger forearm muscles provide better support for your elbow.
- Be mindful of posture: Avoid slouching or leaning on your elbows for extended periods.

Why Physiotherapy is Key
Physiotherapy isn’t just about exercises—it’s about a holistic approach to recovery. Your physio will consider your lifestyle, goals, and the underlying cause of your injury to create a personalised treatment plan. Here’s why physio makes such a difference:
- Accurate diagnosis: Your physio can identify the root cause of your elbow pain and address it effectively. Often this can be done with a clinical assessment only which will not require a scan, therefore saving time and money.
- Hands-on techniques: From massage to joint mobilisation, physios use a range of manual therapies to aid recovery.
- Education: You’ll learn about your injury, how to prevent it in the future, and how to make lasting changes.
- Progressive exercises: A step-by-step plan ensures you regain strength, mobility, and confidence without overdoing it.
Final Thoughts
Elbow injuries don’t have to hold you back. Whether it’s a niggling ache from too much computer work or a more serious condition, physiotherapy offers effective solutions to help you recover. By understanding your injury and working with a physio, you’ll be on your way to stronger, pain-free elbows in no time.
So, if your elbow is giving you grief, don’t ignore it. Reach out to XPhysio today and take the first step towards recovery. Your elbows will thank you!
Neck pain is a condition that’s more common than many people realise. It doesn’t just affect older adults or those in physically demanding jobs—neck pain can strike people of all ages, backgrounds, and lifestyles. Whether it stems from a car accident, poor posture while working at a desk, or repetitive strain from daily activities, neck pain can be debilitating, disrupting your ability to enjoy life to the fullest.
In fact, neck pain has become an increasingly prevalent health issue, particularly in the modern world where sedentary lifestyles, prolonged use of electronic devices, and poor ergonomics are more common than ever. What was once seen as an isolated issue, affecting only a specific group of people, is now understood to be a widespread problem that impacts people from all walks of life.
Thankfully, treatment with physiotherapy and exercise physiology offers effective, science-based strategies to help individuals not only manage neck pain but also recover and prevent it from recurring. In this blog, we’ll take an in-depth look at the various causes of neck pain, common injuries associated with it, and the role that physiotherapy and exercise physiology can play in helping you recover fully.
The Anatomy of the Neck: A Complex System
Before delving into the specific causes of neck pain, it’s essential to understand the basic anatomy of the neck. The neck is a highly complex structure made up of bones, muscles, tendons, ligaments, nerves, and blood vessels. The cervical spine, which supports the neck, consists of seven vertebrae (C1 to C7). These vertebrae are connected by discs that act as cushions, allowing for flexibility and shock absorption.
The muscles of the neck are responsible for a wide range of movements, from simple nodding and turning motions to more complex movements like looking up or down. Moreover, the neck serves as the bridge between the brain and the rest of the body, housing critical nerve pathways that control motor and sensory functions. Even a minor injury or strain in this delicate system can result in significant pain, limited mobility, and dysfunction.
The neck’s intricate structure makes it highly susceptible to injury, especially when subjected to physical or emotional stress. From whiplash in a car accident to tension headaches caused by muscle strain, the variety of factors that can affect the neck is vast.
Common Causes of Neck Pain
Neck pain can arise from a variety of causes, some of which may seem harmless at first glance. Below are some of the most common sources of neck pain:
1. Poor Posture
One of the most prevalent causes of neck pain in the modern era is poor posture. This issue is particularly widespread among people who spend long hours sitting at desks or working on computers. When you sit for prolonged periods with your head tilted down or poking forward and your shoulders rounded, it puts added strain on the muscles in your neck. Over time, this excessive load can lead to chronic neck pain, stiffness, and even headaches.
2. Text Neck
Closely related to poor posture, “text neck” refers to the strain caused by looking down at smartphones, tablets, or other electronic devices for extended periods. In today’s digital age, many people spend hours each day hunched over screens, placing excessive stress on the cervical spine. The human head weighs about 2.5 to 5 kilograms, and when you tilt your head forward to look at a screen, the pressure on your neck can increase dramatically—up to 27 kilograms when the head is tilted at a 60-degree angle!
3. Whiplash
Whiplash is a common injury that occurs when the neck is rapidly jerked backward and then forward, often in a car accident or other traumatic event. This sudden motion can strain or tear the muscles, tendons, and ligaments in the neck, leading to acute pain and limited mobility. While some people recover from whiplash within a few weeks, others may experience chronic neck pain that lasts for months or even years.

4. Repetitive Strain Injuries
Engaging in repetitive motions that involve the neck, such as turning your head frequently or carrying heavy loads on one shoulder, can lead to repetitive strain injuries (RSIs). These injuries occur when the muscles and tendons in the neck become overused and inflamed, causing pain, stiffness, and limited range of motion. Athletes, tradies, and individuals with physically demanding jobs are especially prone to RSIs.
5. Degenerative Disc Disease
As we age, the discs in our cervical spine can begin to degenerate or wear down. This condition, known as degenerative disc disease, is a common cause of neck pain in older adults. The discs act as shock absorbers between the vertebrae, but when they begin to break down, they lose their ability to cushion the spine, leading to pain, stiffness, and reduced mobility. In severe cases, the condition can also cause herniated discs or bone spurs, which may press on the nerves and lead to further pain or numbness.
6. Muscle Strain
Muscle strain is another frequent cause of neck pain and can occur for a variety of reasons. Something as simple as sleeping in an awkward position or carrying a heavy bag can lead to strained muscles in the neck. People who engage in strenuous physical activities, such as weightlifting or contact sports, may also be prone to muscle strain.
7. Stress and Anxiety
Emotional stress and anxiety can take a significant toll on the body, particularly in the neck and shoulders. When you’re stressed, your muscles tend to tense up, and this tension often manifests in the neck and upper back. Chronic stress can lead to muscle stiffness, headaches, and persistent neck pain.
The Implications of Chronic Neck Pain
For many people, neck pain isn’t just a temporary inconvenience—it can have long-lasting implications for their health and quality of life. Chronic neck pain can lead to a range of physical, emotional, and social challenges, including:
1. Limited Mobility
When neck pain becomes chronic, it can significantly reduce your range of motion. Simple tasks like turning your head to look behind you or tilting your head to one side can become difficult or even impossible. This limited mobility can affect your ability to drive, exercise, or perform daily activities.
2. Headaches and Migraines
Neck pain is often accompanied by tension headaches or migraines, particularly when the pain is caused by muscle strain or poor posture. These headaches can be debilitating, making it difficult to concentrate, work, or enjoy leisure activities.
3. Sleep Disruptions
Chronic neck pain can make it challenging to find a comfortable sleeping position, leading to sleep disruptions and insomnia. Lack of sleep can, in turn, exacerbate pain levels, creating a vicious cycle that’s hard to break.
4. Emotional Distress
Living with chronic pain can take a toll on your mental health, leading to feelings of frustration, anxiety, or depression. The constant discomfort can make it difficult to enjoy hobbies, social activities, or time with loved ones, leading to a reduced quality of life.
5. Reduced Productivity
When neck pain becomes severe, it can affect your ability to work or complete everyday tasks. Whether you’re dealing with pain that prevents you from focusing on your job or you’re missing work due to frequent medical appointments, chronic neck pain can reduce your productivity and, in some cases, lead to financial stress.
How Physiotherapy Can Help
Physiotherapy is a highly effective treatment for neck pain, especially when it’s caused by musculoskeletal issues like poor posture, whiplash, or muscle strain. The goal of physiotherapy is to improve the function and mobility of the neck while reducing pain and preventing future injuries.
Here’s how physiotherapy can help you recover from neck pain:
1. Manual Therapy
Physiotherapists often use hands-on techniques, known as manual therapy, to relieve tension in the muscles and joints of the neck. This may involve gentle manipulation of the cervical spine to improve alignment, mobilisation of the neck joints, or massage to reduce muscle tone.
2. Postural Correction
A significant component of physiotherapy for neck pain involves correcting poor posture. Your physiotherapist will assess your posture and identify any imbalances that may be contributing to your pain. They will then provide exercises and stretches designed to strengthen the muscles that support your neck and improve your overall posture. Over time, these exercises can help alleviate pain and prevent future injuries.
3. Strengthening Exercises
Weak muscles in the neck, shoulders, and upper back can contribute to chronic neck pain. A physiotherapist will develop a personalised exercise program to target these weak areas and build strength and endurance. Strengthening the muscles that support your neck can improve your posture, reduce strain on your cervical spine, and enhance your overall function.
4. Stretching and Flexibility Training
In addition to strengthening exercises, physiotherapists often recommend stretches to improve flexibility and reduce tension in the neck and surrounding muscles. Gentle stretching can help relieve spasm in the muscles and improve your range of motion, making it easier to move without pain.
5. Ergonomic Advice
Many cases of neck pain are related to poor ergonomics in the workplace or at home. A physiotherapist can provide advice on how to set up your workstation, including the proper height of your chair, desk, and computer monitor, as well as how to position your body to reduce strain on your neck. Small changes in your environment can make a significant difference in preventing neck pain.
6. Education and Self-Management
One of the most valuable aspects of physiotherapy is the education and guidance it provides. Your physiotherapist will teach you how to manage your neck pain independently, including techniques for reducing pain at home, preventing flare-ups, and maintaining a healthy posture. This empowers you to take control of your recovery and avoid future injuries.
The Role of Exercise Physiology in Neck Pain Recovery
While physiotherapy focuses on manual techniques and exercises to relieve pain and improve mobility, exercise physiology takes a broader approach to rehabilitation. Exercise physiology is the study of how physical activity impacts the body, and exercise physiologists use this knowledge to design exercise programs that promote health, fitness, and recovery.
For individuals dealing with chronic neck pain, an exercise physiologist can develop a personalised exercise plan that complements the work done in physiotherapy. Here’s how exercise physiology can help:
1. Individualised Exercise Programs
An exercise physiologist will take into account your overall health, fitness level, and specific neck pain issues when designing an exercise program. This may include a combination of strength training, cardiovascular exercise, and flexibility training, all tailored to your needs. Regular exercise can improve your overall fitness, reduce pain, and prevent future neck problems.
2. Injury Prevention
One of the primary goals of exercise physiology is to prevent future injuries by addressing the underlying causes of neck pain. By improving your posture, increasing your strength and flexibility, and teaching you how to move correctly, an exercise physiologist can help you avoid the repetitive motions and poor habits that lead to neck pain.
3. Whole-Body Approach
While physiotherapy often focuses on the neck and upper body, exercise physiology takes a whole-body approach to recovery. An exercise physiologist will consider how other areas of your body may be contributing to your neck pain, such as poor core strength or imbalances in your hips or legs. By addressing these issues, they can help you achieve long-lasting relief from neck pain.
4. Chronic Pain Management
For individuals with chronic neck pain, exercise can play a crucial role in managing pain and improving quality of life. Exercise has been shown to release endorphins, the body’s natural painkillers, and reduce inflammation. Regular physical activity can also improve mood, increase energy levels, and reduce the emotional toll of chronic pain.
5. Improving Mobility and Function
Exercise physiology can also help individuals with neck pain improve their overall mobility and function. Through targeted exercises, you can regain the strength and flexibility needed to perform everyday tasks without pain. This can enhance your ability to work, exercise, and engage in activities you enjoy.

Conclusion: A Holistic Approach to Neck Pain Recovery
Neck pain can be a frustrating and debilitating condition, but it doesn’t have to control your life. By understanding the causes of your pain and seeking the right treatment, you can recover fully and prevent future injuries. Physiotherapy and exercise physiology offer complementary approaches to neck pain recovery, providing both immediate relief and long-term solutions.
Physiotherapy helps address the root causes of neck pain, whether it’s poor posture, muscle strain, or injury, through manual therapy, exercises, and education. Meanwhile, exercise physiology takes a broader approach to rehabilitation, focusing on improving overall fitness, preventing future injuries, and managing chronic pain.
Together, these disciplines offer a holistic approach to neck pain recovery, helping you regain your strength, mobility, and quality of life. If you’re dealing with neck pain, consider consulting with a health professional at XPhysio today. With the right care and guidance, you can overcome neck pain and get back to living pain-free.

Ankle sprains are some of the most common injuries, making up a significant portion of visits to emergency departments, especially among both the general public and athletes. These injuries can happen to anyone, whether you’re a weekend warrior, a seasoned athlete, or just walking down the street and miss a step. Twisting the ankle inward, known as a lateral sprain, is the most typical type of injury, and without proper management, it can have long-lasting effects. Despite being a common injury, many people underestimate how crucial it is to take care of a sprained ankle, often ignoring it or assuming it will heal on its own. Unfortunately, that’s not always the case, and improper care can lead to recurring problems.
If you’ve sprained your ankle before, you know how frustrating it can be. The immediate pain, swelling, and inability to walk comfortably can throw off your daily routine. And what’s worse is that many people think it’s okay to just “walk it off,” only to face issues down the track. Ankle sprains usually require physiotherapy treatment to achieve the best outcomes. Physiotherapists play a vital role by guiding patients through the rehabilitation process and ensuring they regain full function without the risk of ongoing instability.
the Role of Physiotherapy
Let’s break down what actually happens when you sprain your ankle. When your foot rolls inward, it stretches or tears the ligaments on the outside of your ankle, which are meant to stabilise the joint. These ligaments are like rubber bands holding everything together, and when they’re overstretched or torn, it results in pain, swelling, and often a sense of instability. You might feel like your ankle is going to give way, especially when walking on uneven surfaces.
Now, here’s where physiotherapy comes into the picture. Physiotherapists are trained to assess the severity of the sprain and help you manage the injury in the short and long term. They create tailored treatment plans that not only address the pain and swelling but also work on preventing future sprains. This might involve strengthening the muscles around the ankle, improving your balance, and working on proprioception (your body’s ability to sense movement and position).

The Importance of Early and Proper Treatment
Despite how often ankle sprains happen, it’s surprising that only about 50% of people actually seek medical attention. That’s concerning because when ankle sprains aren’t treated properly, they can lead to chronic instability. This means that you might experience persistent pain, swelling, and even recurrent sprains for months, or sometimes even years, after the initial injury.
In the acute phase, a lateral ankle sprain can cause severe pain and limit your ability to walk. In some cases, there’s even concern about possible fractures, but the good news is that only about 15% of ankle sprain cases involve a fracture. To help healthcare providers assess whether a fracture might be present, there’s something called the Ottawa Ankle Rules. These guidelines are used to determine whether an x-ray is necessary. Interestingly, the most accurate diagnosis of an ankle sprain usually happens around four or five days after the injury when the swelling has reduced, so immediate x-rays or ultrasounds aren’t always needed.
If you’ve just sprained your ankle, you’ll likely be feeling a combination of pain, frustration, and concern about how long it will take to recover. This is where early treatment plays a key role in speeding up the healing process. Instead of waiting for the injury to “go away” on its own, it’s best to get it checked out as soon as possible. The quicker you address the injury, the less likely it is that you’ll deal with ongoing issues.
Physiotherapy: Essential in Managing Ankle Sprains
Let’s dive into the nitty-gritty of how physiotherapy can help. A structured rehab program designed by a physiotherapist can significantly reduce your recovery time and minimise the chance of re-injury. Physiotherapists take a holistic approach to your recovery, focusing on not only the ankle but how the entire body moves and compensates for the injury.
1. Acute Management (First Few Days)
Immediately after the injury, managing pain and swelling is your top priority. The old RICE (Rest, Ice, Compression, Elevation) method is no longer the go-to standard for managing sprains. Instead, we now follow the PEACE and LOVE protocols.
- Protect: In the initial days, you want to protect the injured ankle. This could mean using crutches or wearing a brace to offload the joint and allow the ligaments time to start healing.
- Elevate: Elevating your ankle (keeping it higher than your heart) helps reduce swelling by encouraging fluid to drain from the area.
- Avoid Anti-Inflammatories: You might think that popping some ibuprofen or aspirin would help, but anti-inflammatory medication can actually interfere with the natural tissue regeneration process.
- Compress: Wrapping the ankle with a compression bandage or using supportive taping can help limit swelling.
- Educate: A huge part of the recovery process is understanding what’s going on in your body. Your physio will educate you about your injury and what you can expect throughout recovery.

2. Sub-Acute Management (After the First Week)
Once the acute phase has passed, you’ll start moving into what we call the sub-acute phase of rehab. During this time, your physiotherapist will focus on restoring your range of motion, strength, and balance. The goal is to get you moving again without causing more pain.
- Load: Introducing gentle movement and weight-bearing exercises is crucial during this phase. Your physio will guide you through exercises that improve mobility without aggravating the injury. These movements are designed to help maintain joint flexibility, prevent stiffness, and begin the process of strengthening the surrounding muscles.
- Optimism: Believe it or not, your mindset can play a huge role in how quickly you recover. Keeping a positive outlook and trusting in the process will go a long way in ensuring your rehabilitation is successful.
- Vascularisation: This is just a fancy term for improving blood flow to the injured area. Your physio might suggest some light cardio exercises, like cycling or swimming, to keep your heart pumping and help with healing.
- Exercise: Gradual, targeted exercises are introduced during this stage to prevent re-injury and promote healing. This is where the real work happens in terms of regaining your strength and stability.

3. Late-Stage Rehabilitation (Getting Back to Normal)
In the final stage of rehab, your physiotherapist will focus on returning you to your normal activities, whether that’s going back to sport, work, or just being able to walk without pain. This stage involves more advanced exercises that challenge your balance, coordination, and strength.
Return to Sport/Work: The goal here is to ensure you can safely return to your previous level of activity without the fear of re-injury. This might include exercises that mimic the movements you do in your sport or job, ensuring that your ankle is strong and stable enough to handle the load.
Why Comprehensive Rehabilitation is Key
One of the biggest mistakes people make when recovering from an ankle sprain is not following a structured rehab program. It’s easy to get advice from friends, family, or the internet, but the truth is, everyone’s injury is different. What worked for someone else may not work for you. Without proper guidance, you might be setting yourself up for a longer recovery time or, even worse, repeated sprains in the future.
A well-rounded rehabilitation program is essential for improving your joint’s range of motion, proprioception, and neuromuscular control. These are all fancy terms for ensuring your ankle moves the way it should, you have good balance, and your muscles work together properly. Without these things, you’re more likely to sprain your ankle again.
Physiotherapy doesn’t just focus on the injured ankle. It looks at how your whole body functions and how it compensates for the injury. For instance, if you’re limping because of your sprained ankle, other muscles in your body are working harder to pick up the slack. Your physio will work with you to address these imbalances, ensuring your entire body is functioning optimally.
The Role of Manual Therapy
Manual therapy can be a helpful part of the rehabilitation process, but it’s not a magic fix. It’s important to understand that while things like massage, joint mobilisation, and soft tissue work can provide temporary relief, they need to be combined with an exercise-based rehab program for long-term results. Your physio will use manual therapy techniques to help reduce pain and improve mobility, but the real progress comes from doing the prescribed exercises.

Conclusion
Ankle sprains are more than just a minor inconvenience – they require proper attention and care to prevent long-term issues. Physiotherapy is vital in managing these injuries from the acute phase through to full recovery. By following evidence-based guidelines and working with a qualified physiotherapist, you can expect better outcomes, reduced risk of chronic instability, and a smoother return to your daily activities.
If you’ve recently sprained your ankle, don’t hesitate to reach out for professional help. Our team at XPhysio Frenchs Forest are experts when it comes to this. Give us a call today – we’re here to guide you through every step of the way and get you back on your feet as soon as possible!
Plantar fasciitis is one of the most common foot injuries out there, but despite how often it occurs, it’s still a condition that leaves a lot of people scratching their heads. If you’ve ever woken up in the morning, stepped out of bed, and felt a sharp heel pain, you might already be familiar with it. This condition can cause a lot of discomfort during daily activities, whether you’re an athlete, someone who spends hours on their feet at work, or just someone who enjoys a casual stroll through the park.
The thing is, plantar fasciitis can affect anyone, and it’s not just limited to those who are physically active. It’s a tricky condition that can linger for weeks, months, or even longer if left untreated. The good news is that with the right understanding and some effective physiotherapy interventions, you can find relief and get back on your feet, pain-free. In this blog, we’ll unpack what plantar fasciitis is, what causes it, and how physiotherapy can be a game-changer in helping you overcome it.

What is Plantar Fasciitis?
Let’s start with the basics. The plantar fascia is a thick band of connective tissue that runs along the bottom of your foot. It connects your heel bone to your toes and plays a crucial role in supporting the arch of your foot. Its main job is to absorb the shock of each step you take while also providing stability to your foot structure.
Now, plantar fasciitis happens when this tissue gets irritated or overworked. What’s tricky about this condition is that it often starts gradually and can worsen over time. The tissue can become inflamed, and in chronic cases, it may even start to degenerate, leading to ongoing pain and discomfort. Most people with plantar fasciitis experience sharp, stabbing pain in the heel or along the arch of the foot. It’s particularly bad first thing in the morning or after you’ve been sitting for a long time and then try to stand up.
Sound familiar? If you’re nodding along, then you’re probably dealing with plantar fasciitis. But why does it happen, and what can you do about it? That’s what we’re here to figure out.
Causes of Plantar Fasciitis
There isn’t just one cause of plantar fasciitis. It’s often a combination of factors that contribute to the condition. If you’ve been diagnosed with plantar fasciitis, it’s likely that at least one of the following has played a role:
Overuse or High Impact Activities: If you’re someone who enjoys running, jumping or any kind of high-impact activity, you are at great risk for developing plantar fasciitis. Prolonged standing, like if you are on your feet all day for work can also strain the plantar fascia and lead to inflammation.
Foot Mechanics: Not everyon’s feet are built the same and certain foot mechanics can make you more prone to plantar fasciitis. For Example, if you have flat feet, high arches or abdnomal walking pattern, the way your foot strikes the ground can place extra stress on the foot.
Improper Footwear: We’ve all been guilty of wearing shoes that aren’t the best for our feet. Whether it’s unsupportive flats or those old running shoes that should have been replaced months ago, improper footwear can significantly contribute to plantar fasciitis. Shoes that lack arch support or cushioning can make it harder for your plantar fascia to do its job, leading to strain and pain.
Age and Weight: As we get older, our bodies naturally change, and the risk of developing plantar fasciitis increases. Additionally, carrying extra weight can put more pressure on the plantar fascia, making it more likely to become irritated or inflamed.
Understanding these causes is the first step in preventing plantar fasciitis from becoming a chronic problem. But if you’re already dealing with it, physiotherapy can help you manage and even eliminate the pain altogether.

Physiotherapy Interventions for Plantar Fasciitis
If you’ve been diagnosed with plantar fasciitis, physiotherapy is one of the best ways to address the issue. Physiotherapists use a variety of techniques to not only relieve your pain but also address the underlying causes so you can prevent the condition from coming back. Here’s a breakdown of some common physiotherapy interventions that are used to treat plantar fasciitis:
1. Strengthening Exercises
Strengthening the muscles of the foot and ankle is crucial for improving the tolerance of the plantar fascia. When you first experience symptoms, it’s important to rest and avoid activities that worsen the pain. But once your symptoms start to stabilise, strengthening exercises become essential.
These exercises target the muscles in your foot and ankle to gradually increase the load that your plantar fascia can handle. Your physiotherapist will guide you through exercises designed to strengthen the intrinsic muscles of the foot (those small but mighty muscles) as well as the calf muscles, which play a big role in supporting your foot’s arch. By building strength in these areas, you’re essentially giving your plantar fascia extra support, making it less likely to become irritated in the future.
2. Manual Therapy and Massage
Sometimes, the plantar fascia just needs a bit of hands-on care. Manual therapy techniques, such as massage and joint mobilisation, can help alleviate symptoms and improve mobility in your foot. These techniques work alongside your exercise program to provide relief from pain and stiffness.
Your physiotherapist might also use techniques to stretch the plantar fascia and surrounding tissues, which can relieve some of the tension and help restore normal movement patterns.
3. Orthotic Devices
Foot mechanics play a big role in plantar fasciitis, and sometimes, a simple shoe insert can make all the difference. Orthotic insoles are designed to provide additional support to your feet and correct any biomechanical issues that might be contributing to your pain.
If you’ve got flat feet or high arches, an orthotic device can help distribute the pressure more evenly across your foot, reducing the strain on your plantar fascia. Your physiotherapist will assess your foot mechanics and recommend the right kind of orthotic for you. In some cases, custom-made orthotics may be necessary to provide the best support.
4. Shockwave Therapy
One of the more advanced treatments available for plantar fasciitis is shockwave therapy. This non-invasive treatment uses high-energy sound waves to stimulate the healing process in your plantar fascia. The idea behind shockwave therapy is that it triggers an inflammatory response, which increases blood flow to the area and promotes healing.
Shockwave therapy is particularly effective for people with chronic plantar fasciitis who haven’t responded well to other treatments. It can help reduce pain and improve function by breaking up any calcification that has built up in the tissue and encouraging new tissue growth.
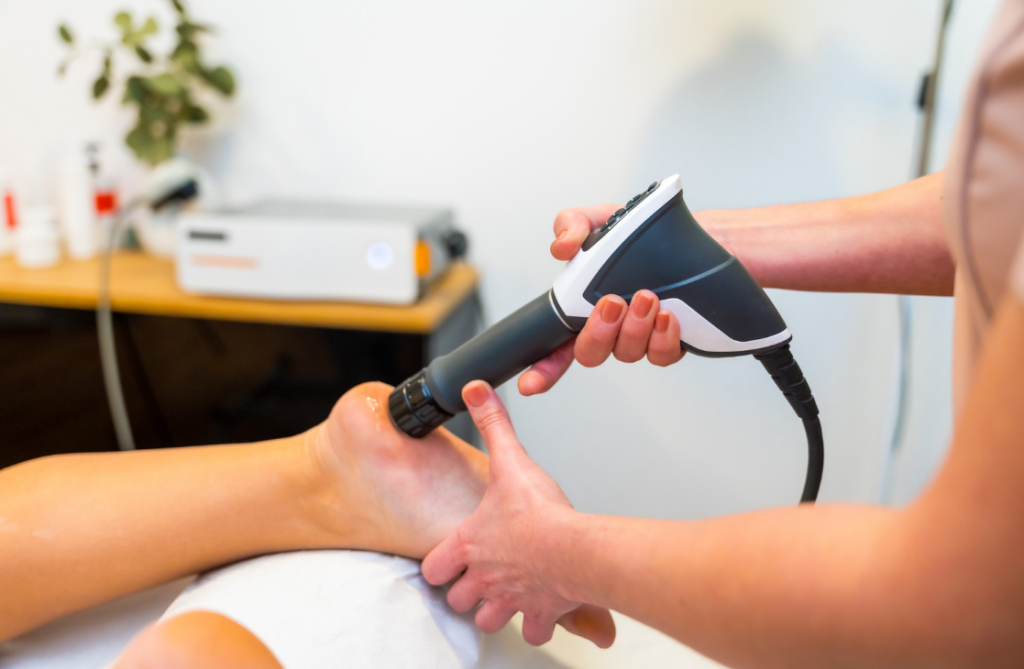
5. Strapping and Taping
If you’re looking for some immediate relief, strapping and taping techniques can be really helpful. Your physiotherapist can use specific taping techniques to support the arch of your foot and reduce the stress on your plantar fascia.
Taping isn’t a long-term solution, but it can provide temporary relief, especially if you’re dealing with a flare-up of pain. It’s also a good way to provide extra support during activities that might otherwise cause discomfort, like a long day on your feet or a workout session.
6. Tracking Steps
One of the reasons plantar fasciitis develops is due to overloading the plantar fascia. For many people, this comes down to simply taking too many steps in a day. Tracking your steps with a pedometer can be a helpful way to monitor your activity level and ensure you’re staying within a pain-free range.
Your physiotherapist can help you determine how many steps are appropriate for you based on your current condition. If you notice that your pain flares up after a certain number of steps, you can adjust your activity level accordingly to avoid overloading the plantar fascia.
Prevention Tips for Plantar Fasciitis
Once you’ve managed to get your plantar fasciitis under control, the last thing you want is for it to come back. Fortunately, there are several steps you can take to prevent future flare-ups:
Wear Supportive Footwear: Make sure your shoes provide proper arch support and cushioning. Avoid wearing unsupportive shoes like flip-flops or worn-out runners, especially if you’re going to be on your feet for extended periods.
Gradually Increase Activity: If you’re getting back into physical activity after a break, take it slow. Avoid rapidly increasing the intensity or duration of your activities, as this can place extra strain on your plantar fascia.
Maintain a Healthy Weight: Carrying extra weight puts more pressure on your feet, which can contribute to plantar fasciitis. Maintaining a healthy weight will reduce the load on your plantar fascia and help prevent future problems.
Stretch and Strengthen: Regularly stretching and strengthening your calf muscles can help reduce tension in your plantar fascia and prevent it from becoming irritated.
Conclusion
Plantar fasciitis can be a real pain—literally. But the good news is that with the right physiotherapy interventions and some lifestyle adjustments, relief is well within reach. If you’re dealing with persistent heel pain or discomfort along the arch of your foot, it’s time to take action.
Consult with a physiotherapist at XPHYSIO for a personalised treatment plan tailored to your specific needs. A proactive approach combined with targeted exercises and physiotherapy can make all the difference in overcoming plantar fasciitis and getting back to the activities you love.
As we age, it’s no secret that our bodies go through all sorts of changes. Most of these changes are completely normal, but when it comes to our muscles, joints, and bones, it’s easy to feel concerned—especially when you get a scan that highlights degenerative changes. The medical terminology on these scans can feel overwhelming, and often, the results don’t differentiate between normal, age-related changes and the possible causes of symptoms. This can lead to a lot of confusion and stress. It’s not uncommon for people to misinterpret their scan results, believing they are in worse condition than they actually are.
In this blog, we’re going to break down some common age-related degenerative changes, how to understand your scan results, and highlight the importance of working with a physiotherapist to properly interpret them. Plus, we’ll touch on some incidental findings—things that show up on scans but may not be as concerning as they sound.
The Complexity of Pain and Scans
Before we dive into the specifics, it’s important to understand that pain is a complex process. It’s our body’s natural defence mechanism, designed to protect us from harm. But here’s the tricky part: damage doesn’t always cause pain, and just because you feel pain, it doesn’t mean there’s necessarily damage.
Thanks to ongoing research, we now know that scans don’t always paint the full picture when it comes to pain. Studies comparing the scans of people with and without symptoms have revealed that many people walk around with some form of “damage” or pathology on their scans, but they experience no pain at all. In fact, many of these individuals go about their daily lives without any issues. This is where things can get confusing—just because something shows up on a scan doesn’t mean it’s causing your pain or needs to be treated.
Age-Appropriate Degenerative Changes: What’s Normal?
As we age, there are a few changes that naturally occur in our musculoskeletal system. These changes might sound scary when you see them listed on a scan, but the reality is that they’re a normal part of the aging process. Here’s a look at some common age-appropriate degenerative changes:
1. Joint Health
As we get older, the cartilage that cushions our joints naturally starts to wear down. This can lead to conditions like osteoarthritis, where the joints become stiff and painful. However, just because you see signs of wear and tear in a joint on your scan doesn’t mean you’ll experience symptoms. Many people have signs of joint degeneration on their scans but experience little to no discomfort.
2. Bone Density
Our bones naturally lose density as we age, which makes them more susceptible to fractures. This is why conditions like osteoporosis become more common in older adults. Decreased bone density can show up on a scan, but it’s something that can often be managed with diet, exercise, and, in some cases, medication.
3. Muscle Mass and Strength
As we age, we also lose muscle mass and strength—a condition known as sarcopenia. This loss of muscle can impact mobility and increase the risk of falls, but it’s a gradual process that can often be slowed or reversed with regular strength training and physiotherapy.
4. Posture and Alignment
Changes in our spinal discs and ligaments are a common part of aging, and these changes can sometimes lead to alterations in posture or spinal alignment. For example, you might develop a slight hunch or notice that your range of motion isn’t what it used to be. While these changes are normal, they can sometimes contribute to discomfort, which is why maintaining flexibility and mobility through exercise is key.
5. Flexibility and Range of Motion
As we get older, our connective tissues, like tendons and ligaments, become less flexible. This can lead to a gradual reduction in range of motion, which is why it’s so important to stay active and keep those muscles and joints moving.

Incidental Findings on Scans: What Do They Mean?
Now that we’ve covered some common degenerative changes, let’s talk about incidental findings—those things that show up on your scan that might sound alarming but are often completely normal. Here are a few examples based on common areas of the body:
1. Shoulder
A study conducted in 2013 looked at the prevalence of full-thickness rotator cuff tears across different age groups. They found that:
- 0% of people in their 20s to 40s had full-thickness tears.
- 10% of people in their 50s had full-thickness tears.
- 15% of people in their 60s had full-thickness tears.
- 36% of people in their 80s had full-thickness tears.
Interestingly, 65% of the people with rotator cuff tears didn’t experience any symptoms. That means that a significant number of people were walking around with these tears but were pain-free and functioning normally. If something like this shows up on your scan, it doesn’t necessarily mean it’s causing your pain or needs surgical intervention.

2. Knee
A study focused on individuals aged 50 to 90 looked at the prevalence of meniscal tears in this age group. The results showed:
- 19% of females aged 50-60 had meniscal tears.
- 56% of males aged 70-90 had meniscal tears.
What’s surprising is that only 61% of these individuals reported experiencing knee pain in the past month. This highlights that, while meniscal tears are common as we age, they aren’t always associated with symptoms.
3. Back
There’s been a lot of research done on back pain and how it correlates (or doesn’t) with scan results. A recent study showed that:
- 37% of pain-free 20-year-olds had evidence of disc degeneration on their scans.
- A whopping 96% of pain-free 80-year-olds had disc degeneration.
Again, this shows that degenerative changes in the spine are common as we age and don’t always result in pain. If your scan comes back showing disc degeneration, it’s important to remember that it’s a normal part of aging and may not be the root cause of any discomfort you’re experiencing.
Why You Are Not Your Scan
Here’s the takeaway: you are not your scan. Medical imaging is incredibly useful for diagnosing certain conditions, but it has its limits. Scans can pick up every little detail—things that may have been there for years without causing any issues. Just because something abnormal shows up doesn’t mean it’s causing your pain or needs treatment.
That’s why it’s so important to consult with a physiotherapist who can assess your symptoms, examine your scan results, and give you a comprehensive, real-world interpretation. A physio will be able to help you understand which findings on your scan are normal for your age and which ones might be contributing to your symptoms. They’ll also guide you through a treatment plan that’s focused on getting you back to feeling your best, without unnecessary worry about incidental findings.
Physiotherapy for Age-Appropriate Degenerative Changes
Physiotherapy is one of the best ways to manage age-related changes in your musculoskeletal system. Here are some of the interventions that a physiotherapist might use to help you stay active and healthy as you age:
1. Exercise Prescription
Staying active is one of the most effective ways to manage degenerative changes and maintain your overall health. A physiotherapist can design a tailored exercise program that includes strength training, flexibility exercises, and cardiovascular activities. This type of program will help you build muscle, maintain joint health, and improve your balance and coordination.
2. Pain Management Techniques
If you’re experiencing pain related to degenerative changes, a physiotherapist can use a variety of techniques to help manage it. These might include manual therapy (such as massage or joint mobilisation), heat and cold therapy, and even dry needling. The goal is to reduce pain while improving your overall function.
3. Balance and Fall Prevention
As we age, our risk of falls increases, particularly if we’ve lost muscle strength or balance. Physiotherapists can guide you through balance exercises and functional training to improve your stability and reduce your risk of falling. This is especially important for older adults, as falls can lead to serious injuries like fractures.
4. Joint Mobilisation and Soft Tissue Techniques
If joint stiffness or muscle tightness is limiting your range of motion, physiotherapists can use hands-on techniques to help. Joint mobilisation can improve the movement of stiff joints, while soft tissue techniques can address tight muscles and help you move more freely.
Conclusion
Aging is a natural process, and age-appropriate degenerative changes are nothing to fear. In fact, understanding these changes is the first step toward maintaining a healthy, active lifestyle well into your later years. Physiotherapy plays a crucial role in this journey, offering targeted interventions that can help you manage pain, maintain mobility, and stay strong.
Remember, the next time you get a scan back, don’t be alarmed by every detail. Work with one of our physiotherapists at XPhysio who can help you interpret the results and provide a clear path forward. By staying proactive and taking care of your body, you can enjoy a fulfilling, active life, no matter your age!
You could have sworn someone had just kicked you from behind as you fell onto your knees, immediately losing all power in your leg. But when you turned around, there wasn’t anyone in sight. A sharp pain shoots through your leg, and you reach down to feel a strange divot at the back of your ankle. That’s when it hits you—something’s gone seriously wrong. You’re already thinking, “This is going to need surgery, no question.”
But here’s the thing—you might be wrong!
Believe it or not, Achilles ruptures are now often treated without surgery, using early immobilisation instead. Recent studies have shown that there’s only a minimal difference in the re-rupture rates between patients who go the surgical route and those who opt for conservative management. It’s a pretty big shift in how this injury is treated, and if your specialist agrees that your case is suitable for non-surgical treatment, it could mean avoiding the risks and recovery time associated with surgery altogether. Not bad for an injury that many people assume automatically requires going under the knife!
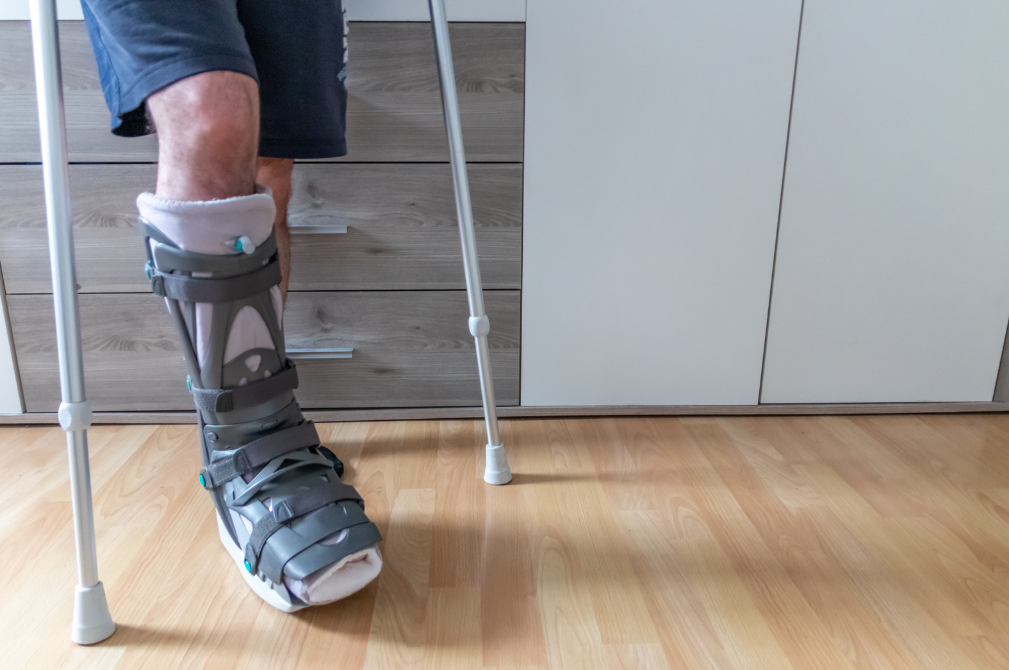
Understanding Achilles Rupture
Before we get into the nitty-gritty of treatment, it’s worth understanding a bit more about what an Achilles rupture actually is and how it happens.
Anatomy of the Achilles Tendon
The Achilles tendon is the largest and strongest tendon in the human body. It connects the calf muscles—specifically the gastrocnemius and soleus—to the heel bone (the calcaneus). This tendon plays a key role in everyday movements like walking, running, jumping, and even standing on your toes. Anytime you push off the ground with your foot, you’re engaging your Achilles tendon.
Because the Achilles tendon handles so much load and repetitive stress, it’s particularly vulnerable to injury. Ruptures occur when the tendon is suddenly overloaded, and the force is too great for the tissue to handle.
Cause
There are a few common scenarios where an Achilles rupture is likely to occur:
Sudden Forceful movements: This is often the culprit in ruptures, particularly during activities that involve a rapid change in direction or explosive pushing off. Think sports like basketball, football, tennis, or sprinting, where you need to go from stationary to full speed in a split second.
Chronic overuse: Over time, repetitive stress can weaken the Achilles tendon. This is especially common in athletes who don’t give their body enough time to recover between intense training sessions, or people who do a lot of walking or running on hard surfaces. Overuse creates micro-tears in the tendon, and over time, this wear and tear can lead to a full rupture.
Age and activity level: ruptures are more common in people aged 30 to 50, particularly those who engage in “weekend warrior” activities—high-intensity sports without proper conditioning or preparation. Tendons naturally become less elastic and more prone to injury as we age.

Symptoms of Achilles Rupture
Achilles ruptures are typically dramatic, and the symptoms aren’t hard to miss:
Sharp Pain: People often describe the pain of an Achilles rupture as feeling like they’ve been kicked or hit in the back of the leg. Some even hear a “pop” or “snap” when the tendon gives way.
Divot at the back of the ankle: If you feel a noticeable gap or divot where the Achilles tendon should be, that’s a classic sign of rupture.
Swelling and tenderness: The back of the leg and ankle will swell up fairly quickly after the injury, and the area will likely be very tender to the touch.
Difficulty walking: A ruptured Achilles tendon makes it extremely hard to push off your foot, making walking difficult. You may have a limp or find it impossible to bear weight on the injured leg.
Physiotherapy Interventions
If you’ve just experienced a rupture, you’re probably wondering what the next steps are. This is where a physiotherapist can make all the difference. Whether you end up going the surgical or non-surgical route, a tailored rehabilitation plan is crucial to ensure proper healing and to minimise the risk of re-injury.
Non-Surgical Management
More and more often, non-surgical management is being recommended for ruptures, especially for people who aren’t high-level athletes. The idea is that by immobilising the ankle and gradually increasing the range of motion and load through the tendon, the body can heal itself.
At XPHYSIO, we collaborate closely with a number of trusted orthopaedic surgeons. If you’ve been diagnosed with an Achilles rupture, we can arrange for you to be seen by a specialist who will help determine whether surgery is necessary or if non-surgical management is the better option. If non-surgical treatment is chosen, we would fit you with a VACOped CAM boot or a similar walker. These boots are designed to keep your foot at the right angle for optimal healing while allowing for adjustments over time as the tendon repairs itself.

Tip: These timelines are averages. Your progress may be faster or slower depending on your age, fitness, and the severity of the rupture. A physiotherapist will adjust your plan based on how your tendon responds.
Post-Surgery Rehabilitation
If surgery is necessary, rehabilitation becomes even more important. A physiotherapist will guide you through the post-surgical recovery process, ensuring that the tendon heals properly and regains its strength and flexibility.
Some key elements of post-surgery rehabilitation include:
Range of motion exercises: After surgery, the ankle is often stiff, and you’ll need to do gentle range-of-motion exercises to restore flexibility without putting too much stress on the healing tendon.
Strengthening Protocols: As you progress in your recovery, strengthening the muscles of the calf and the Achilles tendon is crucial. A physiotherapist will guide you through a gradual progression of exercises designed to rebuild strength without overloading the tendon too early.
Gait Training: After an Achilles rupture, walking normally can feel like a distant goal. A physiotherapist will work with you to retrain your gait and restore a natural stride, reducing the likelihood of compensatory movements that could lead to further injury.
Functional Exercises: These are exercises that mimic the movements you’ll be doing in your day-to-day life or sports activities. For example, if you’re a runner, your physiotherapist will incorporate exercises that prepare your Achilles tendon for the specific stresses of running.
Gradual Progression: The key to successful rehabilitation is a phased approach. Your physiotherapist will create a program that gradually increases the intensity and load on your Achilles tendon, ensuring that you don’t do too much too soon and risk a re-rupture.
To learn more about post surgery rehab, read out blog HERE
Typical Recovery Timeline For Both Conservative or Surgical
Whether you’re managed conservatively or after surgery, the broad principles of rehab are very similar. At XPHYSIO we individualise every program, but here’s what a standard evidence-based timeline often looks like:
- 0–4 Weeks: Non-Weight Bearing
In the first few weeks the goal is protection. The ankle is held in plantarflexion (toes pointed down) in a boot or cast to take stress off the healing tendon. You’ll usually be on crutches and non-weight bearing, although gentle toe wiggling and circulation exercises may be encouraged. - From 4 Weeks: Begin Partial Weight Bearing (up to 50%)
Once the tendon has begun to knit together, you can start carefully loading it. Most people move to partial weight bearing in the boot at about 4 weeks, using crutches for balance. This introduces controlled stress that stimulates the tendon to heal stronger. - 5–6 Weeks: Gradual Reduction of Plantarflexion
The boot angle is reduced by around 5 degrees every five days (or as instructed by your specialist). This slowly brings the foot closer to a neutral position, allowing the tendon to adapt to length changes without being overstretched. - By 9 Weeks: Achieving Full Plantar Grade
Around the 9-week mark, most people reach neutral (plantar grade) in their boot. This means the ankle is in a normal standing position and the tendon is tolerating a functional length. - 6–12 Weeks: Restoring Range of Motion
During this phase, gentle, supervised ankle mobility exercises are introduced. The aim is to restore normal dorsiflexion (bringing the foot upwards) and plantarflexion while respecting the healing tissue. - 12–20 Weeks: Strengthening Phase
As movement normalises, more active strengthening of the calf muscles begins—initially seated or isometric exercises, progressing to standing heel raises, balance work, and light functional drills. - 5–7 Months: Return to General Activity
Everyday activities like brisk walking, cycling, or gym work can usually be resumed gradually. Plyometric or high-impact exercise is still limited at this point however we are building your capacity for your chosen sport. - 8–12 Months: Return to Play/Sport
This is the period where advanced sport-specific conditioning occurs—running drills, cutting, jumping, sprinting. Return-to-play testing ensures your tendon strength and function are symmetrical and your risk of re-rupture is low.
Preventive Measures
Once you’ve fully recovered from an Achilles rupture, it’s important to take steps to prevent the injury from happening again. The Achilles tendon will be stronger, but it’s still vulnerable, particularly in the first year after injury. Here are some tips to keep your Achilles tendon healthy:
Proper Warm-up and Cool Down
This is something many of us skip, but it’s especially important after an Achilles rupture. Warming up properly increases blood flow to the muscles and tendons, making them more elastic and ready for exercise. Cooling down helps flush out lactic acid and promotes recovery. At XPHYSIO, we can provide you with a tailored warm-up and cool-down routine that suits your activity level.
Footwear and Equipment
Wearing the right shoes is another important preventive measure. Look for footwear that provides proper support for the arch of your foot and has good cushioning to reduce impact. If you’re an athlete, make sure your equipment (e.g. orthotics) is up to scratch and not worn out.
Cross-Training
Avoid doing the same type of exercise over and over, as this can lead to overuse injuries like an Achilles rupture. Instead, mix it up! Incorporate a variety of activities into your routine—swimming, cycling, yoga, strength training—to reduce stress on the Achilles tendon and work different muscle groups.
Conclusion
An Achilles rupture can feel like a devastating setback, especially if you’re active or involved in sports. But the good news is that with the right treatment, full recovery is achievable. Whether you go down the surgical or non-surgical route, working with a physiotherapist to create a personalised rehabilitation plan is critical to getting back on your feet—lit erally and figuratively.
At XPHYSIO, our team is here to help you through every step of your recovery. From initial diagnosis to rehabilitation and preventive care, we provide the support and expertise you need to make a successful comeback. With patience, dedication, and the right guidance, you’ll not only recover but come back stronger and more resilient than before.
So, if you’ve recently ruptured your Achilles or you’re experiencing symptoms that have you worried, don’t wait—reach out to a physiotherapist today and start your journey to recovery. You’ve got this!
References
Ochen Y, Beks RB, van Heijl M, Hietbrink F, Leenen LPH, van der Velde D, Heng M, van der Meijden O, Groenwold RHH, Houwert RM (2019). Operative treatment versus nonoperative treatment of Achilles tendon ruptures: Systematic review and meta-analysis. BMJ. 2019 364: 5120.
Ever felt that sharp jab of pain while reaching into the back seat of the car? Or maybe you’re gritting your teeth as you push through the last few lateral raises at the gym? That pesky discomfort could be shoulder impingement—a surprisingly common issue that can leave you frustrated and wondering when your shoulder will feel normal again.
Whether you’re an athlete, a tradie, an office worker, or someone who spends their days painting ceilings or gardening, shoulder impingement can sneak into your life and throw a spanner in the works. But don’t worry—there’s plenty you can do about it!
In this blog, the team at XPHYSIO will walk you through what shoulder impingement is, why it happens, and how physiotherapy can be your secret weapon to getting back to a pain-free, mobile life.
What is Shoulder Impingement?
Let’s start with the basics. Your shoulder is one of the most complex joints in the body, with a huge range of motion. But that flexibility comes at a price—it’s also prone to injury.
A Quick Anatomy Lesson
The shoulder is a ball-and-socket joint, with the ball at the top of your upper arm bone (humerus) fitting snugly into a shallow socket in your shoulder blade. To keep everything stable and moving smoothly, you’ve got a team of four muscles and their tendons called the rotator cuff. Think of these as the shoulder’s support crew.
Now, here’s where things can go wrong. Shoulder impingement happens when those rotator cuff tendons get squashed (or “impinged”) between the bones in the joint—specifically the acromion (a bony bit at the top of your shoulder) and the head of the humerus. This pinching can lead to pain, inflammation, and frustration.

Why Does Shoulder Impingement Happen?
Shoulder impingement can happen for a bunch of reasons, and often it’s a mix of several factors. Here are some of the big ones:
1. Repetitive Overhead Movements
Ever painted a ceiling, played heaps of tennis, or spent a weekend lifting things above your head? These kinds of activities can overwork the rotator cuff tendons, leading to wear and tear.
2. Poor Posture
Slouching at your desk, hunching over your phone, or sitting in awkward positions can mess with your shoulder alignment. Over time, this poor posture puts unnecessary stress on the rotator cuff.
3. Muscle Imbalances
If some of your shoulder muscles are weak while others are tight, it can throw off the way your shoulder moves, increasing the risk of impingement.
4. Structural Abnormalities
Some people naturally have a narrower space in their shoulder joint, which makes impingement more likely.
How Does Shoulder Impingement Feel?
Wondering if you might be dealing with shoulder impingement? Here are some of the classic symptoms:
Pain
- A dull, aching pain in the shoulder that gets worse with overhead movements.
- Sometimes, the pain radiates down your arm, especially when you’re reaching for something or lifting.
Weakness and Limited Movement
- You might find it hard to lift your arm or rotate it fully.
- Struggling to reach behind your back or out to the side is another telltale sign.
How Physiotherapy Can Help
Here’s the good news: shoulder impingement is absolutely treatable, and physiotherapy is one of the most effective ways to tackle it. At XPHYSIO, we take a personalised approach to get you moving pain-free again. Here’s how:
1. Thorough Assessment
We start by digging deep into what’s causing your pain. A physio will assess your:
- Posture: Is slouching a factor?
- Strength: Are some muscles pulling their weight while others slack off?
- Mobility: How’s your range of motion looking?
- Biomechanics: Are your movement patterns putting extra stress on your shoulder?
This detailed assessment helps us tailor a plan just for you.
2. Pain Management
Before jumping into strengthening or stretching, it’s essential to get your pain under control. We might use techniques like:
- Manual Therapy: Hands-on treatment to ease tension and improve movement.
- Massage and Joint Mobilisations: To reduce stiffness and improve blood flow.
- K-Taping or Strapping: For extra support and to limit painful movements.
- Education: Understanding which movements to avoid and how to move better.
3. Strengthening Exercises
Weak muscles are often a big part of the problem, so we focus on strengthening your rotator cuff and the muscles around your shoulder blade. This helps stabilise the joint and prevent future issues. Some common exercises might include:
- Shoulder external rotations with resistance bands.
- Scapular retraction exercises (to strengthen your shoulder blade muscles).
- Gradual progressions to ensure pain-free improvement.

4. Stretching and Flexibility
Tight muscles can pull your shoulder out of whack, so stretching is another key piece of the puzzle. Gentle stretches or even self-massage techniques can work wonders in improving flexibility and preventing further tightness.
5. Posture Correction
Bad posture is a major player in shoulder impingement, so we’ll help you become more aware of how you’re sitting, standing, and moving throughout the day.
- For desk workers: Adjusting your chair, desk height, and screen can make a massive difference.
- For drivers: Pay attention to how you’re sitting in the car to avoid slouching.
6. Biomechanical Analysis
We’ll take a closer look at how you move, whether that’s your gym technique, the way you lift at work, or how you throw a ball. Identifying and fixing any abnormal movement patterns is crucial for preventing future problems.
7. Activity Modification
Sometimes, it’s as simple as tweaking the way you do things. If certain movements or activities are making your pain worse, we’ll guide you on how to adjust them without completely giving them up.
Preventing Shoulder Impingement
Once you’re feeling better, it’s important to keep those shoulders healthy. Here are some tips to prevent impingement from making a comeback:
1. Nail Your Technique
Whether it’s lifting weights at the gym or doing DIY projects at home, using the correct form is key to avoiding shoulder strain.
2. Keep Your Shoulders Strong
Incorporate regular shoulder-strengthening exercises into your routine to maintain stability and mobility.
3. Stretch it Out
Don’t let your muscles get tight! Make stretching a habit, especially if you’re spending long hours at a desk.
4. Set Up Your Workspace
An ergonomic workspace isn’t just about comfort—it can save your shoulders too. Make sure your desk and chair are set up to promote good posture.
Final Thoughts: Take Control of Your Shoulder Health
Shoulder impingement might be common, but it’s definitely not something you have to live with. Reach out to us today and with the right mix of physiotherapy, strengthening, and lifestyle adjustments, you can wave goodbye to shoulder pain and get back to doing what you love.
At XPHYSIO, we’ve helped countless people reclaim their mobility and live pain-free. So, if your shoulder’s giving you grief, don’t wait—book an appointment with us today. Let’s work together to improve the way you move! Our number is 9806 3077, give us a call now to get started.
